Document Navigation
About
In 2022-23 the University of the Sunshine Coast (Unisc) conducted a comprehensive 12 month evaluation of the Community Based Palliative Care Model that Little Haven has developed in the Gympie region over the past 40 years.
To view all the report findings jump straight to the Executive Summary, Section 3 – Evaluation Findings and Section 4 – Discussion. All the other sections are for the evaluation scope, reference, and context.
Key findings of the report highlight the service model’s strengths (Section 4.5), including but not exclusive too, early access (Section 3.6.2.1), specialist staffing (Section 4.2.3.1), a patient and family-centered approach (Section 3.6.3.1) with holistic care (Section 3.6.1) and community involvement (Section 3.6.7).
The reports economic evaluation conclusion recommends that:
State and national funding bodies should strongly consider further investments in community-based palliative care services, such as Little Haven, as this example has shown the excellent return on investment and value for money, in addition to providing high-quality care with outstanding client satisfaction and a person-centred model of care. (Section 3.3.4) .
The major challenges identified in the report were securing an ongoing and sustainable government funding model (Section 3.3.4) and adapting to changing volunteering patterns (Section 3.7.5). The report suggests potential improvements and considers the model’s replicability in other settings, emphasizing its community-based, holistic approach to palliative care.
Report Cover

A service and economic evaluation of
Little Haven Palliative Care Service’s model of care.
University of the Sunshine Coast
90 Sippy Downs Drive, Sippy Downs QLD 4556 www.usc.edu.au
13/4/2023 version 3
Evaluation Team:
Chief Investigator and key contact:
Dr John Rosenberg RN PhD, School of Health. Senior Lecturer, palliative care researcher. Project Lead.
T: +61 7 5430 2922 | jrosenbe@usc.edu.au
Co-investigators:
Prof. Cindy Davis BS (Psych Hons) MSW PhD, Professor, School of Law and Society. Discipline Lead, Social Work.
Dr Trudi Flynn BA (Psych Hons) PhD, School of Law and Society. Program Coordinator, Master of Counselling
program. Counsellor.
Ms Josie Linn BSci(Hons) MCouns, School of Health. Research Assistant.
Dr Katharina Merollini PhD, School of Health. Lecturer & Health Economist.
Mrs Doreen Nabukalu MPH, School of Health. Research Assistant.
Declaration:
This evaluation was commissioned by Little Haven Cooloola Sunshine Coast Palliative Care Association Inc. to be undertaken by the University of the Sunshine Coast for which payment was provided.
Download Paper
If you would prefer to download the entire research paper you can do that here. It is in .PDF format and the file is just 2.61MB.
Executive Summary
Evaluation aim
This evaluation was commissioned by Little Haven Cooloola Sunshine Coast Palliative Care Association Inc. [hereafter “Little Haven”] and conducted by a multidisciplinary research team from the University of the Sunshine Coast [UniSC].
The evaluation aim is to identify the extent to which Little Haven’s model of care meets their goals for service provision and community engagement and provides efficiencies in the utilisation of health care services. These goals are to provide the delivery of the highest quality of care, support and education for those experiencing or anticipating serious illness and loss in the Gympie and surrounding region. This evaluation includes examination of organisational structures, processes and outcomes, and economic costs and benefits.
Exploring these components enables the identification of key components of Little Haven’s model of care and informs consideration of the replicability of the model in other settings.
Evaluation approach
A co-designed approach to the evaluation was implemented to address the aims identified above. Ethical approval was granted by the University of the Sunshine Coast Human Ethics Research Committee.
A comprehensive range of data sources was obtained, comprising organisational documentation including financial data; peer reviewed publications and grey literature; qualitative in-depth interview data from current patients and current and bereaved carers, and key stakeholders; qualitative focus group data from staff, volunteers; and mixed method carer satisfaction data. These data were analysed using an established analytical framework designed for the evaluation of structures, processes and outcomes of healthcare organisations.
Evaluation outcomes
Review of the peer-reviewed and grey literature identified seven key components of community-based palliative care that were clearly evident in Little Haven’s model of care:
- Accessibility of service
- Specialist staff
- Early intervention
- Patient- and family-centred approach
- Holistic care
- Community involvement
- Free to low-cost services
Identifying how these components are configured and operationalised in the Little Haven model of care was essential to ascertain the extent to which the model meets the goals for service provision and community engagement and provides efficiencies in the utilisation of health care services.
Overview
Little Haven is clearly regarded as the provider of a very high standard of clinical care and other aspects of holistic care needs. The multidisciplinary clinical staff are seen to be pivotal in this, and the notion of going ‘above and beyond’ was clear. Similarly, the volunteers are regarded as essential to the work of Little Haven and at no time was there any indication of hierarchical views of ‘staff versus volunteers.’ Patients and carers prospectively and retrospectively report high satisfaction not only with the type of services received, but the ways in which these services are delivered. Other service providers are largely supportive of Little Haven’s model of care, particularly those GPs who work most closely with them in shared care arrangements. Where there are multiple services engaged in care, Little Haven undertakes a care-coordination role which is essential in the support of patients and their families and carers. Recognising the necessity for self-care in palliative care practice, Little Haven’s staff support strategies are outstanding and clearly enable the challenges of PEoLC provision to be addressed.
Structural components
The configuration of organisational elements in the Little Haven model of care is clearly ordered around its stated goals. A notable structural component of the model of care as it enables local – rather than centralised – governance of the service, suiting its size and location and demonstrating a powerful connection to the community it supports. Little Haven is currently in a strong financial position however its reliance upon Government funding for its continued operation represents a risk for the organisation. Previous increases in government funding have addressed a wages shortfall, rather than underpinning growth. It is not clear how current government funding models could support all components of Little Haven’s model. Fundraising efforts are critical and are well-supported by the Gympie community, again reflecting powerful and reciprocal ties.
The organisational prioritising of holistic, person-centred care including care for carers and after bereavement is fundamental to its provision of care. Plans for the establishment of a hospice building reflect a growth mindset that is responsive to community expectations. Strong interdisciplinary and interagency links are found with Gympie Hospital and the wider SCHHS, GPs and generalist home-based care providers. Its volunteer program is resisting a wider trend in volunteering of high attrition and low recruitment, due in no small part to the role Little Haven holds as a ‘citizen organisation’ in the region. Volunteers are valued and report tremendous reward in the work they do.
Process components
The operationalisation of these structures into processes that aim to achieve the organisational goals of the Little Haven model of care is where it most clearly demonstrates excellence. Early admission is an uncommon practice in palliative care primarily due to funding constraints, with admission usually limited to those with a likely prognosis of three to six months. Provision of care early in the disease trajectory is linked to improved end-of-life outcomes, and at Little Haven, patients are accepted at time of referral regardless of their diagnosis, prognosis, or personal circumstances. The capacity of Little Haven staff to work very flexibly with patients and carers across time in response to constantly changing needs is a strength of the model.
As noted, Little Haven’s model of care is embedded deeply within its community, and it upholds its responsibility to that community. The efforts put into community engagement are a key part of Little Haven’s place as both a provider of services and a citizen organisation in the region. There were mixed views about the extent of community awareness of Little Haven in Gympie and surrounds; the Marketplace shopfront and fundraising were seen to be pivotal touchpoints between Little Haven and the community; each was seen to promote awareness not only of Little Haven but of broader issues encountered regarding life-limiting illness, caregiving, and grief. These were further promoted through the range of public activities Little Haven leads.
Outcome components
The products resulting from the structures and processes of the model of care demonstrate the extent to which Little Haven meets its goals of care. A high degree of congruence exists between the tenets of compassion, care and support within the model, as offered to patients and carers, and the caring orientation of management, staff and volunteers towards each other. This is a service and a model that recognises itself to be situated deeply within its community and upholds its responsibility to that community.
Little Haven is a well-run community service and, for as long as QH or other government funding can be secured in the future, it is in a strong financial position. Many of the financial benefits of its model of care are evident including lower health care costs, and reduced health system costs if provided early. Community-based palliative care services provided by Little Haven enables individuals to receive care in their preferred location (in most cases their home), whilst reducing time spent in hospital (4.5-7.5 days less) and fewer emergency department presentations (2-13% less) in the last year of life.
Fulfillment of patients’ preferred place of care and death is an important outcome measure and Little Haven is a strong advocate of fulfilling clients’ needs; in fact, ~90% of their clients died according to their wishes. The presence of community-based palliative care services transfers a significant care burden that reduces the pressure on hospitals and the health system, however family carers often carry a greater care burden as a result, and the availability of community-based palliative care is reported to have carers subsequently experience greater sense of support and, ultimately, less complicated grieving. Over 90% of bereaved carers report they were ‘Extremely Satisfied’ with Little Haven services.
For staff, there is strong confidence and belief in the Little Haven model of palliative care. Job satisfaction is high and burnout with subsequent attrition is remarkably low. Like their counterparts in the staff, Little Haven’s volunteers describe enormous satisfaction drawn from their contributions to the service. They see it as both valuable and valued, and understand it to be contributing both to the immediate needs of families and the betterment of the local communities it supports. The current recruitment and retention trends for Little Haven are sufficient for current demand, although given the nature of volunteering itself, it is not clear whether Little Haven will continue to buck the trend widely observed elsewhere.
Reflecting its deeply embedded quality, the Little Haven model may not be able to be separated as a distinct entity from the community in which it has developed. Its structures and processes are both derived from community need and inform community awareness. In this sense, it is a ‘organisational citizen’ more so than simply a service provider, and this speaks to a critical quality of difference for the organisation. In return for the community investment – both social and financial – in it, Little Haven provides members with holistic, immersive, multidisciplined, high standard palliative care, free of financial cost to the patient and their family.
Summary
This evaluation the Little Haven model of care enables the identification of key components of Little Haven’s model of care and informs consideration of the replicability of the model in other settings. These components are highly contextualised, and reflect the structure-process-outcomes elements noted above, including:
- Offers a notably early point of engagement post-diagnosis with patients than is broadly practiced in the palliative care sector.
- Is highly flexible in its capacity to meet patient needs on a day to day and overarching basis, and in its support of patient preferences.
- Provides high levels of support for family and carers.
- Integrates care coordination.
- Offers new nursing staff a substantive time to orient to the Little Haven model of care with a one month mentoring process.
- Demonstrates high rates of staff retention and longevity
In this context of excellent service delivery, there are only a few issues to summarise for Little Haven’s consideration as it continues to evolve and respond to these data and other continuous improvement outcomes:
- Securing ongoing funding is clearly an ongoing concern for Little Haven considering current approaches to funding of community-based palliative care. The affordability of Little Haven’s model includes, but goes beyond, an equation of costs for service delivery; it also rests on value for money achieved through its model of care and measured by the critical flow on effects to the health, social and economic outcomes.
- It is reasonable to believe that the volunteering program will be impacted upon by changing social cohesion and volunteering patterns, despite its current stability. An investigation of how other programs are optimising this transition could inform Little Haven’s medium-term planning. Approaches to citizenship based on public health palliative care are found globally that might add value to evolving understanding of community engagement with Little Haven’s work.
- Although liaison with GPs is reported positively by those participating in this evaluation, structural and practice constraints are present that may impact upon Little Haven’s operation. Whilst there are systemic workforce issues relating to General Practice in the region (and beyond) which exceed Little Haven’s remit, its continued attention to sustaining existing, and building new, relationships with GPs in the region is essential.
- It is not clear from this evaluation whether an Aboriginal Health Worker is available for indigenous clients, or if indeed, indigenous people requiring palliative care seek Little Haven’s support. This might be considered when indigenous families receive support from Little Haven in partnership with
culturally appropriate services. - Similarly, it is not clear whether people experiencing, or at risk of homelessness, receive care from Little Haven, whether singly or in collaboration with other services specialising in this area. It is noted that those living alone do successfully receive care from Little Haven.
- There are observed barriers to accessibility to allied health and complementary therapies either due to location or declining health, meaning that attending Little Haven premises is not always possible. Carers raised the question whether these could be provided in-home.
- Succession planning is also part of Little Haven’s view of the future. Like many small, community-based organisations, Little Haven has a champion in its CEO, Sue Manton. She is very much the public face and voice of Little Haven and is acknowledged by many as the primary driving force behind its success and sustainability. It is acknowledged that the CEO will one day no longer be in the role, and the Board is cognizant of this, particularly in light of her substantial role in public promotion of the Little Haven model of care and funding opportunities.
Transferability of the Little Haven model of care
Under-resourcing and physical distances to health and social care services can impede access to specialist palliative care and it is recognised that regional and rural communities can have PEoLC needs distinct from metropolitan communities. This goes beyond the resources required in such communities to the character of the community itself, as noted above.
Where there are cohesive communities with a strong sense of identity and healthcare providers who not simply provide a service but are a clear ‘citizen’ of the community, partnerships between them can attend both to holistic care needs of patients and families and the broader social character of the community in addressing the issues of dying, caregiving, death and grief. It is clear in this evaluation that this characteristic permeates throughout Little Haven’s model and is a significant organisational quality at the very foundations of its presence in the Gympie community.
Whether the Little Haven model could be replicated in other settings is a complex matter requiring judicious consideration of local context. Its structures certainly support duplication, and many of its process would permit very positive outcomes to be achieved. The qualities and capacity of local communities, the proximity and relationship of other health care services, and the availability of appropriately qualified staff and engaged volunteers may demonstrate significant differences; the replication of the Little Haven model would, to a great extent, support the development of local community-based palliative care services in other regional centresat the very least. Its transferability into metropolitan or larger regional settings would appear to highly depend on contextual factors rather than simply workforce availability in these populated areas.
On behalf of the research team,

Dr John Rosenberg PhD RN
Chief Investigator | Nursing Discipline | School of Health | University of the Sunshine Coast
Tel: 07 5430 2922 | e: jrosenbe@usc.edu.au
Thursday, 13 April 2023
1. Introduction
1.1 Context
Little Haven Cooloola Sunshine Coast Palliative Care Association Inc. [hereafter “Little Haven”] is a community-based specialist palliative care and bereavement support service based in Gympie, Queensland. Its stated goals are to provide the delivery of the highest quality of care, support and education for those experiencing or anticipating serious illness and loss in the Gympie and surrounding region.(1)
A stated hallmark of Little Haven’s model of care is the recognition of the value of families and communities working alongside clinical services, and the influence community engagement has on compassionate care and support of dying people, their families and communities. In addition to the provision of specialist, interdisciplinary, clinical palliative care, Little Haven promotes early intervention, support of patients during active treatment, and allied health and psychosocial support. These holistic approaches enable optimal independence and planning for anticipated care needs as health declines, and before crises occur, if possible.
Further, this early intervention approach in the provision of palliative and end-of-life care [PEoLC] may enable a reduction in the avoidable transfer of home-dwelling patients to hospital during their palliative care, which in turn can result in better patient and carer experiences, and efficiencies in the cost of health care (Youens & Moorin, 2017). Several economic evaluations of palliative care exist demonstrating the value of community-based models of care (Gardiner et al., 2017; Yosick, et al., 2019).
It is also acknowledged that regional and rural communities can have PEoLC needs distinct from metropolitan communities (Spelten et al., 2019). Although some greater community cohesion can be present, under resourcing and physical distances to health and social care services can impede access to specialist palliative care; the need for knowledgeable, skilled and engaged communities is critical. Through its community engagement, Little Haven provides care for the partners and families of patients during the care of the dying person and after their death. This bereavement support is a substantial part of Little Haven’s model of care.
1.2 Aims of evaluation
This evaluation was commissioned by Little Haven to the University of the Sunshine Coast (UniSC) and seeks to understand the broader contexts in which Little Haven operates and identify the extent to which Little Haven’s model of care meets their goals for service provision and community engagement and provides efficiencies in the utilisation of health care services. This includes examination of organisational goals, structures and functions, clinical and social outcomes, and economic costs and benefits. This further enables the replicability of Little Haven’s model of care to be considered.
1.3 Structure of report
To report on the evaluation process, this Report is divided into these sections:
- Executive Summary
- Introduction
- Evaluation Design and Methods
- Evaluation Finding
- Discussion
- References
- Appendices
1.4 Expected outcomes
This evaluation undertook a detailed examination of Little Haven’s model of care, particularly focusing upon service provision, economic cost/benefits, lived experience and community engagement. It includes comparison with similar models in comparable settings.
This Final Report is provided as required by the Agreement between UniSC and Little Haven.
UniSC will implement dissemination strategies including the development of several manuscripts for publication in peer-reviewed scholarly journals and conference presentations.
This evaluation may be utilised by Little Haven in its liaison with government, health services including other palliative care service providers, and the local community.
1.5 Abbreviations
| ACP | Advance Care Planning |
| AHW | Aboriginal Health Workers |
| AIHW | Australian Institute of Health and Welfare |
| EoLC | End-of-life care |
| HREC | Human Research Ethics Committee |
| Little Haven | Little Haven Cooloola Sunshine Coast Palliative Care Association Inc. |
| NHHRC | National Health and Hospitals Reform Commission |
| PCOC | Palliative Care Outcomes Collaborative |
| PEoLC | Palliative and end-of-life care |
| QH | Queensland Health |
| RACFs | Residential Aged Care Facilities |
| SCUH | Sunshine Coast University Hospital |
| SCHHS | Sunshine Coast Hospital and Health District |
| UniSC | University of the Sunshine Coast |
| WHO | World Health Organization |
2. Evaluation Design and Methods
2.1 Design
2.1.1 Co-design methodology
To provide a co-designed evaluation approach, the following framework was implemented. As a process, it enables stakeholders to contribute to role clarification and communication protocols, agree on specific evaluation objectives and methods, and inform an ongoing plan for evaluation and research within the partnership.
The framework is comprised of eight steps:
- Establishment
a. Meet leadership group: UniSC and Little Haven.
b. Confirm objectives, timelines, outcomes and outputs for evaluation.
c. Agree on communication and reporting protocols, including research-related outputs.
d. Agree on roles of leadership team members.
- Review program material
a. Review organisational documentation and relevant materials (eg: policy, plans, statistical data, stakeholder information, etc.).
b. Review published and grey literature.
c. Develop concept map including assets and gaps in current models of care.
- Develop evaluation criteria and questions
a. Develop and verify evaluation criteria and questions.
b. Identify both retrospective and prospective data sources.
c. Determine repeatable data collection and analysis methods.
d. Develop and verify data management protocols.
e. Develop and submit application for Ethics Approval to UniSC Human Research Ethics
Committee.
- Collect data
a. Collect data from multiple sources (identified in 3.b).
b. Utilise data management systems to ensure integrity and confidentiality (identified in 3.d).
- Analyse results
a. Analyse data utilising appropriate method/s.
b. Synthesise results and findings.
- Develop conclusions and recommendations
a. Finalise conclusions and recommendations.
- Prepare and deliver evaluation report
a. Draft report and submit for review by leadership group.
b. Finalise report and submit to organisational leadership and collaboration members.
- Prepare material for dissemination
a. Draft and submit manuscript/s for submission for publication in peer-reviewed, scholarly
journal/s.
2.1.2 Program logic
The evaluation design shown in Figure 1 below demonstrates the program logic derived from the co-design.
Figure 1: Program logic

2.1.3 Donabedian’s Structure-Process-Outcome framework
As noted in Figure 1 above, the Donabedian framework with the multiple sources of data and their initial analysis to be synthesised in a way that provides an overall evaluation of organisations (Donabedian, 1980,2003). In this evaluation project, the following working definitions were applied:
- Structure: the configuration of organisational elements that enable achievement of organisational goals, regulate the influence of individual variations of the organisation, and facilitate the exercise of responsibilities related to roles. It is the ‘arena’ for organisational action.
- Process: the operationalisation of these structures to achieve organisational goals.
- Outcomes: the products resulting from the configuration and operationalisation, such as the extent to which fulfilment of organisational goals is achieved, or even the failure to do so (adapted from Rosenberg, 2007).
2.2 Background
2.2.1 Palliative Care
Palliative care, considered by the World Health Organization [WHO] as a human right, aims at improving the quality of life for patients and their families who are facing life threatening illness and their families through preventive and treatment measures that relieve pain, reduce suffering, improve psychosocial and spiritual health (WHO, 2020). The Australian definition underscores consideration of all patients with active and advanced life limiting illness evidenced by a documented individualised multidisciplinary assessment and management plan, delivered, or informed by a clinician with expertise in palliative care (Australian Institute of Health and Welfare [AIHW], 2022).
The need for palliative care is significant, with WHO estimating about 26 million people need palliative care each year (WHO, 2020). In the Australian context, given approximately 160,000 annual deaths, it is estimated that 75% would benefit from palliative care (Palliative Care Australia [PCA], 2018). In the financial year 2019-2020, hospitalisation related to palliative care was 8,700, of which 52% were related to cancer diagnosis (Blanchard et al., 2022).
Generally, early provision of palliative care improves end of life outcomes, such as alleviating the symptom burden (Baumann et al., 2015), reduced pain (Mularski et al., 2009), improved satisfaction with care (Gade et al., 2008),reduced ICU use (Romanò et al., 2017) and reduced length of hospital stay (Trtchounian et al., 2017). The settings in which palliative care is provided vary across different regions in Australia, mainly comprised of specialist inpatient facilities, general medical practice, specific departments like paediatrics, residential aged care facilities [RACFs], hospices and community/home settings (PCA, 2018).
2.2.2 Preferred place of death
Dying at home is a preference for at least 80% of people who have never experienced palliative care (Arnold et al., 2015). In Australia, about 60-70% of people are estimated to prefer to die at home regardless of age (Swerissen, 2014). A systematic review conducted in 2013 assessed the changes in this preference over time and concluded that about 80% of patients do not change their preference as the disease progresses (Gomes et al., 2013a). This preference is also evident amongst caregivers and families of palliative care patients (Woodman et al., 2016).
Early in 2009, the National Health and Hospitals Reform Commission [NHHRC] recommended increasing investment in services directed towards increasing palliative care at home or in community settings to enable patients achieve their desired wish of dying at home close to their families (NHHRC, 2009). According to the Australian Palliative Care Outcomes Commission in 2021, there are no clear estimates of community palliative care deaths. However, it was reported that about 33% of deaths occurred in private residential facilities and RACFs (Blanchard et al., 2022).
2.2.3 Community-based palliative care services
Despite the limited data on palliative care provided outside formal hospital settings, a substantial number of people still receive palliative care within community settings. According to the Palliative Care Outcomes Collaborative [PCOC] report (2022), about 52% of reported palliative care patients were dwelling in the community, during symptomatic episodes and the phases of care (Blanchard et al., 2022). This underscores the significance of community-based palliative care despite the inadequate data in national palliative care reports.
The literature suggests that receiving palliative care in the community increases the likelihood of death occurring at home (Shepperd et al., 2016; Ventura Mde, 2016). Patients receiving home-based palliative care generally have reduced demand for hospital-based care (such as Accident and Emergency Department visits) and show lessened symptom burden, compared to those receiving usual care; this impact is felt by family caregivers who subsequently experience less complicated grieving (Aoun & O’Connor, 2014; Bajwah et al., 2020; Gomes et al., 2013b; Gomes et al., 2014; Ping, 2014). Compared to usual care and services, there is evidence for improved health-related quality of life among patients receiving home-based palliative care (Brännström & Boman, 2014; Shepperd et al., 2016).
2.2.4 Models of care
In Australia, specialist palliative care providers are at the forefront of the current models of palliative care in both hospital and community settings. Specialist palliative care teams, often part of regionalised health services and major hospitals, extend their services to some community settings, including RACFs, hospices, community, and outreach services closer to patients’ dwelling places (PCA, 2018). Other specialist palliative care services are from the not-for-profit and charitable sectors. Common elements in these models of care are illustrated in Figure 2 and include:

- Accessibility of service: access to services is mainly through provision of home visits, provision of afterhours care, 24-hour phone support, provision of care on demand, and operating day care centres (Kilonzo et al., 2015).
- Specialist staffsuch as palliative care nurses: as noted by Gomes and colleagues(2013b), being staffed with specialist palliative care teams gives community palliative care a distinct advantage compared to general home care.
- Early intervention:some organisations demonstrate in their models of care that they support patients early after diagnosis and sometimes during active treatments, such as chemotherapy. This approach is considered very effective in improving patients’ outcomes (Pellizzari et al., 2017).
- Patient- and family-centred approach: services encourage non-professional team members such as friends, family members, volunteer community members, and spiritual/faith leaders to provide in any way they can. This enables people to spend their last days in the company of those who are important to them.
- Holistic care: in community-based models, care goes beyond the physical health of a person and involves spiritual and psychosocial support, bereavement counselling and other services, such as advance care planning and complementary therapies, in addition to medical, nursing, and allied health services, with noted benefits to patients (Gomes et al., 2013b).
- Community involvement and other non-professional staff: services may have teams of community volunteers, such as respite carers and pastoral carers, who are actively involved in the support of patients, fundraising activities and spiritual care.
- Free to low-cost services: most of the organisations are not-for-profit and provide free services, including equipment hire.
Figure 2: Common elements of models of care

2.2.5 Cost effectiveness of community-based palliative care
The economic value of palliative care cannot be underestimated. Regardless of the settings of care, from the provider’s perspective, palliative care is associated with lower health care costs (Abian et al., 2022; Brereton et al., 2017; Smith et al., 2014), reduced health system costs if provided early (Seow et al., 2022), and has been found to be very cost effective when managing some health conditions like heart failure (Kaufman et al., 2021). Further, in patients with non-malignant illnesses, palliative care is associated with reduced health service utilisation, including reduced emergency department presentations and hospital admissions (Quinn et al.,2020).

Due to these reduced emergency presentations (Delgado-Guay et al., 2015) and hospital stays (Spilsbury & Rosenwax, 2017), a general reduction in the demand of health care services for people who opt for home-based palliative care, and health care costs more generally, are often lower compared to usual care (Luta et al., 2021). The cost-effectiveness of some home-based models, such as person-centred integrated heart failure care and home palliative care, were found to be very cost effective (Sahlen et al., 2016).
With an increasingly ageing Australian population, the demand for palliative care will substantially increase over time. In their recent paper, Lam et al., (2021) highlight the importance of strengthening community palliative care to reduce the reliance upon hospital resources. Community-based palliative care transfers a significant care burden that reduces the pressure on hospitals and the health system. This evaluation of the feasibility and cost benefit of Little Haven’s model of care illustrates the role of community-based palliative care organisations in meeting patients’ expectations of dying at home.
2.3 Ethical considerations and approval
Approval to conduct this evaluation was granted by the Human Research Ethics Committee (HREC) of the University of the Sunshine Coast (Approval #A221806). The letter of approval is found in Appendix 1: Ethics approval.
2.3.1 Use of documents
Documentation in the public domain was identified and retrieved. Consent was given by Little Haven to access relevant non-confidential internal reporting including the use of organisational documentation not already in the public domain, to enable organisational and economic evaluations.
2.3.2 Human participants
All participants were provided with a targeted Research Participant Information Sheet and Consent Form to facilitate voluntary participation (see Appendix 2: Suite of Research Participant Information Sheets and Consent Forms). It was clearly communicated to all participants that their participation (or not) in data collection would not disadvantage them in their relationship with Little Haven, whether it is their service provider or employer, or in a stakeholder relationship. Participants were informed that they were free to withdraw from the study at any time. Written consent was obtained from all participants and stored securely.
Regarding the participation of palliative care patients and carers in research, individual patients and carers provided their own consent for their own participation; carers could not provide proxy consent for the patient. People receiving palliative care are recognised as having capability to consent to their own clinical treatment, even at advanced stages of illness progression (Chatland et al., 2023); although interviews were not conducted with individuals in the final stages of illness, their potential capacity to consent is acknowledged.
Risk assessments are routinely undertaken by Little Haven upon admission to the service, and this information was accessible to the co-investigator conducting patient, family and carer interviews. This researcher is very familiar with the client base as an experienced community counsellor, and managed risk relating to participant distress.
2.3.3 Waiver of consent for existing dataset
A waiver to consent was granted by the HREC in relation to data derived from the Carer Satisfaction Survey. At the time of administration by Little Haven, respondents consent to current and future use of the data within Little Haven. As all of the data are submitted anonymously, it was not possible to deidentify them to determine who completed the surveys. Survey responses were downloaded to an Excel file and transferred to SPSS™ for statistical analysis.
2.4 Data management
Data were managed according to the UniSC Data Management policy and procedures, and confidentiality was maintained. Electronic files are stored on a centralised, secure, password protected UniSC electronic hard drive. Hard copy documents are stored in a securely locked filing cabinet at a UniSC campus. Identifying information is stored separately from the deidentified interview and focus group transcripts. Access to the data is restricted to members of the research team. All data will be stored for five years following completion of the project, or five years following the publication of the research (whichever is the latest), in accordance with the Australian Code for the Responsible Conduct of Research. The data will be disposed of in accordance with these requirements.
2.5 Data collection and analysis
Data were collected in line with the Program Logic noted in Figure 1. Data sources were:
- Documentary sources:
a. Peer-reviewed publications.
b. Organisational documents and grey literature pertaining to service delivery at Little Haven and in broader healthcare contexts.
c. Economic data relating to service delivery costings. - Qualitative in-depth interview data provided by current patients and current carers, or bereaved family members/carers.
- Qualitative focus group data provided by employees and volunteers and qualitative in-depth interview data provided by key stakeholders.
- Anonymous mixed-method Carer Satisfaction Survey data from an existing dataset held by Little Haven.
These data sources and the analytical methods applied to them are discussed in the subsections below.
2.5.1 Peer-reviewed literature
A review of peer-reviewed literature was undertaken to identify published literature on community-based palliative models of care and operational structures, processes, and outcomes.
2.5.1.1 Literature search research question
What are the models of community-based palliative care in Australia?
2.5.1.2 Data sources and search strategy
A detailed search strategy was developed by Doreen Nabukalu for three electronic databases including CINAHL (EBSCO), PubMed and SCOPUS. First, a search strategy was developed for PubMed using MeSH headings such as “model of care”, “community-based” OR “home”, “palliative care” and text words comprising key terms and their synonyms. The search in PubMed was limited to articles in Australia to reduce on contextually irrelevant articles. The PubMed search was then translated to CINAHL (EBSCO) using the appropriate subject headings and key terms. With similar key terms, the search was also conducted in Scopus, with title, abstract and key terms searched. No hand searching of articles was undertaken. To avoid loss of relevant articles, there was no limit to any years of publication. The search history is provided in Appendix 3.
2.5.1.3 Article screening and synthesis
Using inclusion and exclusion criteria, abstracts and full text were screened in JBI Sumari™ software tool for systematic reviews. A narrative approach was used to analyse and describe the review findings. Data synthesis of 32 articles identified as relevant to the evaluation was conducted by Dr John Rosenberg.
2.5.2 Organisational documents including grey literature
A desktop documentary review was undertaken to provide broader views of the context within which Little Haven operates. The National Palliative Care Service Directory was used to identify all palliative care services in Australia and organisational documents in the public domain such as strategic plans, annual reports, financial reports and other information published on organisational websites were accessed. Donabedian’s model of evaluation of quality of quality of care focusing upon the structures, processes, and outcomes (Donabedian, 2003) as noted above in Section 2.1.3 was used to map these data. This model has been previously applied in the evaluation of palliative health care systems (Rosenberg, 2007). Again, a narrative approach was used to analyse and describe the review findings. This review was undertaken by Doreen Nabukalu.
2.5.3 Economic data
Given the increasing demand for community-based palliative care services, it is vital to consider the impact of costs for providing end-of-life care in these settings. An economic evaluation of services provided from a health service perspective considers the direct investment made by Queensland Health (QH) and direct outcomes achieved by the service, but also includes the broader impact on the provision of other health services. Data for this analysis were obtained from Little Haven performance measurement data, annual reports and internal records including:
- Deidentified data pertaining to service delivery.
- Economic data relating to service delivery costings including Little Haven funding schedule (such as overall budget, hourly rates for staff, funding for different service components) and deidentified patient health care records (hospitalisations, duration of hospital episode).
- Service delivery, economic and patient health care data obtained from Little Haven performance measurement data, including annual reports and other internal records.
The overview of service costs relating to palliative care provided by Little Haven, including an assessment of economic viability from the provider perspective, and cost evaluation from a health services perspective, is provided in section 4.3 below, and includes an outline of limitations of the economic evaluation, future considerations, and conclusions. The economic analysis was undertaken by co-investigator Dr Katharina Merollini.
2.5.4 Qualitative data sources
This evaluation sought the input of a range of participant groups whose current or past involvement with Little Haven enabled them to provide particular insights through their lived experience. These groups were current patients/carers, bereaved carers, staff, volunteers, and key stakeholders who were invited to participate in the qualitative components of the evaluation research.
2.5.4.1 Recruitment
The qualitative research is reliant on purposive recruitment, introducing potential for selection/self-selection bias. Rather than seeking clinicians’ vetting, an invitation, the Research Participant Information Sheet and Consent Form were distributed via mail by Little Haven’s administrative service to patients, families and carers. Further, invitations to participate were signposted on the Patients’/Families’ Notice Board in the Little Haven offices, with the Research Participant Information Sheet and Consent Form in envelopes below the sign.
Staff and volunteers were similarly recruited via email and signposting. Stakeholders were identified in the desktop review of Little Haven documentation and were approached individually via email and phone by the Chief Investigator.
All participants provided written consent via a signed Consent Form. Response rates were not applicable to this purposive sampling method.
2.5.4.2 Qualitative data collection
Immediately prior to the commencement of each interview or focus group, the research project was overviewed with participants, and informed consent to participate and record the session was verbally confirmed. Participants were notified of the point at which the audio recording of the session commenced.
In-depth interviews: patients, families, carers
Patients, family members and carers who responded to the mailed invitation to participant negotiated a suitable time and place for in-depth interviews to take place. A total of 16 interviews were undertaken in private dwellings by co-investigator Josie Linn, comprised of six patients, three current carers and seven bereaved carers.
The interviews were semi-structured and guided by previously developed Guidance Questions that explored patients’, families’ and carer’s lived experiences of Little Haven, how they came to be involved with the service, the nature of the communication between them, standout qualities and suggestions for future development. Any concerns they have were addressed also. The Guidance Questions are attached in Appendix 4: Guidance questions for participant groups data collection.
Focus groups: staff
A suitable time and place for the conduct of each focus group was collaboratively identified among members of the Little Haven staff team and co-investigator, Dr Trudi Flynn. The initial focus group was conducted onsite at the Little Haven offices in Gympie. Additional focus groups with single attendees were conducted via telephone or Zoom™. A total of 10 staff members participated in the focus group study. The participants were comprised of the CEO, the Clinical Nurse Coordinator, the Senior Social Worker and Lead of the Bereavement Support services, Registered Nurses and clinical nurses.
The focus groups were semi-structured and guided by previously developed Guidance Questions that explored staff perceptions of strengths and benefits of the model, key descriptors of the model from staff perspectives, staff experiences of facilitating the model, experienced challenges, and ideas for further development. Staff perceptions of the relationship between Little Haven and the regional Gympie Community were also explored. The Guidance Questions are also attached in Appendix 4: Guidance questions for participant groups data collection.
Focus group: volunteers
A single focus group of 13 volunteers was held in a meeting area in a local hotel prior to the Little Haven Volunteers’ Christmas party. It was facilitated by Dr John Rosenberg.
The focus groups were semi-structured and guided by previously developed Guidance Questions that explored volunteers’ perspectives strengths and benefits of the model, experienced challenges to volunteering, and ideas for future development. Volunteers’ perceptions of the relationship between Little Haven and the regional Gympie Community were also explored.
In-depth interviews: key stakeholders
The perspectives of key stakeholders were essential to gaining a rounded understanding of Little Haven’s model of care. Eight interviews were conducted by Zoom™ by Dr John Rosenberg, with participants representing the Little Haven Board, and external clinicians including General Practitioners.
The interviews were semi-structured and guided by previously developed Guidance Questions that explored stakeholders’ highly contextualised experience in their associations with Little Haven, strengths and benefits of the model, experienced challenges, and ideas for future development. Their perceptions of the relationship between Little Haven and the regional Gympie Community were particularly explored.
All in-depth interviews and focus groups were recorded and processed by Otter.ai™ transcript generating software. Transcripts were grouped according to participant groups: patients, carers/family members, staff, volunteers, and key stakeholders. Transcripts were checked against recordings and corrected where required; participants were deidentified at this point. These final transcripts formed the data for the qualitative sources of the research.
A thematic analysis approach was utilised to investigate the data (Braun & Clark, 2006; Clarke & Braun, 2017). All of the transcripts were read through initially prior to the commencement of coding. Each transcript was then coded in relation to content. Associated codes were grouped forming the output themes. Given the semi-structured nature of the interview and focus group Guidance Questions, some of the themes were informed by these, whilst other themes emerged and were noted for analysis.
2.5.5 Carer satisfaction survey dataset
Twelve weeks following the death of a patient, the Little Haven administrative team send a Carer Satisfaction Survey via mail to the carer/family member of the individual who has died. Carers are invited to complete and return the survey via an enclosed pre-paid envelope. Returned surveys are anonymous and entered into an Excel spreadsheet by Little Haven administrative staff to create a longitudinal dataset.
This anonymous dataset was included in the evaluation. The survey form is provided in Appendix 5: Carer satisfaction survey. Excel documents containing deidentified survey data were made available to the research team and transferred into SPSS™ for analysis. The data analysis generated descriptive statistics, and narrative analysis of open comments enabled identification of emergent theme. This analysis was undertaken by co-investigator Dr Trudi Flynn.
2.6 Limitations of evaluation design
The evaluation methods, whilst co-designed, may not investigate all aspects of Little Haven’s structures, processes and outcomes.
3. Evaluation Findings
3.1 Review of peer-reviewed literature
This review of the peer-reviewed literature utilised the methods described above in Section 2.5.1 and includes articles addressing models of palliative care provision in Australia, particularly in community-based settings and, to some extent, in regional locations. It is acknowledged that this review is limited to its specific inclusion/exclusion criteria and that other articles may contain valuable information. Nevertheless, this review provides relevant insights into this evaluation project. Key themes have been synthesised from the selected literature and are explored in further detail below.
3.1.1 Rationale for clear models of care
This review identified the historical origins of palliative care services in Australia, noting that their evolution over many decades has led to enormous variations in models of care:
In Australia, palliative care services have emerged largely as a result of funding initiatives since the 1980s with services operating in outpatient, inpatient and community-based settings, with a combination of public and private providers utilising both specialist and generalist models of care (Phillips et al, 2006, p.374).
This has resulted in diverse models which, although they possess common elements (see Figure 2 above), vary widely. In conducting this evaluation, it was important to understand how models of care impact upon the provision of acceptable, feasible and efficient palliative care. To do so has a fundamental purpose for dying people:
Efforts to improve home-based models of care should be viewed as central to enabling the rights of terminally ill people to make choices about how their last days will be spent (Poulos et al, 2018, p.277).
These models must be carefully evaluated for suitability and acceptability to their end-users – patients, families and carers – for whom a pre-ordained or assumed approach to care can render it ineffective in achieving their goals:
The models of care might not translate into granting clients their wishes regarding places of terminal care and death (Aoun et al., 2016 p.17).
A central tenet of palliative care is the placement of the person (ie: the patient/client, and those who care for them) at the centre of care. This was clear in the literature and interrogated further in the evaluation of Little Haven’s model of care.
3.1.2 Person-centred care
There is no question that person-centred care is an indispensable element of palliative care, and one that is particularly demonstrated in community-based settings where individualised care rightly prevails. In practice, this translates into the lens through which interactions between patients and service takes place. The principle of holistic care has its origins in the modern hospice movement and is evident in services where person-centred care addresses not just the clinical requirements of a given patient, but the context within which their illness experience occurs. The provision of person-centred care requires care providers to:
…consider people’s relational, creative, spiritual, cultural and social needs, as well as their physical and psychological needs. Strategies to connect on holistic levels can ensure that clinical care aligns with what is meaningful and important to patients and their families (Stanley & Daddo, 2022, p.10).
Rather than beginning with a set of non-negotiable care practices to be imposed upon a patient – particularly in the home setting – the exploration of context with the patient enables the care to be suitable and acceptable to them:
To ensure the success of the interventions, the nurses need to discuss with the client the nature of the intervention and how it will impact on the client in depth prior to the intervention commencing (Aoun et al., 2016, p.17).
In this study, an intervention promoting a specific person-centred approach to community-based care (“Heidi’s Have a Go” – HHaG) was highly successful:
…the program helped them understand patient priorities (90%) and provided opportunities to build rapport (90%). Most reported that involvement with HHaG helped them understand patient needs (70%) and noticed changes in patients’ emotional wellbeing (70%). Over half of the participants noticed changes to patients’ physical wellbeing (60%) and felt that HHaG provided opportunities to discuss patient values around this poignant stage of their lives (Daddo & Stanley, 2021, pp.534-5).
This responsiveness and flexibility are highly regarded by both patients and healthcare providers (Saurman et al., 2022), enabling ‘a flexible service which allowed carers to maintain “normal” family life activities (Poulos et al, 2018, p.276). This ‘normality’ is a benchmark, perhaps, of person-centred care.
This is a conventional approach for the majority of palliative care patients. What of those for whom engagement with services, or suitability of services, is less clear?
3.1.3 Specific population groups
3.1.3.1 Home alone
Aoun and colleagues have undertaken a number of studies into palliative care patients who live alone. As a population group, they are considerably less likely to manage a preferred home death unless family and social networks are very strong. Nurses have identified specific areas of risk for ‘home alone’ patients, including:
… client falls, ability to manage medications safely, lack of social support, and reluctance to accept assistance to meet activities of daily living such as hygiene needs as their primary areas of concern. (Aoun et al., 2016, p.15).
For Little Haven, those living alone are supported to remain there if it is their preferred place of care; with hospital admissions for end-of-life care of less than five days, and, on occasions, death at home, these outcomes are notable.
It was suggested that a residential hospice was one approach that could provide a home-like environment whilst addressing these challenges to patient safety and care:
… a hospice specifically for clients who are home alone to ‘‘enable the client to experience terminal care in a home environment while also having social, emotional and medical support’’ (RN9) (Aoun et al., 2016, p.16).
This is explored further in the qualitative evaluation sections below.
Nevertheless, approaches to models of care that included Care Workers and duress alarms were seen to contribute positively to successful community-based services providing care to those living and dying alone:
This study has provided a useful insight into the experiences of dying people who are living alone using these models of care. It provided some encouraging evidence that home-based palliative care interventions are useful and supportive to patients living alone. (Aoun et al., 2012, p.604).
3.1.3.2 Indigenous peoples
Culturally appropriate palliative care for Aboriginal and Torres Strait Islander peoples has a chequered history in Australia, and models of care utilised to provide proper support must attain this in their design (Haydon et al., 2021). A significant stumbling point has been the interface between indigenous and Western approaches to therapeutic interventions. In their recent study, Rooney et al., (2022) identified elements of this misalliance, where there are differences in:
… supporting a holistic approach, developing culturally appropriate care, conflict within a Western medical model, regulatory issues, and geographical barriers. …the benefits of including traditional therapies are overall positive, however, there are barriers including conflict with the Western model of medicine and regulation (p.1465).
The utilisation of Aboriginal Health Workers (AHWs) has been identified as a culturally appropriate and effective in palliative care. Their inclusion promotes agency of First Nations people, and improves the acceptability of mainstream care:
The use of AHWs for home visits and support is vital to bridging the cultural divide between mainstream palliative care and Aboriginal culture. In other areas of health care and health promotion AHWs have played an integral role, linking mainstream healthcare services with Aboriginal communities in a culturally sensitive way. Healthcare systems that give the control to the Aboriginal community have also been shown to be very successful in improving access to, and in the context of acceptance of care (O’Brien et al., 2013, p.6).
3.1.3.3 People experiencing homelessness
When many of the models of community-based palliative care are predicated on the presence of a dwelling place, their responsiveness to those experiencing – or at risk of – homelessness can be inadequate. When there is not a central location of care, where cohesive connections with healthcare services and community networks are fractured or absent, many models of palliative care struggle to provide truly person-centred care. In particular, these challenges can be:
… the need for coordination around the complexities of late-stage hospital presentations and multiple admissions, how to ensure the homeless person could access their required medications and keep them safe, how to promote engagement of the homeless person with the health services and dealing with the staff stress arising from working with this group (MacWilliams et al., 2014, p.87).
It has been proposed that a case management approach addresses continuity of care and trust in healthcare workers, leading ultimately to improved palliative care:
… using a case manager to coordinate care, encouraging the provision of appropriate post-hospital discharge accommodation, fostering stronger collaborations between health providers and shelters, and providing training for both health and accommodation staff (MacWilliams et al., 2014, p.87).
3.1.4 Community engagement
Person-centred care in many settings where community-based palliative care is provided can be enhanced through community engagement. This refers not only to those who volunteer specifically with palliative care services, but to the wider community, whose capacity to engage with fellow citizens need not be underestimated:
The responsibility for supporting those experiencing a life limiting illness, the frail, elderly and bereaved can be shared by the community rather than provided predominantly in family and professional silos … If the confidence and capacity of the community were enabled to respond earlier and to less urgent, practical, emotional and spiritual care for those around them, professional care services would have increased capacity to respond to those with more complex care needs (Stanley & Daddo, 2022, p.11).
Models of care that intentionally pursue building this capacity of local communities can be seen to be a key player in, but not controller of, the issues of dying, caregiving and grieving in the communities they serve (Patel & Noonan, 2022). This shared sense of responsibility may be more clearly identifiable in places where there is strong cohesiveness, including regional centres. Carefully harnessing of this capacity is essential to its success:
Given the level of community support that currently exists for the local palliative care service it is important that the proposed model be disseminated to the community and processes put in place to enable resources to be shared throughout the local palliative care system. (Phillips et al., 2006, p.378).
In this way, services not only provide care to those at home, but raise the bar within communities to participate in this activity. In the words of the authors of one Queensland study:
High quality palliative care can be delivered to the community … engaging both the local community and local health authorities (Mitchell & Price, 2001, p.62).
In practical terms, one study described the role of the local palliative care service in raising awareness of Advance Care Planning (ACP) through:
… speaking engagements at public forums such as Rotary, Senior Citizens, and Lions Club to talk about palliative care and more specifically, ACP. They also assumed responsibility to facilitate ACP discussion and complete the appropriate documentation if required when individual people from the community might ‘pop in’ to the service or were referred by local doctors and district nurses for an advance care plan (Blackford & Street, 2012, p.2028).
3.1.5 Partnerships are essential
The imperative to create and maintain partnerships in implementing models of care extends beyond the community to the healthcare sector itself. Care coordination, common documentation for assessment and management, and other elements are essential to models of care that provide comprehensive, managed care in complex settings:
The formalisation of partnerships across the network provides a platform to explore creative alternatives for better continuity and coordination of local palliative delivery, including initiatives such as: co-funding of service delivery; utilising common palliative care clinical indicators and assessment and management tools; standardised data collection, developing a common language; and the use of end-of-life care pathways by generalist health care providers in all care settings. (Phillips et al 2006, p.377).
One of the most utilised approached to partnerships in model of community-based palliative care is the multidisciplinary team.
3.1.5.1 Multidisciplinary teams
Multidisciplinary teams are a key tenet of palliative care practice and are widely implemented in service models of care. Regional settings are especially challenging, however, where healthcare services and sole providers may be scarce or absent altogether:
Community health staff, GPs (General Practitioners), residential aged care providers, private nursing services, acute care providers in both the public and private setting, and specialist medical and nursing staff will need to be actively engaged as partners in the delivery of palliative care in the network. (Phillips et al., 2006, p.377).
This goal, while worthy, can be especially challenging in regional Australian settings where GPs may be under resourced or even unwilling to participate in palliative care multidisciplinary teams. This may be for a range of reasons, some identified by Hatton and colleagues in their trial of a regional palliative care model 20 years ago, when trialling case conferencing for home-dwelling palliative care patients:
It is clear that quality of care and the increase in knowledge and communication are the driving forces for GP attendance at case conferences as opposed to financial reward, given this meeting is unpaid for the local doctors except for some financial redress through the subsequent uptake of [palliative care program] items (Hatton et al., 2003, p.15).
In a more recent study, the General Practice nurses were tasked with promoting and supporting completion of ACPs. Although this places this palliative care intervention at the coalface of primary care, there were some significant barriers to its effectiveness:
Lack of support from GPs and practice managers was the most frequently described barrier. This was described in various ways, including as a culture of resistance to change, lack of interest, difficulty achieving consensus about change sometimes due to a large number of practice staff and a general reluctance of GPs to raise difficult topics, such as dying, with patients. GPs were also described as being more interested in discussing disease- or treatment-related issues rather than ACP or supportive care matters (Nagarajan et al., 2022 pp.153-4).
Nonetheless, other approaches to multidisciplinary teams in palliative care have been attempted, with varying degrees of success.
3.1.5.2 Nurse Practitioners
In Australia, the Nurse Practitioner (NP) is a regulated healthcare professional with advanced clinical skills and limited prescribing rights for diagnostic testing and prescription of medications. In a number of places around Australia, NPs have been utilised to augment the practice of palliative care services, particularly in community-based palliative care. In a trial by Edwards and colleagues, two NPs were employed to enhance care in these numerous ways:
The two NPs provide patient assessments, order diagnostic tests, initiate referrals to relevant healthcare providers, prescribe appropriate medications, and communicate with the patient, their family, and other informal carers. They also work in collaboration with the [name] inpatient services, general practitioners, specialist palliative care physicians, residential aged care facility staff, other multidisciplinary providers, and non-government organisations. These partnerships assist individualised care and education, planning through weekly multidisciplinary care meetings, and preparation for the end-of-life (Edwards et al., 2019, p.251).
Notably, this complex role was built on the practical implementation of partnerships between stakeholders. In another study, the benefits of this role in this setting were clear:
The NP demonstrated how advanced skills can complement the skills of other health professionals in eliciting client and carer wishes and values, and facilitating solutions. Extending scope of practice in home care in particular, is not only essential because of Australian health service limitations, but enabled increased autonomy and flexibility in the NPs’ responses to (often) crisis situations (O’Connor et al., 2016, p.585).
The question of the suitability of the NP role at Little Haven is discussed by staff and General Practitioners and is explored further below.
3.1.5.3 Pharmacists
The home setting in palliative care is one where a significant number of medications can be present and managed by patients themselves or family carers. With the impact of illness or caregiving, the risk for medication error can be high, and the ramifications considerable, leading to distress and even avoidable hospitalisation. In this study:
The inclusion of a pharmacist in a community palliative care team led to an increase in the medication-related knowledge and skills of its members, improved patients’ medication management, and minimised related errors (Hussainy et al., 2011, p.1).
A close working relationship between pharmacies and palliative care providers is necessary for the appropriate and timely supply of medications specific to palliative care in the home setting and is explored further below.
3.1.5.4 Care workers
In some settings, the use of care workers in addition to Registered Nurses has been identified as an effective strategy to enable families to realise end-of-life care in the home, through the provision of practical assistance and emotional support and reassurance (Poulos et al, 2018, p.276). This level of healthcare worker is unregulated in Australia, but receives baseline training through vocational education and, sometimes, palliative care-specific training for work in this sector. In the following study, the ‘care aide’ (that is, the care worker) was observed to be well-received by patients and carers, including those experiencing social isolation, and complementary to the clinical care of Registered Nurses:
The extra care aide support was described positively as providing emotional support, relieving isolation, enabling the client to share their life story, and reducing the anxiety felt by the nurses. Care aide support was described by nurses as a ‘‘great help to those socially isolated clients’’ (RN3) and clients receiving care aide support were described as ‘‘emotionally supported, much happier’’ (RN4) (Aoun et al., 2016, p.15).
3.1.6 Telehealth
There are many challenges in regional areas for the provision of palliative care. In this recent study, these were concisely described and proposed telehealth as one strategy to address them:
People living in rural and remote communities in Australia often experience poor access to palliative especially during after-hours. Poor access to palliative care services especially after-hours can be very distressing for both patients and families especially. This can lead to patients’ symptoms not being managed in a responsive way that meets patients’ and families’ needs. By enabling communities in rural and remote communities in Australia to have access to immediate after-hours palliative care services, telehealth can be useful in servicing these communities and overcoming issues of access and availability (Namasivayam et al., 2022, p.8).
Telehealth is promoted widely as an effective strategy to address the clinical, caregiving and financial challenges of service provision in regional settings (Haydon et al., 2021; Namasivayam et al., 2022; Tieman et al., 2014; Tieman et at, 2016). It is reported to enhance person-centred care, specifically:
Person-centred symptom management – the value of context and clinical judgement: the effects of the telehealth model monitoring tools and their relationship with clinicians’ knowledge of particular patients (Collier et al., 2016, p.411).
However, resistance to introducing telehealth has been observed. In one study, the complexity of this was explored, identifying benefits to both patients/carers and work efficiencies:
Telehealth represents a new form of practice and staff require support in developing skills and changing work practices. Reluctance to change practice to a telehealth option for monitoring of patients may be due, in part, to fear of missing something that would otherwise be picked up from a physical home assessment even though home visits continued to occur during the trial. Clinicians need to see that the change has patient and carer benefits not just system or service benefits (Tieman et al, 2016, p.6).
This was reiterated where it is not possible to see the patient during phone consultation:
… the use of telephone in providing services has its challenges. Being a traditional audio-only communication tool, it prevents nonverbal interaction, can cause communication difficulties, and cannot provide visual feedback (Namasivayam et al., 2022, p.8).
Where this modality was not simply via telephone but videoconferencing, the benefits of being able to see the patient and family were significant:
Clinical benefits of telehealth: the impacts of the telehealth model on clinical care encompassing the following sub-themes: making connections, the visual medium, expressing empathy through ‘seeing’, clinical assessment and the visual, real time clinical data and empowering patients and families (Collier et al., 2016, p.411).
The use of telehealth has also been linked to job satisfaction for clinicians, who cited efficiency, patient-centredness, rapid response, inclusiveness and other benefits:
They discussed the patient-centred nature of the service and expressed satisfaction that they could ‘serve’ more people in need as a result of improved efficiency. They highlighted multiple aspects of the service that were patient-centred including: more patients seen, more responsive (quicker to be seen), patients not needing to travel, inclusion of family/carers, culturally appropriate care for Aboriginal and Torres Strait Islander patients, increased access to multidisciplinary care and more comfortable care in the home (Haydon et al., 2021, p.627).
Financially, Haydon et al., 2021 reported savings in non-labour costs where telehealth was used in a comparison group in a community-based palliative care service in a regional setting; there was no evidence of savings to labour costs.
Of course, telehealth is not without its difficulties, and this study identified a significant range of challenges experienced in a trial of telehealth, with broad impacts:
The troubles with telehealth: the effects on staff when telehealth technologies do not function as planned, along with the effects on relationships when the telehealth model is introduced. This … reveals unanticipated effects of the telehealth model … technological and teething troubles, material and affective disconnections; carer burden; the absence of a ‘disease’ free day; bringing decline into consciousness; and alert overload (Collier et al., 2016 p.411).
Further, its development and implementation can be complex, given that it must strive to achieve ‘…a balance between clinical need, consumer benefit, and technical and financial feasibility (Tieman et al, 2014, p.6) Although concerns have been raised by clinicians about families’ ability to manage telehealth or videoconferencing modalities, this was found not to be the case and, in fact, provided more data to services than would not otherwise be available (Tieman et at, 2016). Critical to the success of this strategy is co-design:
Resources developed in isolation of the intended use and user, and simply released to the market to determine their potential use and value, may have limited value (Tieman et al., 2014, p.2).
It is through consultation with end-users and engagement with staff that telehealth strategies are more likely to produce their benefits, as noted above. It could be assumed that other digital health technologies are also able to address the challenges reported above, however, one study states that, with some notable exceptions, they are not a panacea:
Other than scheduled telehealth, videoconferencing, or after-hours telephone support, little evidence was found for digital health technologies used to deliver virtual models of palliative care (Disalvo et al., 2021, p.1385).
Nevertheless, telehealth has been associated with costs savings and the achievement of good quality care in the community palliative care setting (Haydon et al., 2021). It is discussed further below.
3.1.7 Financial implications of models
Community-based models care bring measurable cost savings to the healthcare system. Spilsbury and Rosenwax (2017) reported ‘…a reduction of inpatient averaged hospital costs of 9% (7%-10%)’ (p.1) through the provision of palliative care at home versus hospital. This cost benefit, however, is not typically passed on to community-based service providers, who continue to be underfunded by government and rely heavily on fundraising. This cost benefit is observed in a range of groups with life-limiting illnesses, including dementia, through the significant reduction of avoidable hospital admissions in the last year of life (Rosenwax et al., 2015). Similarly, early referral of people with dementia to palliative care services is linked to better patient outcomes (Aoun et al., 2016). The financial landscape of Little Haven’s model of community-based palliative care is examined in detail in Section 3.3 below.
3.1.8 Summary of review of peer-reviewed publications
This review is not exhaustive. Many examples of models of care are detected in the healthcare system but not reported in peer-reviewed publications. Some did not meet this review’s inclusion/exclusion criteria. However, it is beneficial to identify the elements of known modules in the context of this evaluation.
This quote identified in this review is included verbatim for its succinct summation of the nature of the models of community-based palliative care:
Researchers continue to explore what constitutes an optimal community service for end-of-life care. Previous literature has highlighted that case management is important, and that comprehensive, direct-contact, team-based care increased the likelihood of dying at home and caregiver satisfaction. The intensity and accessibility of palliative care support is a key factor influencing home death, and lack of 24-hr services to support carers when patient condition deteriorates, or symptoms are unstable can result in unplanned admissions at the end of life. People who have had the chance to discuss their end-of-life preferences with family are more likely to die at home than those who have not (Cross et al., 2020, p.935).
3.2 Review of grey literature including organisational documents
There are 44 identifiable palliative care services in Queensland registered with the National Palliative Care Service Directory. Of these, about 23 provide community-based palliative care, mostly as an addition to other health care services such as hospice or aged care. There are, however, considerable variation in the models of care and services:
- Community palliative care services.
- Specialist palliative care services mainly provided to inpatients and outpatient clinics however there are packages of care in the community for patients and careers. These are multidisciplinary teams providing specialised palliative care support to people with a life-limiting illness and their families. The teams are composed of specialist medical officers, nurses, social workers, occupational therapists, physiotherapists, speech pathologists, music therapists, dieticians, administrative officers, psychologists, and volunteers including pastoral care.
- Palliative care physicians attached to established health service centres (ie: hospitals) provide home visits and oversee the patients’ medical care in their home or review the patient at a local clinic.
- Nurse-led palliative care services:
- o Integrated with aged care: palliative care is provided to aged care residents as they approach end of life.
o Integrated with hospice care: end-of-life care is the primary health care service, however earlier palliative care clients are also catered for.
o Community palliative care service organisations: primarily specialising in providing palliative care within their communities. Staff such as nurses work with the clients and their carers to provide clinical support while remaining in their homes.
o Respite services.
- o Integrated with aged care: palliative care is provided to aged care residents as they approach end of life.
- Telehealth: a team of nursing and allied health professionals offer individualised support and advice to clients dealing with a life-limiting illness through online platforms such as telephone services, emails, SMS, and online chats (eg: PalAssist).
3.2.1 Provision of care services
These services provide an array of individual services which are noted in Table 1 below.
Table 1: Examples of services provided by community-based palliative care
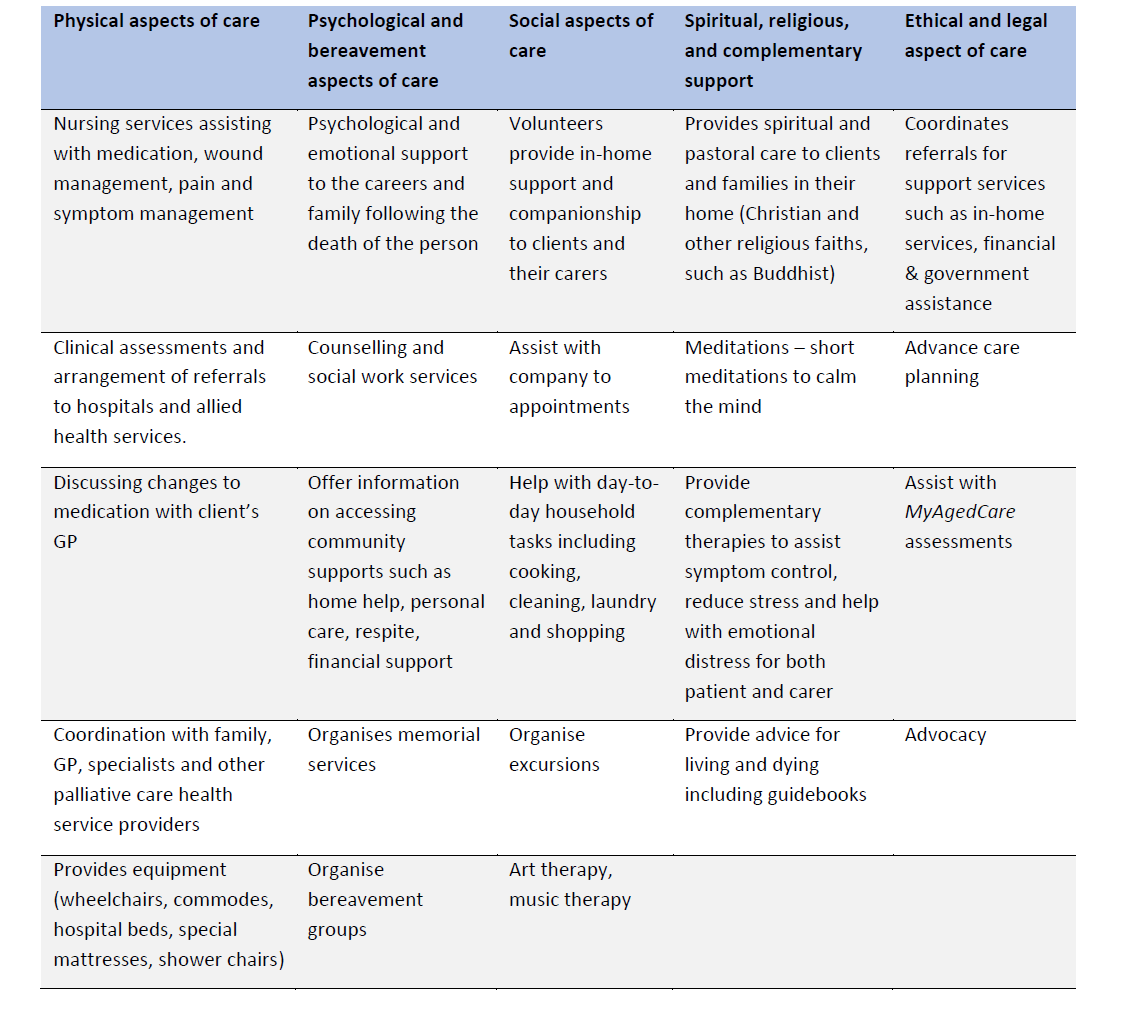

3.2.2 Volunteer services
Volunteering is a central part of community-based palliative care and is found in most models. Little Haven reports a cohort of 146 volunteers in June 2022 and these are denoted in Figure 3 below. Error! Reference source not found.. Notably (although not surprisingly) the vast majority of volunteers are aged 60 and above, including the largest group aged 70-79.
Figure 3: Volunteers by age group, June 2022

Nevertheless, Little Haven report steady recruitment of new volunteers, which is also noted by volunteers during focus group data collection. Indeed, Table 2 below records the annual number of reported volunteer hours which the CEO and Volunteer Coordinator both consider to represent about half of the actual volunteer hours spent in support of Little Haven.
Table 2: Annual volunteering hours
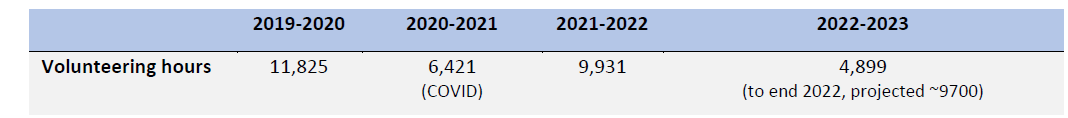

3.3 Economic assessment of service provision and viability
3.3.1 Service provision
As a community-based service which receives government funding in return for a minimum contracted number of occasions of service provided each year, Little Haven also has other sources of income (as listed in the next subsection). The ‘occasions of service’ refer to three broader categories:
- After hours nursing care.
- Allied Health and nursing care.
- Care – bereavement, social and emotional and care conferencing activities.
Little Haven typically delivers most occasions of service for Allied Health and Nursing Care (~60%), followed by Bereavement, Social and Emotional and Care Conferencing Activities (~25%) and After-hours nursing care (~15%). An example of this is provided in Table below for the financial year 2021/22. In an agreement with QH, the hours of occasions of service in these categories are reimbursed by applying a multiplier effect, reflecting the intensity of each service delivered, i.e., ‘after hours nursing care’ is counted with a 1:4 ratio, meaning one actual hour of service delivered is counted as 4 hours of occasions of service. For ‘allied health and nursing care’ a ratio of 1:2 is applied and for ‘care – bereavement, social and emotional and care conferencing activities’ actual hours of service delivered are counted as occasions of service (ratio of 1:1). Notably, the yearly hours of contracted occasions of service by QH were far exceeded by Little Haven by 101% if actual hours delivered are compared, or by 250% if hours of occasions of service including multiplier effect are compared.
A total of 280 individuals received a service provided by Little Haven and nearly half (~47%) also received support from a Hospital and Health Service (HHS) specialist palliative care service. The average length of engagement for each client was 228 days and more than half (57%) of clients died during the financial year 2021/22. Around three quarters of clients (75%) were aged 65 years or older and most clients (80%) established an Advance Care Plan during their engagement with Little Haven.
Table 3: Little Haven Service Provision in financial year (2021/22)
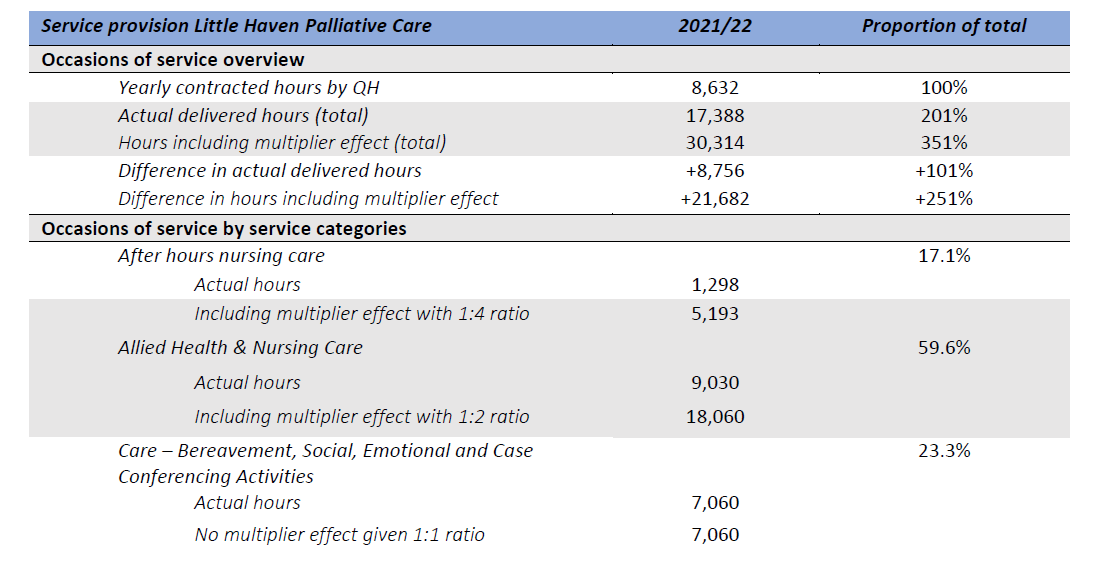

3.3.2 Assessment of economic viability (provider perspective)
An assessment of economic viability of Little Haven was performed based on balance sheets, annual reports and other internal records provided by Little Haven for each financial year, including an appraisal of all financial activity (income, expenses), cash on hand, total assets and liabilities for the last three financial years, from July 2019 – June 2022.
As illustrated in Figure 4: Little Haven income components in financial year 2021/22, Little Haven’s income in the most recent financial year (2021/22) consisted of funding (61%), fundraising (20%), donations (14%) and submissions and grants (5%).
Figure 4: Little Haven income components in financial year 2021/22

These components vary from year to year and Figure 5 gives an overview of income components over the last three financial years, including special government subsidy payments for job seekers and a cash flow boost (available in 2019/20 and 2020/21). It is noticeable that ‘funding’ was the main source of income for Little Haven during this time and overall, slightly decreased (from 68% to 61%), whereas donations and fundraising gradually increased (from 5% to 14% and 13% to 20%, respectively).
Figure 5: Little Haven income overview by financial year (2019-2022)

As shown in Figure 6, Little Haven is largely funded by QH payments (66-87%) and QH patient scripting (4-11%). Funding from the Department of Veteran Affairs and private funding was around 1% during the last three financial years. Whilst the Federal Department of Health contributed 17%-20% previously, this did not continue in 2021/22, as well as COVID-related funding in 2020/21 which was not received in 2021/22.
Figure 6: Little Haven funding overview by financial year (2019-2022)

Little Haven main expense categories are shown in Figure 7 by financial year. The highest contributors to overall costs are related to staff costs, including wages (65-68%), superannuation (6-7%), and employee benefits (5%). Fundraising expenses contribute around 4% per year, followed by IT expenses with about 3% of expenses. A range of other expenses are accountable for up to 2% each, including insurance, motor vehicle expenses, cleaning and depreciation. The ‘other’ column includes a range of minor expenses, for example advertising, bank fees, bereavement support, complementary therapies, education & training, postage, volunteer expenses, repairs and maintenance.
Figure 7: Little Haven expenses overview by financial year (2019-2022)

Given that wages make up a large proportion (nearly 70%) of expenses, these can be further broken down into wage categories for direct medical care, i.e., nurses (~76%), administration (~11%) and allied health (~13%), as shown in Figure 8: Expenses for wages by category for financial year 2021/22. These proportions are typical throughout the last financial years but exact numbers for financial year 2021/22 are shown here as an example.
Figure 8: Expenses for wages by category for financial year 2021/22

Table provides an overview of total income and expenses incurred by Little Haven, as well as total cash on hand, assets and liabilities by financial year. Each year there was a net surplus between total income and expenses with the highest surplus in financial year 2020/21, mostly due to extra COVID-related funding and government subsidies and lower wage-related expenses compared to the last financial year (2021/22).
Table 4: Little Haven financial summary by financial year 2019-2022
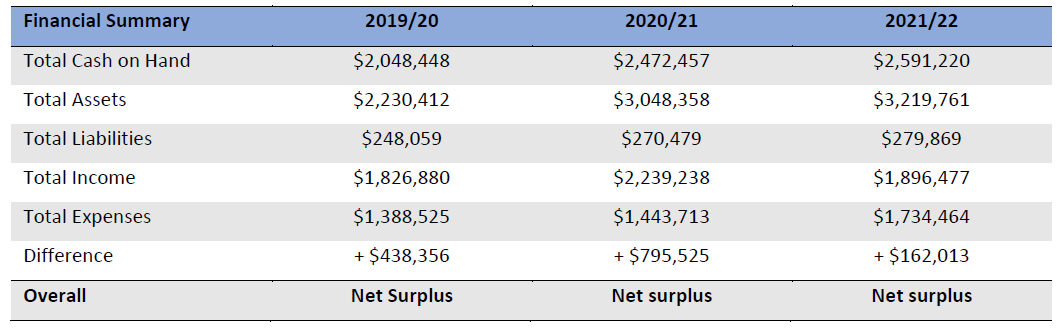
From a business perspective, Little Haven is a viable service which consistently resulted in a higher total income compared to total expenses over the observed period of service. The main driver of income is funding, in particular from QH and the main driver of expenses are staff-related costs which is expected from a service provider.
Little Haven has accrued a substantial amount of cash on hand and total assets with only minor liabilities. Little Haven is a well-run community service and as long as QH or other government funding can be secured in the future, it is in a very strong financial position.
3.3.3 Economic evaluation of service provision (health service perspective)
3.3.3.1 Value for money
As a first step, Little Haven’s direct service provision data was used to assess the value for money given total costs and outcomes. Hereby, costs per hour of occasion of service were calculated as well as average costs per client receiving a service by Little Haven (individuals undergoing palliative care, n=280) and average costs per client receiving care (including family members of individual undergoing palliative care, n=487). An overview of these cost outcomes for the financial year 2021/22 is shown in Table below. Given the contracted 8,632 hours of occasions of service by QH and an investment of $1,001,689 the anticipated cost per hour of occasion of service was $116.
However, Little Haven far exceeded on contracted deliverables and provided over 17,000 hours of service which were counted as over 30,000 occasions of service hours, resulting in a cost of $58/hour of actual hours of service provided ($1,001,689/17,388), or $33/hour of occasion of service (accounting for multiplier effect: $1,001,689/30,314). This represents only 50%-28% of the anticipated cost and is excellent value for money from a QH perspective. However, from a service provider perspective, including all expenses incurred during the financial year, the costs per hour of occasion of service are only half of the anticipated cost with $57/hour. Furthermore, average costs per client receiving palliative care services resulted in $6,194 from a Little Haven perspective and only $3,577 from a QH perspective and the average costs per client receiving care from Little Haven (including family member support) was even lower with $3,562 and $2,057 from Little Haven and QH perspectives, retrospectively.
These estimates also provide excellent value for money compared to average costs for palliative care hospitalisations in Australia of $15,373 per separation (Independent Hospital Pricing Authority, 2021) and average costs of integrated home-based care of on average $8,000 per client in Australia (KPMG, 2020) (see Table ).
Table 5: Cost evaluation of Little Haven service provision in 2021/22 from Little Haven and QH perspectives

Comparison to other palliative care services shows the strong position of Little Haven as a community-based palliative care service compared to palliative care services provided in other settings (see Table 6).
Table 6: Comparison of service utilisation in different palliative care settings
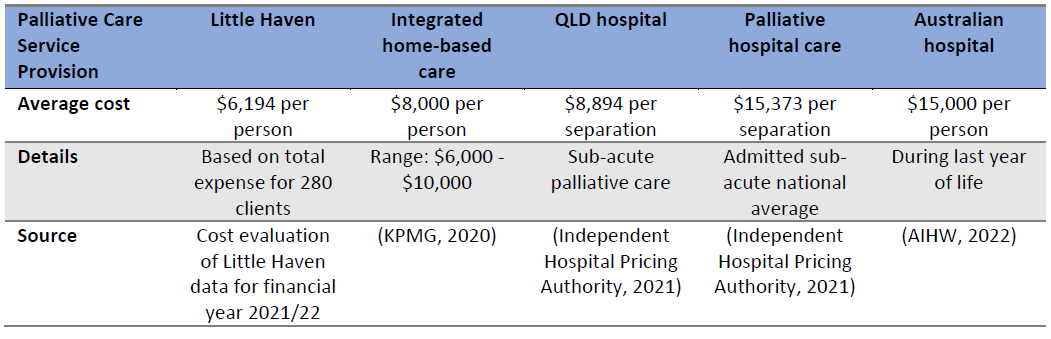
3.3.3.2 Cost savings
As a next step, cost savings due to decreased utilisation of other health care services were considered (see Table ). There is high-quality evidence from the literature that integrated home-based care (IHPC), such as provided by Little Haven, enables individuals to receive care in their preferred location (ie: in most cases their home), whilst reducing time spent in hospital (4.5-7.5days less) and fewer emergency department presentations (2-13% less) in the last year of life (KPMG, 2020). This equates to average health savings of $4,544 (worst case) to $6,109 per person (best case) per year (KPMG, 2020). Based on Little Haven service provision during the last financial year this would apply to 160 individuals who died during the financial year 2021/22 and were hence in the last year of their life, resulting in indirect cost savings to Queensland of $727,040 in a worst (based on 160 individuals with cost savings of $4,544 each) and $977,440 best case scenario (based on 160 individuals with cost savings of $6,109 each). Implementation costs are not considered here as Little Haven is already an established service.
Table 7: Estimated indirect cost savings to QH based on reduced hospitalisations and emergency admissions
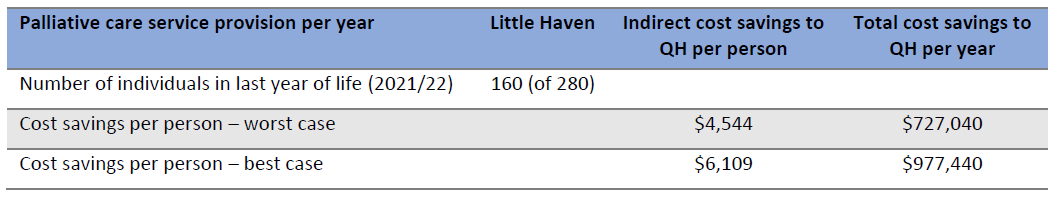

3.3.3.3 Limitations of the economic evaluation
The economic evaluation was limited to a crude cost comparison of direct and indirect costs relating to the services provided by Little Haven and cost savings experienced by QH due to a reduction in hospitalisations and emergency admissions. However, for a full cost-effectiveness evaluation, outcome measures for patients, carer and families would need to be considered alongside costs. ‘Standard’ economic evaluations normally combine quality and length of life into quality-adjusted life years (QALY) as outcome measure (e.g., cost per QALY). The assessment of impact and outcome measures is quite complex and different in the context of palliative care as clients are at the end of life and a positive outcome is a ‘good death’, which is a subjective, unique experience which cannot be evaluated directly or through questionnaires.
Another key consideration for providing community-based palliative care is to allow individuals to stay in their preferred care location for as long as possible, and to die at home if desired. As such, patient satisfaction is an important outcome measure in this setting. Little Haven is a strong advocate of fulfilling clients’ needs and ~90% of their clients died according to their wishes (measured in fulfillment of Advance Care plans) which could not be considered in terms of costs but should be emphasised in the context of value for money.
Also, this evaluation does not take into account the broader societal impact, for example the positive outcomes on family/friends and, as mentioned earlier, a large proportion of services provided by Little Haven consist of emotional support rather than clinical/medical care, such as bereavement, social and emotional and care conferencing activities (~25%). As a result, for example, Little Haven bereavement support may lead to reduced productivity losses by family due to less taken time off work (or other activities) for grieving or reduced use of Medicare-subsidised mental health services. Unfortunately, there is currently no published data describing or quantifying these indirect cost savings and further research in this area is warranted.
3.3.4 Summary
Little Haven is a highly viable community-based service and provides excellent value for money from a health service perspective. Applying a conservative cost estimate based on a reduction of QH health service use (hospitalisations and emergency admissions), cost savings are estimated to range from $730,000 – $980,000 per year for the cohort of Little Haven clients (n=160) in the last year of life alone. Average costs per person per year of providing palliative care services were much lower for Little Haven clients ($6,194) compared to the national average for in-home palliative care services ($8,000) or hospital-based palliative care services ($15,373). Furthermore, contracted deliverables to the state funding body QH in terms of hours of occasions of service provided were exceeded by far (100%-250%) with average cost of only $58 (actual hours) $33/hours of occasion of service (including multiplier effect) instead of an anticipated/funded $166/hour.
For a full economic evaluation outcome measures, such as preferred location of care, preferred location of death and client satisfaction should be taken into consideration. If a broader societal perspective was adopted the impact in terms of increased community well-being and increased productivity (such as due to bereavement support) would even be higher and most likely result in much bigger overall cost-savings but theses indirect cost savings or productivity changes are difficult to measure, and more research is needed in this area to quantify these effects.
State and national funding bodies should strongly consider further investments in community-based palliative care services, such as Little Haven, as this example has shown the excellent return on investment and value for money, in addition to providing high-quality care with outstanding client satisfaction and a person-centred model of care.
3.4 Findings of qualitative evaluation
The participation of various groups in the qualitative evaluation is noted in Table below.
Table 8: Participants in qualitative data collection

(4) One patient who had consented to be interviewed, was unable to participate due to a rapid deterioration in health. The appointment was cancelled by the carer, who had also consented to be interviewed and was unable to proceed in the circumstances.
(5) Current carers of patients appeared more reluctant to participate. The impression given was that ownership over the process was being given to the patient.
3.5 In-depth interviews: patients, families and carer
Analysis of these data identified nine emergent and interrelated themes referring to PEoLC. These are listed in Table below.
Table 9: Emergent themes: patients, families and carers
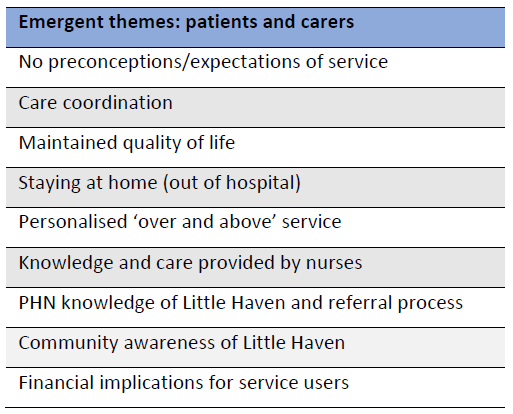
These themes are explored further below, with exemplar quotes from participants.
3.5.1 No preconceptions/expectations of service
One of the clearest emergent themes expressed by all participant groups was that of not having any expectations of the service that would be offered by Little Haven. This was variously described but could be generalised to a cohesive theme that the lack of expectations comes from the fact that end-of-life care is not something that is widely known about until it is needed, therefore, patients and carers alike, begin to learn about the service offered by Little Haven from the time of admission.
Once I worked it out that they weren’t just like [in-home aged care and disability support service] …at first I was thinking they were just like that. But then once I realised what they were like, I didn’t realise how extensive their support is, and how ongoing and how they really do look after you. I know I could go up there tomorrow and sit down and they’d make time to have a chat. I wouldn’t feel at all awkward about doing it. BC2
3.5.2 Care coordination
A particular and unexpected aspect to Little Haven that had a significant impact on the wellbeing of patients and carers, was the extent to which other care services liaised with Little Haven who coordinated care. Within this sample, liaison included but was not limited to other medical services (SCUH palliative care service, GPs, chemotherapy and renal units, hospitals) pharmacies, in-home care and support services external to Little Haven, Centrelink and specialist paediatric support services.
…they were doing a lot of liaising with [paediatric palliative support service] [JL: And for you, it sounds as though that that liaison and that communication with your other supports was quite important?] Yeah…and because Little Haven were also prepared to, either way, they said we can help you if you decide to stay here and not go to [paediatric palliative support service] …so yeah, either way, they were like we can, you can work out end-of-life care plans with us. But because I worked one out with [paediatric palliative support service] and [they] sent it to them. So they were, everyone was on the same page. Everyone was on the same page. BC7
3.5.3 Maintained quality of life
An aspect of the holistic model of care offered by Little Haven that may not be immediately obvious externally but is understood and appreciated by the patients as being a focus of the service aside from the clinical care provided, is the support in maintaining as full a quality of all areas of life as possible.
[JL: what is important to you?] I think at the moment is still keeping a lifestyle. And so like, you’ve been told all these things, you’re not really going to make it, mate. You don’t want to keep that in your mind. So you push that out of your mind and try to keep super positive and keep doing all the things that you want to be doing…and whether that be things at home to finish them off so that [partner] has still got a lovely home and things are still working for her…that’s what is mostly important for me… keep busy… keep the farm going. And I think keeping all those things, that’s what’s kept my head together as well. PT2
Because sometimes my breathing is a bit puffed. Anyway, they told me to get this script from the doctor. And which I have, and I’ve only used it a couple of times. But they equipped me with the stuff, a little syringe because I need to sort of pull it up stoppers everything else, just so that I can have them all ready and then take them to golf, because I play golf …to enable me to still do those things. PT3
3.5.4 Staying at home (out of hospital)
An important aspect of the service offered by Little Haven was the accessibility for patients and carers to seek support and advice at any time. All participant groups indicated that they felt comfortable doing this as they needed. It was noted that the 1800 health number was unable to give advice or information and suggested hospital attendance as a first and only option.
I was surprised at how much availability and how supportive and with phone calls and, you know, the 24-hour service. Like if I do have any questions…I was surprised that there was something out there like that. So instead of having to go through the hospital system to ask all those questions, to have that once you come out of that hospital system and to go into one [organisation] that doesn’t have to follow those protocols…everybody that we spoke to nurse-wise was able to answer the questions, they didn’t have to refer it up. CC1
Oh, I talked to [nurse] at 11.30pm and she was up, she was doing things, it was her shift. She said sensible stuff. I did it. And I went to sleep on that. Whereas, you know, we were hovering…do we have to go to the hospital again? How long can I avoid it? What are we gambling with? …I find that I can talk to someone I know, outside the medical [hospital] system to gauge what’s really worth doing. PT4
Being able to remain within the home to obtain answers to medical concerns was identified as a key aspect in maintaining a more ‘normal life’ for palliative patients and their carers and families. Prompt answers to concerns and being able to then self-administer treatments within the home, allowed patients and carers to continue their routines without the upheaval of extensive and prolonged hospital emergency department visits as a regular occurrence. This support was indicated to promote dignity, autonomy and independence and a sense of control in an otherwise uncontrollable circumstance.
3.5.5 Personalised ‘over and above’ service
Participants described surprise at how readily Little Haven responded to their individual views and needs.
I was surprised that they are so good at what they do, that they just respect those that, you know, they get to know those people…they are not just a set of values they stick to, they step into your values…and they work within those values. BC5
…it was above and beyond, like, wow…in saying that, I don’t feel like it was probably unique. I feel like those, you know, who I had interactions with Little Haven, I feel like they would have done the same thing for anyone they cared for. That’s why I think it’s so amazing. BC7
All participant groups felt that nothing was too much trouble and that at no point had they felt as though they were a burden on the service.
[JL: …anything that surprised you about Little Haven?] How dedicated they are, I’ve found that as individuals there’s just dedication … and [they’re] going to move heaven and earth to make sure I’m okay. PT5
I think they rang me two or three times while I was in there [hospital] just keeping that connection. PT6
Well, the nurses themselves and their attitude towards you that made you feel special. Okay, and they deal with you [partner] as well don’t they? PT1
This personalised service extends to the inclusion of the family and carers.
…they make you feel like one of the family. BC2
And to at least know that when things get pear shaped, they’re kind of there to help the boys [sons] deal with stuff. PT5
3.5.5.1 Allied health and complementary therapies
There were some contrasting opinions offered when asked about the use of allied health services and complementary therapies offered by Little Haven. The patient group showed the most variance in responses, with some making use of many therapies and others sharing they had found a barrier to engaging with these.
And I use their services. So I go there and have massages…and Bowen therapy. I think that helped with my knees, which is more osteo than the other thing. Yeah, so I have been using their services that way. Social worker as well, you know, to talk to her. I was doing some art therapy with my other daughter to try for some conversation type stuff… they’ve been really, really good. PT3
The barriers highlighted focused on accessibility to allied health and complementary therapies either due to location or declining health, meaning that attending Little Haven premises was not possible. There was a question raised as to whether a mobile aspect to these services may be available in the future to increase accessibility.
[JL: Is there anything that could be additionally helpful?] …having a home visit person that could do that, okay, whether it is massage or just physio type thing…I imagine there would probably be budgetary constraints. For example, if I was to try and go and do that there…[requires oxygen] grabbing a tank…and the cords and the chair to get taken somewhere, get treatment for half an hour, 45 minutes, reverse, come home. It’s so cactus…it defeats the purpose of it. PT5
Finally, within this theme, there was a suggestion that in some cases, carers did not access allied health and complementary therapies due to a feeling that they should:
…leave it to people that needed, as good as it was. I thought it was sort of using them…because I didn’t need it. BC2
3.5.5.2 Equipment
Access to equipment was raised within several interviews as being of significant note as a positive of the service offered by Little Haven. In particular, the way this was organised, delivered and then retrieved when no longer required.
[Patient was given days to live] So we were just kind of bracing, it was a big whirlwind. So that, you know, the hospital bed came, all of the moving apparatus and all that sort of stuff came as well from Little Haven, which I don’t who organised any of that. But it all just started to arrive, which was amazing. CC1
3.5.5.3 Respite volunteers
While access to equipment was recognised as a key positive theme through all participant groups, there appeared to be less awareness of respite volunteers. There was a reported misperception that these volunteers provided transport to appointments, addressing an identified gap in support; however, in these circumstances, LH attempts to access funded transport first.
As volunteers and community engagement are considered amongst the key strengths of the Little Haven model, there may be benefit in exploring how the respite volunteer role might be communicated to patients and families in more depth.
3.5.6 Knowledge and care provided by nurses
The specialist knowledge and compassionate care offered by Little Haven nurses was recurrent throughout the interviews. Initially in building relationships with patients and their families.
…at first it was tricky because Mum didn’t want anyone…except for me and [partner] to look after her. And they were really good at just slowly coming in and building up that relationship. BC2
and throughout the palliative journey through to the death of the patient. The quote below describes the experience of one carer at the time of death of the patient.
Anyway, she [nurse] said to me… so how did you guys meet? And so I told her…[description of conversation at patient bedside about patient and partner life experiences – detail removed to protect identity] …and I said oh, his breathing has changed. And she said, yes, that’s because he is taking all these memories with him. And I thought, oh my God, you are cunning! You know, you engage me in all that conversation, not as idle chat but you were relaying it all to [patient] and with that [patient] took six more breaths and didn’t take any more. BC5
3.5.6.1 Excellent information sharing
The style of communication experienced when interacting with Little Haven staff members (nursing, allied support and administration teams) was highlighted as a strength. Honest and open communication of information by nursing staff in particular was able to alleviate fears and uncertainty for both patients and carers around the dying process.
I was going through this stage in the in this disease where I was obsessed with death …and I talked to the nurses at Little Haven and they made me feel so relaxed, it was wonderful. PT1
One resource was cited by several carers as being of utmost assistance in the time provided immediately post death when cognitive function is impaired through initial grief.
…and the other thing that I found 100% helpful was they gave me a pamphlet and it was opened out and in it was everything that you probably need to do after someone’s died. God that was invaluable. BC5
“And that I was most impressed with the information they gave me. They gave me a folder and they gave me the information on who I needed to contact and who did this and who did that. It was marvellous… BC6
3.5.6.2 Primary health knowledge of Little Haven and referral process
The understanding of referring GPs of the service offered by Little Haven showed considerable variation as reported by both patients are carers, with very limited or incorrect knowledge reported in some cases, while being very comprehensive in others. There was a potential geographical link identified within this theme, with GPs within the Gympie area appearing to be more aware of Little Haven, how the organisation works and admission procedures than GPs outside of the Gympie area.
Box 1: Key illustration
And at that point, I went to the doctor and I said, I’ve been waiting for a palliative thing to be offered…and he said, oh sure, what do you want? You could have, do you want to go public? Private? That kind of thing. And I am kind of, I’m happy to go public, thinking that it was, you know, save some money. So public you know, and he said, well, they generally take three days to respond but private, Little Haven, will probably come the next day. And I said, oh, it’s okay, I’ll go public.
And then I sort of put down the phone and thought about it a bit and then I changed my mind and I rang him back and said, no, I’ll go Little Haven and I do remember that part of that decision was having met Sue [at Palliative Networking meetings] and she was so nice, she was so approachable, she was fantastic, you know, I got that impression from the meetings when I was talking to her. And he said Well, you’ll have to get a referral from the public anyway.
Now this really, it is a bit muddled in my memory. And I just thought, you know, what’s the point if I have got to wait anyway, so I rang Little Haven and they really cut to the chase and they said they could…yes they have to get that referral to get the funding that would have gone, anyway, and I said, oh okay, now I understand that but the doctor didn’t seem to understand that or he wasn’t able to explain it… BC4
As evidenced in Box 1, in one case, the referring GP was reported to have given the impression that Little Haven was a private (i.e. paid for) alternative to the SCUH public palliative care service. This highlights a potential development area for comprehensive education for all primary health carers including GPs within the Little Haven catchment area.
A point for further exploration raised through the interviews was the acknowledgement that Little Haven offers a service that can be accessed early in the palliative journey and is not restricted to the end-of-life phase.
…realising that you don’t have to be collapsing on your deathbed to need palliative care. And that’s a big step. PT4
This was observed to be something that does not have a lot of awareness and may link to previous points regarding wider general knowledge about palliative care as well as the potential for development in the dissemination of this information to PHNs and the community in general.
3.5.7 Community Awareness
3.5.7.1 Known for fundraising
A sense of frustration was noted at the levels of fundraising required to fund the service Little Haven provides. There was also an incorrect perception that the service is not government funded (although it is, in part), as it is perceived by the end users to be an essential service, meeting the needs of patients and their families beyond any expectation.
One of the issues is that they have so many volunteers but so much of their energy is taken up fundraising so that they can supply all of this at no charge. It was just amazing you know, all of the visits, and the care, 24-hour care. Well that all costs money, to have nurses on hand all of those things. So, so much of their energy is taken up fundraising where all of that energy should be put towards supporting people and their families. So if they are funded with more and it is a model that works, we know it works, but it needs to be funded so that their energies can be put into looking after the people and their families, not fundraising…everybody knows Little Haven in town… BC2
Despite the service user frustration and confusion regarding the way Little Haven is funded, the perception of the organisation within the community is positive as observed through the dedication of voluntary support.
No matter what, the biggest thing is all the volunteers. They make the place welcoming and they are all helping out. They have a huge support system in town. BC2
Little Haven is trusted. This is in no small part due to how well the CEO is known within the community.
I knew of them, yeah, because I’d been to their fundraisers…and I knew the lady who organised it…Sue…I don’t know her as a friend. But yeah, so I went up to Sue and I said look, Mum’s got cancer, you know, what can I do? And straight away she said…what do you need? BC2
Despite significant community awareness of the organisation, prior to needing the services of Little Haven, there was reported to be no significant general knowledge of the service Little Haven actually offers and where this fits into the wider end-of-life care options.
I did know there were palliative care options…despite, as I said before, being involved with the end-of-life care committee, I actually found there were obvious gaps in my knowledge and understanding of how the process was going to be begun, which isn’t Little Haven’s…I don’t know who to blame. At the time I did feel, why have I not got this understanding and what must it be like for anyone out there who has not even heard of end of life, palliative care?…I thought the GP would kick start the whole thing, so I was waiting for this to come to me… BC4
3.5.8 Financial implications for service users
Linking back to previously discussed themes, in the first instance, addressing potential misconceptions within the primary care services about how and where Little Haven fits into the palliative care and support sector. The potential implications of other sources miscommunicating the financial requirements of accessing the services of Little Haven may cause a barrier to access for some patients.
Secondly, there is a perception amongst Little Haven service users that the service is underfunded by government and that the amount of fundraising required to offer the service free of charge is excessive. However, an alternative view of this, is that fundraising is the reason that Little Haven is so well known and trusted within the Gympie community.
In addition to the links to previously identified themes, an identification that knowledge of accessing MyAgedCare package to assist in funding care offered by Little Haven was something not widely understood or known about by patients or carers. When this was highlighted as an option by Little Haven, it was done in such a way that no obligation was felt in doing this if the funds within the package were needed for assistance in other areas.
And then when Mum got her [MyAgedCare] package…then they said you know, if you can afford to, but you don’t have to do it but you know if you allowed, we could bill you for your visits…so we actually did start paying but only because it was never, no pressure to do it at all. It was just a suggestion… BC2
3.5.9 Subthemes: bereaved carers
During the interviews, bereaved carers either expressed a desire to, or proceeded to tell their full story of caregiving. Also of note, lone bereaved carers expressed a specific desire to be interviewed over the Christmas period. This resulted in three subthemes relating particularly to the bereavement support service provided by Little Haven. They are noted in Table 10 below and explored in further detail.
Table 10: Emergent subthemes: bereaved carers

3.5.9.1 Unexpected service
The follow up service by the allied health team was an unexpected aspect of care and support. The knowledge of this service prior to the death of the patient was variable. There was no specific reason cited for this in the interview data, but this could be due to the focus being on the care of the patient during the palliative journey.
So I think I didn’t realise I don’t think I realised how extensive their support was…like I knew they were there. BC2
3.5.9.2 Continued connection
Continuity of support was identified by the bereaved carer participant group as being useful, in particular by those who had lost their partner and felt a sense of disconnection, now being on their own. Living in more isolated areas ‘out of town’ added to the perceived importance of this follow up service: If I am really upset…I can call and talk to anybody [at Little Haven]. BC3
Even those expressing a reluctance to engage, had still made the effort to attend the bi-monthly social gathering. The attendance and interaction of the allied health support team was noted as being particularly important.
…they do a luncheon…every two months…I’ve been to three of them. And because there was I think about 40 people there. And when you first come to it you don’t know anybody. You’re sitting there all by yourself. The other ladies, a couple of them started talking and then the conversation got onto our partners, personally. But I felt a bit out of it. And I went to the next one… [name] did make an effort to sit [with me]… BC6
The receipt of Christmas and anniversary cards was received well by carers and were an unexpected support in the cases reported …they send me cards all the time… BC3
They even sent me a Christmas card…and as I say, mum passed in February, so that’s a Christmas card 10 months after. So yeah, that’s really nice, so they’re still with me. BC2
In one case, the patient was a child and other support services were involved through the palliative journey and in the follow up support. As the more local service through this particular journey, Little Haven provided a key liaising role for the family in being able to have their very specific end of life experience.
3.5.9.3 Allied health and complementary therapies
Knowledge of these services was seen to be variable, information received post death is a lot to take in and it may be that within all of the other information being given at this time, these get missed. Similarly to the reported experience of carers accessing complementary therapies while Little Haven was caring for their family member, a reluctance to utilise services was highlighted in the post death access of these.
…so every service that I’m using, I’m using up their resources. This was the other thing…so there’s my thing…about not deserving to be…the recipient of some free end-of-life services, palliative care services, okay I’m not really qualified to be the recipient of some art therapy for nothing. It’s obviously costing somebody… BC4
3.5.10 Summary
Patients, families and carers supported by Little Haven express high praise for the service. For some, it was unknown to them, until they came into their care, when they expressed surprise at what was offered through Little Haven’s model of care.
This group of participants were struck by the coordination of their care by Little Haven, between multiple healthcare providers, including their GP, the Gympie Hospital, SCUH and others. Although there were many aspects of healthcare to navigate, this pivotal role played by Little Haven was seen to be key to them staying out of hospital wherever possible. Descriptions of Little Haven going “above and beyond” reflect the surprise already noted. Visits to patients in hospital, the 24-hour phone contact and home care were deeply appreciated.
The clinicians of Little Haven were admired for their knowledge, skill and sensitivity in providing palliative care and bereavement support to patients, current carers and family members, and bereaved carers. Ongoing support gave participants a sense of continuing care.
Some participants expressed their frustration at the funding arrangements for Little Haven. Whilst there was acknowledgement of the government funding provided, it was the source of concern that so much of Little Haven’s efforts went towards fundraising to fill the gap.
3.6 Focus groups: staff
There’s a story…you know. Phyllis Little started Little Haven from a need in the community. And her group of women were committed to making it work. And now, here we are 40 years later, with an incredible service. It’s a connection to story. It’s a connection to something real, that ignited this service. SF3
The Little Haven clinical team are the interface through which patients and carers experience the therapeutic aspects of the Little Haven model of care. A series of three focus groups were undertaken with clinical team members, with a view to learning more about staff perspectives and experiencing as key facilitators of the model.
Exploration of the focus group transcripts identified eight emergent themes pertinent to the research objectives. These themes are noted in Table .
Table 11: Emergent themes: staff
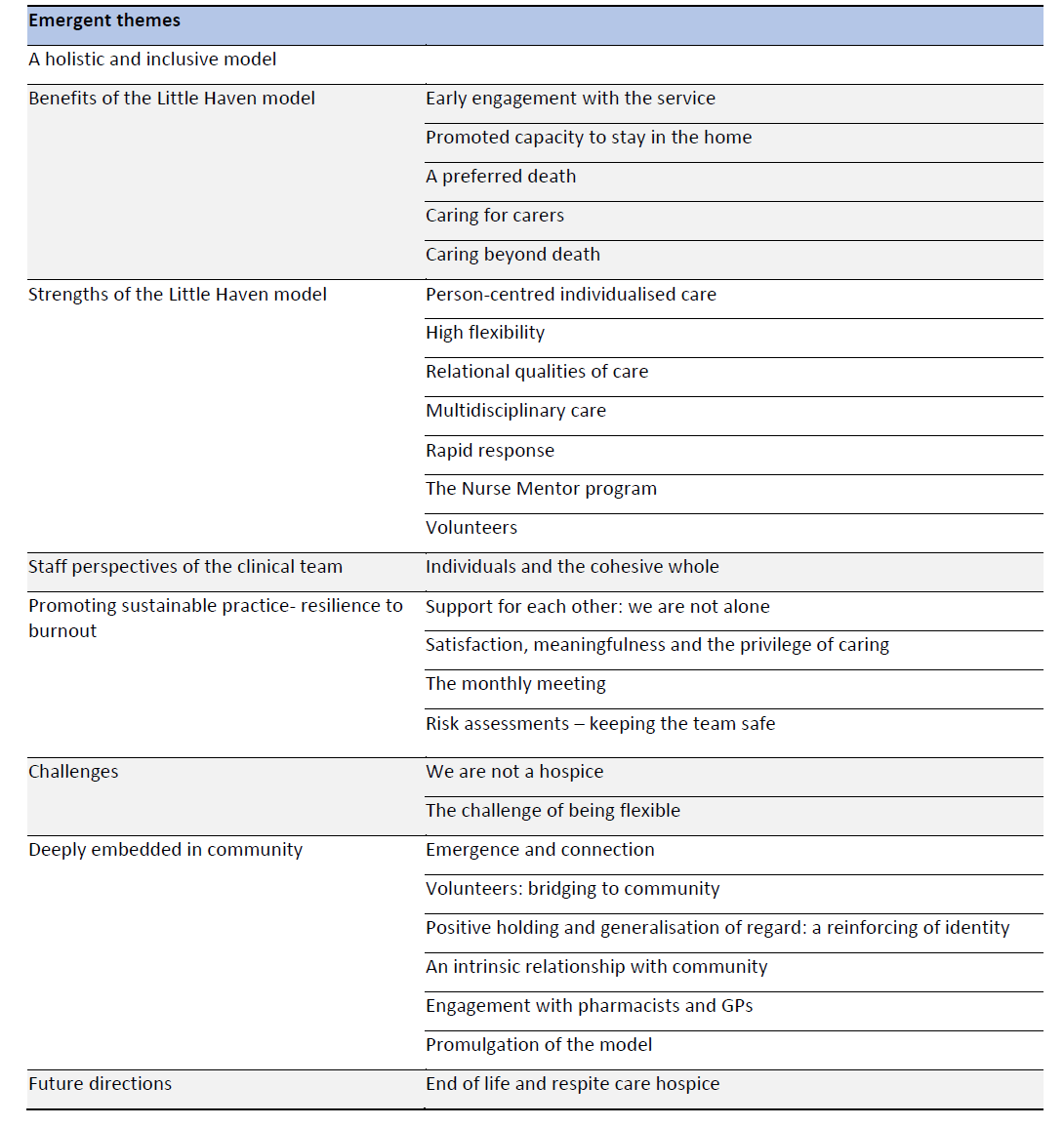
3.6.1 A holistic and inclusive model
At the opening of each focus group, participants were invited to describe in key terms, their understanding of the Little Haven model of care. There was consensus around the term ‘holistic’, and the concept of familial/carer inclusivity, as key descriptors:
It is a holistic approach to terminal diagnosis that comes to a family. It is not necessarily about patients. In the essence of it, it’s about the people that support somebody with that prognosis …so I think that is where we really shine. We make it quite clear in admission that we’re here for all of you. SF10
All-encompassing holistic model that encompasses the client, the family during the palliative diagnosis, journey and then the bereavement afterwards. SF11
The Little Haven model as facilitated by the clinical team, appears to expand well beyond the singular focus of patient care, to include care of carers. Similarly, the offered care itself is multidisciplinary for both patients and carers, incorporating on-call medical/clinical care, equipment loan, health management, social work care, counselling, complementary therapies including art therapy, Bowen Therapy, Reiki, social and support groups, and health administration support.
You know, like they love it when we do the admission and we’ve got a therapist here, we’ve got this, we’ve got that, we’ve got the equipment. You can see their shoulders just relax and they say we were wondering how we need to get a wheelchair but we haven’t gotten money’…we say whatever you need, it will come in a timely manner. SF10
When they first realise the extent of our resources, and the extent of our availability they are so grateful…they’re quite stable and then something will happen and they will give it a try, and you’ll get a phone call at 11 one night….’is there any chance a nurse will pop out?’ ….and out you go. At 11 o’clock or midnight and they go ‘oh my God its true’…and then they never call again, because they are confident and they know that you are there, and that builds the confidence. SF10
Little Haven can commence at any time post diagnosis, and continues beyond the death of the patient, with a longitudinal program of bereavement support offered to carers.
There’s no limitation on proximity to death. We never would ask, you don’t ask particularly I think. SF1
The Clinical Team members further highlighted the inclusive and non-discriminatory nature of the Little Haven model.
I would describe Little Haven Palliative care as holistic, and a very social-based nursing model of care. That it is early entry, that it’s zero discrimination. It doesn’t matter if people live alone or have carers, it doesn’t matter where people live, as long as it’s in a geographical zone, it doesn’t matter if it’s a shanty, to a mansion. And everybody’s treated exactly the same. And that because we don’t have any means testing for that. Our services are free to every single person, there’s no limitations to who we can care for. And everybody gets the same care and access to care. SF3
I observed that there’s patients that we see that are quite tricky, that they have difficult circumstances at home, they’ve got difficult family members they’ve got to deal with. And they are people that actually other services would not go here. Saying No, we wouldn’t take on that person. But I’ve never known Little Haven to turn anyone away, and you know, we have had some really very interesting characters to look after. SF5
3.6.2 Benefits of the Model
The Little Haven clinical team identified a range of benefits associated with the implemented model of care, including the opportunity for early engagement with Little Haven, enhanced possibilities to remain and die in the home, the extension of care to family and carer(s), and the supportive holding of family members and carers across the death of the patient, and for some time after.
3.6.2.1 Early engagement with the service
According to the team, most palliative care services require patients to be within three to six months of likely death at the time of becoming involved with the service. Notably, the Little Haven model accepts patients into the service at any time post-diagnosis, with a range of attributable benefits.
Meeting early means that you can build that rapport…you get to know them, and they trust you. And you’re able to go through the whole trajectory with them, which is really special. SF6
One of the top three fears most people in the world have is fear of dying. It’s the unknown. And I think that earlier entry gives us time to actually help people process that existential angst and all of the questions and all of the fears. You can’t do that overnight. Yeah, you can do that stuff in a few weeks. It takes time for them to accept, to process, and all of those things because it’s so tiring… People say, I’m not scared of dying. I’m not scared of what happens after I die. I’m scared of what’s going to happen between now and then. Because they don’t know. So it’s just being able to talk through and demystify it. Normalise this process, remind them that we’re human beings the same as any other animal, and our systems work very similarly. And just talking them through those things. SF3
A naturally arising next question at this point was ‘What happens when people arrive late into palliative care services?’ The team responded:
I think they still develop [rapport] very quickly. Yeah. And I’m sure whether it’s … any of the other services, I think the fact that you’re with people, it’s such an intimate time in their life, you do develop quick rapport. But I think that the experience for the patient is better if they had a longer time to develop that. There is plenty of research, supporting that early access to palliative care improves quality of life and quantity of life. That’s one of the selling points. We’re going to manage your symptoms, you’re going to have a better quality of life. SF1
I think having cared for both [scenarios] in bereavement, because we’ve had patients, you know, 24 hours, literally, that we have gotten home that have died because that’s what they’ve wanted to do. It’s often the conversations that weren’t had, because no one was willing to face or talk about the fact that a person’s dying, and they didn’t have all these lovely early conversations with our nurses that actually demystify that process and encourage them to talk about those things. I think that’s a big difference for people who have that shorter interaction. In bereavement support, I’m probably doing more talk about all of the conversations [that carers] wish they had had…. I often have to deconstruct more of that as part of their bereavement support. They haven’t had that same level of guidance and through that process, so I think that’s a really significant difference in our service. SF2
Early engagement with the service can also produce a scenario in which there are at any one time a number of patients with quite stable health involved with the service. The variation in immediacy of need can be supportive of the model’s orientation towards flexible person-centred care, as the patient group may not all be experiencing high needs at the same time, creating a moveable availability of time to flex across appointments:
We take patients from the minute they ask for us. Nobody is turned away. Generally a palliative diagnosis is 90 days, the three months thing, and a lot of people don’t recognise palliative care as being as extensive as we do. Our run sheets do actually have stable people on them, and we are doing a lot of holistic caring, really preparing these people spiritually and emotionally. So with these people peppering our seats and populating our patient lists, it does make for a more flexible patient list, because not everyone on the list is vitally scripted for a visit today. SF10.
3.6.2.2 Promoted capacity to stay in the home
Many individuals who receive a palliative diagnosis express a preference to remain in the home for as long as possible (Nysaeter et al., 2022). Clinical team members reflected on conversations with patients and carers, that appeared to indicate that the Little Haven supported patients and carers in this preference:
I’ve had so many comments, especially in the last six months. If it wasn’t for your girls, helping with hygiene or helping this, we wouldn’t be able to stay at home. And that is coming back, more often than not that people are able to stay at home because of our service. And that’s honestly the truth. SF6
A combination of factors within the Little Haven model may potentially contribute to this outcome. Primarily, the availability of clinical and registered nurses visiting the home ensures that health is monitored appropriately, with timely address of any chronic or arising health needs:
So many people talk about how that’s what got them through. They knew if something happened at two o’clock they could call. SF2
The Little Haven clinical team can also provide interim care for patients who are discharged [from hospital/ health service] and who are experiencing a gap between discharge and the activation of other services, or are returned home without supportive services in the home:
You know, it just fills this enormous gap. As we see, when people are discharged, and they don’t have the proper services in place, right. And I do believe that we’re having filled that gap beautifully. And they feel so well supported, and they are able to stay at home with loved ones. Yeah. And I think that’s just such a really special. SF6
Once other services are activated, Little Haven nurses can provide context specific training of other agency providers who come into the home, supporting an improved specificity of care on the part of the providers, and an improved experience of care on the part of patients and family members:
…even upskilling their workers because, it’s that thing sometimes of hygiene assistance or something like that, where they’ll want the Little Haven nurses because they know how to handle someone who might be fragile, whereas they’re just getting a carer that maybe hasn’t had that experience. So sometimes our nurses can pair with them to actually teach them, how to better give appropriate care for someone who’s going into the palliative stage where it really matters how they are handled. SF1
Requests from Service Provider organisations for support from Little Haven nurses provides an opportunity to advocate for a preferred model of care:
…it’s good that organisations come to us and say, could you just talk our workers through what you’d expect of their care in the home, and we’re able to say we would like some consistency with the carer in going into the home, we want, don’t want a different person going in every day. I think that helps upskilling them as an organisation. SF1
Current approaches from organisations asking Little Haven to guide care in the home where multiple service agencies are present, potentially suggest sector readiness for a coordinating role that can work to maximise outcomes for patients in these contexts.
Little Haven nurses and social workers are also active in supporting patients and carers with the at times highly complex applications for supportive financial and service packages such as the Aged Care package. With these in place, patients and carers are able to access a range of ancillary services that also promote their capacity to be cared for at home for longer, up to and through death.
3.6.2.3 A preferred death
Implementation of the Little Haven model is strongly person-centred, with advocacy for patient choice. The team is equipped to support a patient through death at home and is also readily available to support transition of the patient to an end-of-life hospice or a hospital, pending their preference or plan. This capacity to support the preferences of the patient is greatly appreciated by carers.
From a grief perspective, the amount of carers or family that say one of the things that comforts them, especially at raw grief, is knowing that they fulfilled their loved ones wish to die at home. Yeah. So that’s actually like a huge comfort to them. And they always say, couldn’t have done it without, pretty much 99.9% of homes will say, we couldn’t have done this without you. SF3
I think it’s lovely too that they can have a choice of where they want to be. Yeah. I mean, it’s home based, and if they have the goal is to end their life, with their family at home, then that’s what we do. Yeah. Sometimes it might be as long as possible, is what we can do. SF5.
…and that seems to be very different to a lot of organisations we deal with. You ring them up and before you can start talking it’s like, oh, we don’t do this. We don’t do that. So we try always I think and the girls are brilliant at it, well what can we do to help? We might not be the main provider for them, but at least we can triage their concerns and get them on the right track. I think that’s probably the difference. SF1
3.6.2.4 Caring for carers
As indicated within the opening of this report, the Little Haven model of care encompasses the patient, carer and other family members. During home visits, or visits to the Little Haven site, the clinical team will observe and evaluate both patient and carer, determining and responding to identified need. This emphasis, and associated action may represent a point of difference between Little Haven and other palliative services.
Also, it’s not just the care for [the patient]. We also care for the carer. Yes. And in sometimes, you know, we might not need to visit the patient because they’re lovely and stable. But the carer has got so much going on. Nope, I go. ‘Okay, so we’ll see you at one o’clock, then?’ Because you need us. SF6
…and that might become a two hour visit because the carer needed support. But when you looked at it the patient was quite stable. SF2
The range of complementary health and allied health services offered by Little Haven are also available to patients and carers, and carers are encouraged to visit the Little Haven site, both with their family member and on their own. The Little Haven management team are also currently exploring a service package of providing a carer into the home to support Little Haven patients and their carers. This is expanded on in a little more detail within the ‘Future Directions’ subsection of the report.
3.6.2.5 Caring Beyond Death
Within the scope of the Little Haven model of care, support is available and ongoing to carers beyond the death of the patient, through the Bereavement Support program. This is a structured initiative within the Little Haven Palliative Care model, that is offered at to each family. From the Little Haven Bereavement Support lead:
The day following the death of a patient, a member of the clinical nursing team will visit the family to provide bereavement support. There is also a pack that is sent out in the mail that has a little booklet that just talks about grief. It lets them know that a social worker will be in contact in the next two weeks, and that there are some complimentary [sic] therapies available to them as well as part of the bereavement support program. Within the two weeks, one of our social workers will reach out over the phone. They will talk to the person and assess where they are at, and what might be of assistance for them in terms of bereavement support….The model tries to address that everybody grieves differently, everyone’s circumstances are different. Not everyone necessarily needs six face to face session. But, you know, just trying to identify with that person collaboratively about what is going to be useful at this time.
So for some people that might be they’re gonna come in straightaway and have a face-to-face counselling session. Others it might be they might come in and have a massage. And for others it might be ‘Can you call me in a month? Yeah, sure, that’s fine… So we keep on reaching out over a period of time to people to see if they want to engage because grief changes over time. And people’s need changes over time…There is no timeline to that there’s no end date set on that. It’s just as long as the person needs that support, until we both agreed to close essentially. SF2
Little Haven also sends out anniversary cards, and Christmas cards – with some tips for how to get through the first Christmas. There is also a yearly Memorial Service, for all those who have died in the previous year.
Feedback from carers in relation to the Bereavement Support provided by Little Haven is consistently highly positive, as can be seen within the Carer Evaluation Survey outcomes, included within this suite of reports. A clinical team member adds:
I think in particular, it’s not pathologizing, your grief, that, you know, it’s a bereavement support model. So it actually acknowledges that when you have somebody die, particularly if you’ve been a carer for that person, or they’re a very significant person in your life, that it is a significant challenge and struggle, and that you might need, you know, just a little bit of support to get you through that without necessarily needing to diagnose in any way… It’s that continuity of care. SF2
3.6.3 Strengths of the Model
Focus group participants identified and described these perceived strengths within the Little Haven model of care:
- Person-centred individualised care.
- High flexibility in relation to delivery of services.
- Relational qualities of Little Haven care.
- Multidisciplinary care.
- Rapid response.
- The Nurse Mentor Program.
- The vital inclusion of volunteers within the Model.
3.6.3.1 Person-centred individualised care
‘What do I need to know about you to give you the best care possible?
At the centre of the Little Haven model, sits the understanding that death, dying and bereavement, are experienced differently by each person. There was a voiced position within the groups that care models will ideally offer structure, alongside a capacity to tailor services to meet the specific need of a presenting individual.
In reflecting on the Little Haven model of palliative care, SF3 offered:
It’s truly client centred care … it’s what each client needs. We might have a bit of a framework for our care, but we also tailor it to each client and each family based on their needs, which I think is really important. The focus is always the client’s needs. So, if they need care, and they need help, and they need support, we focus on that.
Further, patients’ and carers’ needs continue to shape the service offerings of Little Haven, as staff attend and formulate responses that can take the form of a walking morning, group lunch, an in-house service, or therapeutic group, moving and fluxing as needs shift over time:
Little Haven’s model is responsive to people’s needs and that will mean that it will continue to grow and change. I have considered starting a 6-week therapeutic group as I have identified some people who might be interested in doing that. It is something we could explore doing. We have held many education sessions in response to identified need. Another example is our social gathering, it grew out of talking to people and identifying a need. Our art therapy group works beautifully and again responded to what people wanted. It’s an open group that people can come and go to. I would hope that Little Haven will continue on and continue to grow and change. SF2
3.6.3.2 High flexibility
The capacity of the Little Haven model to allow for a flexibility of approach with patients and families was identified as a hallmark feature of this model. Staff identified the profound value of being able to move and flow in their work according to the presenting needs of the patient and carer, rather than adhering to a projected rigid schedule.
So I’ve worked for other community nursing organisations, and they’re very strict with like, how long we get with each person, whereas I love the Little Haven model, which is you’d have a visit. And if that visits 15-20 minutes, or if that visits, two hours, it’s whatever that family needed that day at that time. And, and I love the flexibility of that and not feeling the pressure of when they got an hour here, I gotta go. If they need that time, they get that time. SF3
We don’t have strict guidelines on timeframes for [Bereavement support], and that we’re allowed to give the care that’s needed, rather than the care that we’ve prescribed, or prescribed by others. But we are actually responding to what the individual needs. SF2
With the whole of the clinical team working flexibly from this principle, it was of interest to inquire how such flexibility could be managed at the organisational level.
Everyone at Little Haven wants this, and Sue as the manager, facilitates this. From the Board of Directors down, this approach is encouraged. That’s what we are. That’s what we do. SF11
Even though [the nurses] have that flexibility, it still seems to work. You would think that it would be a scheduling nightmare, but it’s generally it isn’t. we like to think it’s divine providence, I think, if you do good work well, then it falls into place. SF1
You just have to hand it over. Chuck it up for whatever God it is that you favour and just simply believe in divine providence, you just have to believe it. So for instance, you’ll come to work and there will be a clinical board for that day is really big. You have one patient at Rainbow Beach, three at Cooloola Cove and one at Tin Can Bay. And there’s all that driving to do. I can’t do that. It’s ridiculous. So I’ve got two choices. I instantly become harried and rational always says, you know, this isn’t fair that’s just too much work. That’s just ridiculous. I’ll never get through this list. Take a breath. You start making calls. Oh, I’m down at SCUH, having a molar out, so I tick that off. Next, yeah, we’re definitely down for a visit but we won’t have long I’ve got people coming. So I say okay I will pop in for 20 minutes, a short visit. And it just works [out]. We all agree. SF10
In practical terms, staff indicate that a range of factors may contribute to the capacity to remain flexibly scheduled. As noted previously, onboarding patients earlier in their palliative journey means that there can be a number of quite well or stable patients, at the same time as there are some patients experiencing high need. At other times it just requires a bit of shuffling.
We work really well as a well-oiled machine, I think. Okay. And I think we all feel comfortable reaching out to each other if you do need support. SF3
3.6.3.3 Relational qualities of care
There is recognition among the team that the nature of their work calls for deep relational engagement with patients and their families. Comfort too, with this aspect of their work.
I think a key word is relationships. Yeah, building that relationship from the first moment. And then whether we’re in there for five years or five days, it’s almost like the same level of connection and relationship forms with those families. And, you know, years later, and it’s still that, you know, feel like you’re still talking about families, because they allowed you into such a vulnerable space and time in their life, which, for me, is a huge privilege. SF3
I think when you talk about words that describe Little Haven well, compassionate care has to come at it, and I’ll steal [colleague’s] words here…that Little Haven being a model for humanity. And I think compassionate care is what we’re talking about there. And that’s the thing that we hold for each other. It’s also the thing that we hold for our community and our community feeds it back to us. SF2
3.6.3.4 Multidisciplinary care
Some of the participants spoke particularly to the value of being able to draw from a multidisciplinary team in the provision of care for patients and families.
We have a lot of social work, because we work so closely together, like our social work department is not somewhere else….We used to spend a lot of time doing things like advanced care directives, my aged care applications and the follow up phone calls to Social Security, introducing patients and carers to JPs. It was not a nursing role, but we did it, and then, our social workers came along and took on these roles, and we could then see even more patients on the road…We go to the social workers with our own concerns as well, which can help us stay afloat when things get particularly challenging. SF10.
The significance of having complementary therapies available as part of the model was identified, with the work of the art therapist with patients, carers, bereaved family members and the children within these families highlight. The work of the massage and Reiki therapist were also acknowledged.
The third arm of what we offer is the complementary therapies. Yes. The art therapist is quite remarkable what they drew out when working with patients’ and carers’ children. SF10
3.6.3.5 Rapid response
Little Haven has made a conscious decision to be as responsive to patient or referrer inquiry as possible.
I think that our responsiveness comes from that community connection. We feel a responsibility to our community, because we’re part of the community …when I work for Little Haven, I think ‘what does the community expect of us?’ and they don’t expect us to put someone off. If somebody reaches out to us and wants our support, then we give our support. SF2
3.6.3.6 The Nurse Mentor Program
Each new nurse who joins the Little Haven clinical team will spend the first month of their service shadowing, and being mentored by, one of the more senior clinical nursing staff. This lengthy mentoring provides opportunities for the new nurse to observe and onboard the implementation of the Little Haven model of palliative care, and to form relationships with other members of staff ahead of commencement of their applied role. Several team members spoke of the mentor program.
I think the mentoring programme is such an important part of our model… For at least a month, [the new staff] are supervised and go out on the road with all of the nurses. So they get to see all the different approaches, because everybody brings something different to the care. It’s vitally important that any member representing Little Haven has the model of care down pat. SF1
So I’ve worked at places where you might get a day [shadowing], and then you’ve got a patient load. So being with the nurses per month? Wow, I could not believe it. I just thought this is gonna have to end in a few days. Yeah, just that whole month. Just was amazing. SF6
3.6.3.7 Volunteers
Little Haven clinical team members describe volunteers as vital and integral to the successful implementation of the Little Haven model. Volunteers can be involved in a range of support roles within the Little Haven site, within the community in activities related to the promotion of, or fundraising for, Little Haven, and within the homes of patients, providing respite for carers. Many of those who become involved with Little Haven have been recipients or close relatives of recipients of Little Haven support.
Volunteering is such a big part of our community about model as well because you know, a lot of services are moved away from volunteering, because it’s difficult then managing volunteers is difficult, but what they bring to us is so important. One is a social support system for some of our bereaved who, come back into the into the model as volunteers. They have their own social support. Yeah, and it all keeps us true to our mission. When not, you know, we remember that we are paid and that’s a privileged position within the organisation. But those people [the volunteers] are still doing things to prop our service up bringing their hands to work. I think volunteers get a lot out of what at what they do to I believe they’ve got their own social network development. It is so important to engage [with the volunteers]. We would never afford to do what we do without them. SF1
3.6.4 Staff perspectives on the clinical team
Great warmth and affection enter the voices of the participants as they begin to describe the characteristics of the Little Haven team. This is clearly a group of women who greatly enjoy each other, and the work that they do together. What emerges in this discussion is the dual sense of the team working together as a cohesive whole, while also sustaining identity as individuals within the whole. The ability also to see the value in both states:
We are like one big super nurse… None of us feels like an isolated individual within a team. We are a team. And we are all individuals. We are part of something bigger than ourselves. SF11
What we love about our team is that we’re all very different. Yeah, and have all very different personalities and hobbies and interests and walks of life. And sometimes it’s just the right nurse at the right time. And it could be that that family needed [name] to go after, you know, six weeks of visits, because it was [name] particular, you know, that, that that family needed to open up and have that conversation. And we trust that, like, we call it, you know, the Little Haven magic. And it’s just saying just the right person at the right time for that family. SF3
I find in bereavement support that everyone has their favourite Little Haven nurse, they’re not meant to have a favourite. But what I love is the answer diversifies greatly. It’s all amongst the team, because it’s just that, and I think that’s part of our strength. Yes. And they do have that connection with that person. And they arrived at the right time. And they were all able to hold that conversation beautifully. SF2
3.6.5 Promoting sustainable practice: resilience to burnout
It was observed by a participant during the focus groups that the Little Haven clinical team were not burning out, in contrast with the participants’ experiences in other palliative settings. This presented as significant and prompted consideration of discussed factors within the Little Haven model that may promote sustainable practice and promote resilience to burnout in this intensive workplace.
Field nurses burnout in palliative care. Yes. Somewhere between five and seven years or something. Between five and seven years. For that long, yes. It’s too much. Yes. Now here, I am at nine years. [Colleague name] is nine years. Wow, [Colleague name] is 16 years. [Colleague name] is retired. She would still be there otherwise. She was 70. Yeah, we don’t burn out? SF10
3.6.5.1 Support from each other: we are not alone
As noted above, the clinical team clearly identify themselves as both collective and individual. One participant related this to the palliative care model that the team are a part of:
Not being alone is a part of our model of care. So in the same way that it’s one of the, like, spinal parts of our structures that our clients and families never feel alone in their job. I don’t think as a nurse that I feel alone in the work that I’m doing. But I can always call and even if it’s, if even if I know that a staff member is not working, that I’m really kind of stuck with something or needing to talk, I know, I can call [colleagues], and just go, Can I just talk to you about this? So I feel like what we provide for our clients and families, we also provide for each other. SF3
I think the fact that we have such a supportive environment… I think if accumulated grief is not acknowledged, and if what people do isn’t appreciated, then the burnout rate could be quite high. One of the lovely things about Little Haven is you have the ability to debrief and talk, you can call anyone at any time and they’ll all just, you know, sit up in bed and have a chat to you if that’s what you need to do. SF11
This sense of connection, and congruence with the model of care was also stepped further out by this same participant:
I feel like we [clinical team] are the arms and legs. The business model is the brain. And the community is the Heart. That’s the whole organisation. SF11
Such expressions appear to reflect a deep sense of belonging among the clinical team, both within the team, more broadly within the entire mechanism of Little Haven Palliative, and finally as connected within the entire community itself.
The clinical team also look out for each other in a very dynamic way in the day-to-day practice of Little Haven, with individual team members sustaining awareness of the operations of the team as a whole, and responding protectively as needed:
When a household is particularly tense or sad, we’ll look at the list as say ‘[staff name] has been in there for three days running, so we’ll put [staff name] on another run for a little while…we’ll make sure that that household gets shared around, like consciously…very consciously… SF10
Team members hold a deep respect for each other, understanding what each are giving within their professional roles:
And just that there’s that respect for the other staff members that you know, everyone’s you can, everyone, our nurses, just bring so much to the table in there of who they are as a person and what they’ll do and everyone goes way beyond especially when they’re out on their own on the weekends or on call or overnight. Like no one ever doesn’t do the work because they didn’t want to get out of bed, right? Everyone does what they need to do for the patients. SF4
The personal time of clinical staff who are not on shift is also protected by other members of the team:
We don’t fill a shift. If someone rings in the morning and says I’m not coming in, we’ll probably just juggle the list and see if some of the patients could do a phone call and stuff like that. It’s really unlikely that you will ring around the rest of the staff and see if anyone is able to come in this morning. That just very rarely ever happens. SF11
3.6.5.2 Satisfaction, meaningfulness and the privilege of caring
Threaded throughout the focus group discussions, was the satisfaction experienced by team members inrelation to their work. There also appeared to be a perception, or experience, that this satisfaction was protective in relation to the potential impact factors of working in this field:
Job satisfaction is massive. Massive when you have the amount of vicarious trauma, vicarious grief that palliative care brings to your professional life. It’s very rewarding work. You know, people say all the time, it’s depressing. It is not. It is rewarding. It is beautiful. SF10
It is a privilege, I think that that’s how I feel every day. I love working with patients and families. It just, it does feel like very privileged position to be in. You sometimes work half an hour late. You know, that’s really nothing compared to how it feels to be able to help these people in that moment. SF2
Lucky honestly for me, I feel that it’s what I am supposed to be doing. I feel incredibly comfortable doing what I’m doing. It’s an incredible honour to do what I do. And just the knowledge that you are making that difference with these people. You walk into a house and these people are so scared, they’ve just been told they are terminal. They have been given this unrealistic prognosis of how long they are going to live and they are scared. And you walk into that house and you go, hi, I’m [name], I’m from Little Haven, and everything is going to be okay. And you talk through what is going to happen and what services we provide, and that we are 24/7…We are frequently in dishevelled in people’s houses at two in the morning. When you walk out the door, they are calm and relaxed. That sustains me that the knowledge that I am doing that. SF11
3.6.5.3 The monthly meeting
Each month, the Little Haven staff come together and participate in a comprehensive review of the previous four weeks. Each death of the preceding month is introduced and reviewed from a multidisciplinary service perspective, with attending to case specific communications, tasks, updates and planning. There is a holistic holding to these meetings that is congruent with the tenets of the model itself. Each month, the meeting commences with a meditation and self-care grounding exercise, supporting staff to attend and hold quiet space, and to become aware of their own needs in these moments. Multiple participants referred to this meeting as a significant element within their workplace, from which, or through which, they were evidently resourced.
We have team meetings every month where there’s a meditation that is sort of directed at what kind of month we’ve had. A lovely social worker … will find some sort of meditation that matches the vibe for the last month. We discuss whoever has passed away in that last month. Every one of those people we get to discuss what was good, what was bad, what people we were happy with. Nothing is ever just ‘it doesn’t matter’. I’ve never worked in another line of nursing where you don’t have to just suck it up. But that is not what happens. Everybody has an understanding of the needs we have that support each other. I think that’s what is so incredibly different about it. SF11
It’s just such a comprehensive review of what’s going on in the last month we address each death in the last four weeks, and even the following month, we get to say Hey, [colleague 1; colleague 2], did you catch up with [patient]? Yes, they’re doing very well. And we get that feedback. Right? Well, yeah. And then we might also get something from a social worker where they might say, hey, look, if you’ve got time, could you just keep them a little call? Because they want to reach back to that? SF10
Crucially, the monthly meeting is also a recognised place where staff can voice any concerns that they have, with a feeling of safety:
…that opportunity to express concern is on the table all of the time. That monthly staff meeting. AGM another opportunity to be heard and see what is going on behind the scenes. All very, very transparent. If you want to want to talk about anything….you just chuck it out there and it gets talked about… I can’t think of anything that would be too testing to walk into the business manager and blurt out ‘wow I want to talk about this at the meeting’. This is key, because they’re the things that erode your personal spirit, and your job satisfaction. They’re the sort of thing that wake a woman up in the morning and rob her of her vitality the next day….The things that lead to burn out. SF10
3.5.10.4 Risk assessments: keeping the team safe
Members of the clinical team can frequently travel regionally and sometimes remotely, day and night, providing care into people’s homes. Safety is a consideration for team members and prioritised by management.
I have a responsibility to keep the staff safe. So, we’re doing risk assessments. And we do do backup of each other, I hope. No person should walk into an environment if they weren’t feeling safe. But I think we have probably only had three patients that we’ve had to call and say, this is challenging, and we moved to act. One of them we put on hold for a few months until they sorted out some social dynamics. SF1
Team members also presented as pragmatic in relation to potential risk in the workplace:
Community nursing is a high-risk job. And you know that coming into it, but I think that the right people do this job. Where instead of seeing that as a tricky road, we say, oh, this looks fun. SF3
It was also noted that risk mitigation training was a constituent component taught within the mentoring process.
…and that’s when you also learn the risk mitigation stuff for convenience. And like, make sure you always have an exit strategy. If you feel uncomfortable. Call back to the office and let someone know, like all those things we do automatically. Yeah. And if you haven’t done it before, that’s when you learn that in that, that period of time. You know, when you park somewhere, make sure it’s easy to get out. SF3
Finally, the outreaching members of the Little Haven team are embedded in a strong communications structure and process that ensures regular contact with them throughout the day while on shift:
We’ve got good systems in place to be able to connect in. We use [name of program] on the computer. So that’s a really good system that we can, you know, make sure things are uploaded and happening, we’ve got a good email system, texting system. So we’ve in communication with all of our staff, mainly or full, like all of the days, even when people are sort of out of areas, because there’s quite a few areas that don’t get service. So you’ll often by yourself out in the area that you can’t really contact in. But it’s that open door. SF4
3.6.6 Challenges
Interestingly, inquiry regarding potential challenges experienced in relation to the model appeared to prompt more pause, and consideration among the participants than all other inquiries offered within the focus groups. When participants spoke in acknowledgement of a challenge, it was brief, with the direction of language and discussion turning quickly towards more positive resolution language. A pattern that is perhaps reflective of the general problem-solving orientation that the team bring to their work. Two subthemes emerged in this discussion: the challenge of flexibility, and challenges experienced in relation to expectations that Little Haven provides an inpatient hospice service.
3.6.6.1 The challenge of being flexible
The capacity of Little Haven staff to work very flexibly with patients and carers across time in relation to their presenting needs, has previously been identified as a strength of the model. Interestingly, this flexibility in practice has also been identified by some staff as one of the significant challenges of the Little Haven approach, indicating that there is a weight of service associated with this factor, that is borne with an understanding of the benefit that it provides:
It is challenging having to work in a flexible environment all the time. My diary never looks like 8-8.30 and 8.30-9. There has to be flexibility built into that to allow for unexpected dropins. A gentleman dropped in today unexpectedly who I have been trying to get to come in since his wife died, and I was just able to attend to him immediately. And you know what that will have done is just so much greater than so much other work that I could have tried to do. It is a very rewarding way to work. SF2
It is about constantly looking at workload and shuffling. I never book appointments backto-back… the satisfaction from the work, knowing that you’ve met that person’s need is far more overwhelming than the sort of juggle that you might have to do. As a worker, it’s very satisfying being able to have that flexibility. But it’s also a challenge. SF2
3.6.6.2 We are not a hospice
The common assumption that Little Haven is an inpatient hospice, and the current inability to provide this service, were identified as related challenges by participants.
We’re often assumed were hospice, right? So people often ring us and go, okay, so [name] needs to come in to you now. What do you mean? And then you could have that conversation. We can look after them at home and work out their plan and everything. But there is that assumption from new practitioners coming to the area that that’s what they assumed that we are. SF9
It is interesting that this assumption has arisen with newly arrived practitioners, potentially identifying a target population for an information session regarding Little Haven’s current (and future) scope of service. Community members may also hold assumptions about the service in this regard if their own understanding of the dying process does not incorporate a belief or scenario of dying at home. Little Haven holds regular ‘Dying to Know’ days within the Gympie region, with a view to raising awareness regarding the choices open to individuals as they approach death.
3.6.7 Deeply embedded in the community
Community is a living, breathing presence within the discussions and thinking of the Little Haven clinical team. Its existence as the source of the beginning of Little Haven is acknowledged, growing from community member Phyllis Little’s desire for better care for the dying within the community. Since its inception, the community of Gympie has generated hundreds of thousands of dollars a year in fundraising, to support the existence and function of its palliative care service. Community gave and still gives, and community members were, and continue to be, active in the development and implementation of fundraising activities, many because they had already had a personal experience with Little Haven, themselves, their parents, partners, children. The volunteers sell raffle tickets, work with the Gold Festival, the Glitz and Glamour shop, support fund-raising walks, coffee mornings, bake, make preserves, attend and support awareness events. Others volunteer within Little Haven itself, supporting vital functions of the service:
The volunteers keep you honest as well, with that accountability to community, they give you so much. And in terms of that family or patient, feeling supported by their community, when they’re going through a really challenging time, having a volunteer involved or knowing that people in their community are raising funds for the nurses to go into their house, it really helps their connectedness to community as well. So we’re having more and more people move to this area, who haven’t been here for 500 years who don’t know about how Little Haven started and haven’t generationally have been able to live with us. But they’re just so feel instantly connected to community when they find out that it’s the community that puts us here and supports us to be here. So it instantly links them in where they might have moved from a very long way away and feel disconnected at their end of life from their family of origin, their community of origin. They instantly feel connected to the community. I think that’s really valuable. SF2
With the involvement of so many volunteers, over so many years, there is every sense that the Little Haven model may not be able to be separated as a distinct entity from the community in which it has developed, but rather represent a structure and process that holds reflections of its context.
In response, the community conveys its deep respect and appreciation:
Like any sort of circles when people when I’m socialising outside of work, not uniform. What do you do? And I go oh, I’m one of the Little Haven nurses, they all just instantly go ‘Oh, you guys do an amazing job’. Like, there’s no one that goes ‘sorry, who’s that?’ Right? Never. Yeah, in this community they always know who we are. And if they haven’t personally had it, someone that they know, has had our care. SF3
Notably, this is not a view held by all participants in this data collection, which is discussed further in reporting on volunteer and stakeholder views below. Nevertheless, the high regard in which it is widely held is noted:
I find that calling people for bereavement support, and all you have to say is Little Haven and they just feel safe. So I found a building rapport with someone over the phone to provide counselling they just instantly… It’s like you’ve already been in their home even though they haven’t met you personally. As part of that team that nurtured them so well, they have this trust. It’s really quite special. SF2.
3.6.7.1 Engagement with pharmacists and GPs
GP and pharmacist input are an integral component of home-based palliative care. Participants reported the development of strong, supportive relationships with a number of local pharmacists and GPs with whom they regularly work.
And even to the fact I think the pharmacists, you know. [We had a] local pharmacist join our Board who said she noticed a lot of families are very distressed when they’re sitting waiting for their medications because they’re waiting to pick up the things for syringe drivers. She said, we’ve decided we’re going to deliver those to the home and we won’t charge … for the end-of-life medications. That’s just compassion spreading through community. And so she just felt that they shouldn’t have to sit in the pharmacy. SF1
A lot of pharmacists are also very responsive to us, if we ring up and say we are from Little Haven, they will put whatever we need ahead of the other scripts that they need to fill, because we have a timely response that we need to do. And, you know, some of our pharmacists are trying to carry more of the meds that we need in an instant. SF6
And I think, you know, the GPs take the call from a Little Haven first, you know, whereas they don’t from other places that might call because they know Little Haven nurses are calling for no reason. They’re not going to waste their time, they’re going to know that patients, they’re going to give an accurate handover. And so they’re willing to take that call. SF2
We’ve taken on people a bit further afield, because pressure from Queensland Health, I guess, but there’s a gap in services, there’ll be further beyond our boundaries. So we said we could take people on, but really, they’d be the end-of-life people. It’s a long way for us to be travelling, but those GP surgeries are just blown away by the level of care. SF1
It is interesting to consider these second-hand reports of GPs’ views, as they are validated in the interviews with the GPs explored below. Although not directly addressed, there is a sense of a thread here that relationships with Pharmacists, and GPs are attended to within the Little Haven model, as an extension of the relational focus of engagement and care. These services are important to patient care, and as such are important to foster. In turn, the fostering of such relationships is facilitated by the excellence of the model of care that Little Haven staff provide.
3.6.7.2 Promulgation of the Model
The idea that the Little Haven model of palliative care is intrinsically connected with the community in which it is situated is reflected in one participant’s consideration that it is a model that can seed elsewhere, but not generalised or expanded to encompass elsewhere:
It can be replicated in other communities, but we can’t be a service that goes [and sets ourselves up in] other communities, it should grow out of that community, because it is so important to have that basis and the respect of the community and to have the responsibility back to your community. So getting that through to Queensland Health is proving more difficult than I’d hoped. I very much have encouraged other communities to develop a model like Little Haven, yes, but they need their own Little Haven. And it needs to be their community’s answer to what they need. I believe that. I was incredibly disappointed QHealth did not support those community models when allocating the most recent funding. SF1
A thought from another participant:
That would have to be a part of the models, [if] you’re going to try and regenerate the model anywhere else. I think you have to start with community awareness of death and dying and the potential to have better life transitions. SF10
3.6.8 Future Directions
Consistent with the discussion above, a primary line of envisaged growth for the current model, is the hoped for development of an inpatient hospice within Little Haven’s model of care. Key rationales for this suggestion are twofold. An inpatient hospice will enable Little Haven to provide continuity of care for Little Haven patients who elect not to die at home or do not have sufficient support there. Further, it will enable Little Haven to offer a respite service for carers:
Imagine 88-year-old Mabel and 92-year-old Frank… they can’t do it at home on their own. It’s just not humanly possible. Having an actual homey space that you could bring them into would be nice. SF10
A further potential development sits in the concept of a social work-qualified Care Coordinator who could facilitate effective integration and training of carers contracted by other services. This has already been trialled with a short-term grant, and holds interest as a potential point of future exploration:
So for a while we talked about having a carer, and we employed a carer, but we weren’t getting enough admissions to keep that role going because people often have their care packages. So instead, we’ve probably built up a social work position where they engage more with other care services so that we’re maximising what we can get out of aged care packages for that family. That’s like a care coordinator, which is currently being funded by the PHN to trial that for six months to see how that works… For us, it’s all about improving services into the home… I think there’s been a great advantage in further developing those relationships with care providers so we’re not both going in in isolation. So we’re sharing that role more. SF1
This development will extend on the existing engagement of Social Work team members in relation to care applications and similar, that has provided support for nursing staff within their documented care coordination role:
We used to spend a lot of time doing things like advance care directives, my aged care applications and the follow up phone calls to Social Security, introducing patients and carers to JPs. It was not a nursing role, but we did it, and then, our social workers came along and took on these roles, and we could then see even more patients on the road… SF10
3.6.9 Summary
Participant staff members within the focus group study demonstrated confidence and belief in the Little Haven model of palliative care. Staff members clearly enjoy what they do, believe that they do it well, and are affirmed in their practice by patients and families, management, their colleagues, and the community of Gympie. Staff are able to identify key strengths and benefits of the model and point to organisational structures and processes that promote sustainability. A high degree of congruence exists between the tenets of compassion, care and support within the model, as offered to patients and carers, and the caring orientation of management, staff and volunteers towards each other. This is a service and a model that recognises itself to be situated deeply within its community and upholds its responsibility to that community.
In return for the community investment in it, Little Haven provides members with holistic, immersive, multidisciplined, high standard palliative care, free of financial cost to the patient and their family. Community members are offered the experience of being held deeply by their community, as they move towards the end of their life. This care is extended beyond death, in the form of bereavement support, and attendance at funerals and a yearly memorial service, where those members of the community who have died in the previous year are remembered.
In considering the components and expression of the Little Haven model of palliative care, staff identified several points of difference between Little Haven and other palliative services within which they had previously worked. These included that Little Haven i) offers a much earlier point of engagement with patients post-diagnosis; ii) is much more flexible in its capacity to meet patient needs on a day to day and overarching basis, and in its support of patient preferences; iii) that the Little Haven model provides greater levels of support for family and carers; iv) that the model integrates care coordination; v) that new nursing staff are offered a substantive time to orient to the Little Haven model of care with a one month mentoring process, and vi) that Little Haven demonstrates a higher rate of staff retention and longevity.
There is ongoing interest in actively encouraging other communities to seed and develop their own version of Little Haven, that will perhaps share elements of their model, while also being informed and flavoured by the particulars of the community in which it sits. Current plans to develop an inpatient hospice will enable Little Haven to provide continuity of care for Little Haven patients who elect not to die at home or do not have adequate support there.
3.7 Focus group: volunteers
Analysis of the data generated from a single focus group (n=13) identified x emergent themes. These are listed in Table below.
Table 12: Emergent themes: volunteers

3.7.1 Becoming a volunteer
Many participants reported personal experiences as family members cared for by Little Haven, sometimes from decades ago. It was not always considered a simple step from carer to volunteer:
My partner had cancer, and I had Little Haven come to me, and it was the best thing I ever had. And I had some wonderful nurses. Angels without wings, I call them. That’s how I started, it took me a while after he passed away. To get up the courage and go and do it. VL1
My sister, we’d looked after her or her daughter and I looked after her at her home her daughter that’s 24 years ago. And after she passed I decided that I’d join little haven. So I’ve been with them for 24 years and chemo, respite, raffles, cooking scones. VL7
It was seen to be valuable experience to bring to the role, although there was a strong sentiment of ‘giving back’. Indeed, one uncharacteristically young volunteer (not present) was noted to have this motivation himself:
We got one young one, he’s 16. We looked after his grandfather, he’s paying it back, he’s in grade 11. We’ve got one more year of him. VL5
However, there were some volunteers present whose path to volunteering for Little Haven did not include personal experience of being a carer. One participant described how she decided:
…to help move the books from one of their book sales one year, and then in the next year or two, I just went up as this person and did it and … I’ve been volunteering ever since. VL2
Another participant (male) reported that, after retirement, he was:
…always looking for something to do. I was just sitting around at home and another lady was a volunteer out there in the office and she put my name forward and they had the introduction day so that’s when I joined, been there for the last five years. VL5
Interestingly, others came with professional experience in palliative care:
[JR: So you’ve come to volunteering with a background in palliative care?] Yes, I worked at Little Haven as a nurse, from the 1980s … They were all wonderful. Then after that, I volunteered. VL13
3.7.2 Community awareness of Little Haven
There were mixed views about the extent of community awareness of Little Haven in Gympie and surrounds. The shopfront was seen to be a pivotal interface between Little Haven and the community, but even there, awareness varied enormously:
A lot of people know about Little Haven, but a lot of people don’t. We run a marketplace … and a big surprise is how many people ask you what Little Haven is about and where does the money go? And a lot of people out there we deal with, a lot of people every day… but people out there don’t know what Little Haven is… You get a lot of the young ones coming through, they don’t know what Little Haven is about. VL5
Other public-facing volunteering for Little Haven was also seen as a valuable way to raise awareness, such as the ‘Happy Wrappers’ who wrap Christmas presents in a local shopping centre, using the opportunity to chat:
I think meeting and greeting people is often a really important thing about how you talk to people and tell them about Little Haven … because they will ask you while you’re wrapping. Yeah, lots of communication while you’re wrapping their gifts. So that’s all December, for Christmas. VL4
Participants were clear that, where Little Haven was known to community members, it was held in high esteem. They could see it as a service of ‘care and compassion … shown to the family members’ (VL9), where locally raised funds remained in the local community.
There was one other thing that stands out this Little Haven and whatever money is made, stays under the Little Haven umbrella doesn’t go here, there and everywhere and everybody gets a bite out of it. It stays in Gympie and the surrounding district, and that I think is makes it so much more … they’re very personal. VL7
Remarkably, as a ‘flood town’ who experience major flooding in February 2022, this participant described how, faced with the certain flooding of the Marketplace:
…help came from everywhere to help out to ship stuff out and put stuff back. And with those people, they weren’t, they weren’t volunteers. They just helped. [JR: That’s a bit of a measure … of how Little Haven is viewed by the community? That people would pitch in and help?] That’s Gympie as a whole. Everybody pitches in here when it’s flood time. Everybody. VL6
This was viewed by the group as a clear example of how, as a community, Gympie views Little Haven as ‘theirs’.
3.7.3 ‘Above and beyond’
There was general agreement amongst participants that a clear feature of Little Haven was that it is known for going ‘above and beyond’ what might otherwise be provided. This volunteer, who had been a carer for her husband, experience this firsthand:
The nurses go, you know, they’re 24/7. When my husband was sick and couldn’t believe that the nurses were 24/7 and [name] was one of the nurses that looked after my husband. And “anytime, just pick up the phone just ring me” 24/7 Who gives you that? Some places don’t even give you that, it’s like, “Oh, go somewhere else.” VL12
Another was keen to point out the impression made decades ago by a Little Haven nurse now volunteering and present at the focus group:
This lady here [points to woman beside] was a nurse. A retired nurse. I saw her at five o’clock in the morning in the palliative care ward. She didn’t finish work until eight o’clock that night. Yeah, that’s what the nurses do. VL7
3.7.4 CEO’s role is vital
The CEO, Sue Manton, was very highly spoken of by participants. Her principal role in pursuing funding sources for the organisation was acknowledged: ‘We’ve got a very good manager in Sue Manton. She works really hard for funding and everyone really’ (VL9) and ‘She chases every dollar’ (V5). This participant saw the CEO’s role as central to the growth and quality of the organisation:
I just watched Little Haven grow from a very small organisation to the large one it is today, and it’s a wonderful organisation, I just believe that Sue needs access to more funding to do all the things that she’d like to do. VL13
Moreover, as a manager, she was praised for being at the coalface and supportive to the volunteers’ work, for example:
If it’s a function, she’s in there getting her hands dirty as well. She just doesn’t say “Do this. Do that.” She’s helping. VL12
This concern for the wellbeing of volunteers was also experienced when volunteers were themselves sick:
She knows what we’re all doing. I think sometimes. She does know what we’re all up to. Or if we’re, if we’re unwell. Like I mean, there’s been times when everybody’s probably had something medically wrong with them, but Little Haven actually will ring you and say, “How are you going? Is there anything we can do to help?” VL4
3.7.5 Sustainability
All participants acknowledged that the nature of volunteering is changing and that, with time, fewer and fewer volunteers are likely to be available and willing to support the work of Little Haven. Some felt that the situation was manageable for now but not indefinitely:
While we’re all going It’s great. But in 5 years, there’s probably going to be half of us not volunteering. Yeah, so who’s going to replace us? VL4
Although it was suggested that finding ways to recruit younger volunteers, once participant did not view that as a realistic path:
I know that the younger people aren’t gonna volunteer. Their mindset is completely different. Some of them are there talking about being paid. Others, the whole thing is … life is completely different nowadays. People once, they got cared for. There’s less caring in society, a lot less caring. And I suppose if you’re not cared for, you’re not willing to care for others. And there seems to be a lot of that. VL11
Indeed, the same participant viewed this challenge as a bigger issue than how Little Haven operates:
I think volunteering also has a lot of problems with governance. There’s lots of restrictions. There’s lots of government restrictions that get in the way. Lots of them, including insurance. You know, you can’t do this, you can’t do that. And… or you have to, and people get really peeved off. I’m peeved off. I don’t I don’t think it’s an organisational thing. I don’t think it’s a volunteer thing. I think it’s a societal thing… VL11
Nevertheless, it was something of an exceptional week for recruitment, with the Marketplace reporting that there were ‘three or four new ones this week? One coming up tomorrow’ (VL5).
3.7.6 Future directions
Participants viewed the future as a challenge for volunteering specifically and for Little Haven more generally. Raising public awareness was seen as critical to facing the challenges of the future, and opportunities were seen in the Marketplace:
Well, I think down at the Marketplace. We need to put more information out, what’s Little Haven? with our signage. Little Haven Marketplace. That could be anything. Palliative care: have you heard that word there or not? “Little Haven Marketplace”, it might give people a better idea. VL5
However, raising awareness was also about enabling the Gympie community to understand how it is that they have an organisation like Little Haven running at all:
… everybody in Gympie can know more about Little Haven, what they do and what they stand for, and why we do what we do in Little Haven … like, you know why we get the funds when we sell raffle tickets, because that’s how we run Little Haven. Because like, when someone is sick, they bring out the equipment and all that and look after them. We don’t ask for anything. So how are we going to run if you don’t have all these people behind [it]? VL12
Securing government funding was also spoken of as an essential consideration for the future, alongside community fundraising and corporate sponsorship:
Funding from the government. I think you have to keep pushing the government for palliative funding. Little Haven is just based on all the funding we get from the community. Yeah, I know there’s others from the government, but the community funding pocket contributes an awful lot. That and there’s everybody else in Gympie trying to fundraise and keep their organisation. So it becomes harder to raise that dollar. VL4
I think the big businesses in town, some of them are very good, that’ve contributed to Little Haven, but probably over the next five years, if they could volunteer, give a car for the nurses. And they break down. They have a breakdown in their car. Sure. Yes. They could be the big company that could help out nurses all those big places that give out a helping hand which would be good for the community. VL7
Interestingly there was no mention of Little Haven’s plans to build an inpatient hospice, as identified in strategic documentation and other data collection in this evaluation.
3.7.7 Summary
Participants in the focus group had largely become Little Haven volunteers following their own experiences as carers or family members, and, for some, the experience was decades ago. Others came with professional backgrounds in palliative care nursing, but all viewed their decision to volunteer as worthwhile.
Like others, these volunteers observed what they called going ‘above and beyond’. Whether in their care of patients and families, or their care and support of volunteers, Little Haven as an organisation was held in high esteem by this group for their compassionate response to need. The CEO was singled out in this regard.
The volunteers observed that community awareness of palliative care varied – for some who work in public spaces, it was both recognition of Little Haven and unfamiliarity of it which they encountered. Many of their reflections about how Little Haven could improve both its volunteer recruitment and funding in the future related to the profile of the organisation in the local community. Sustainability of the volunteer cohort, in the face of changing social roles and expectation, was the source of concern for many. Similarly, ongoing funding requirements was seen as a risk for the organisation and one which they acknowledged the CEO in particular spent a lot of time and energy pursuing. The prospect of a day respite service was applauded as an appropriate development in the model of care.
3.8 In-depth interviews: key stakeholders
Analysis of the data generated from these interviews identified these emergent and interrelated themes referring to PEoLC. These are listed in Table below.
Table 13: Emergent themes: key stakeholders
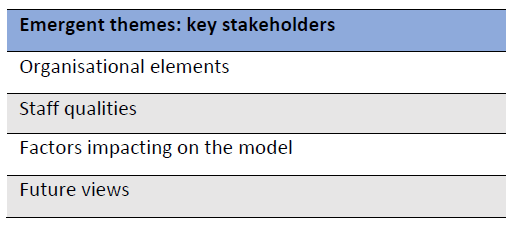
3.8.1 Organisational elements of the model
A range of organisational elements reflecting many of the common elements of models of care illustrated in Figure 2 in Section 2.2.4 were evident in the data obtained from key stakeholders. These are explored further below.
It was noted by each key stakeholder that the quality of clinical care provided by Little Haven was of a very high calibre and clearly patient-centred; their goal to prevent avoidable hospital admissions was clear:
The standout thing is that not only do they have a good skill set, but they are very patient focused, and they will do what it takes to try to deliver the care that the patient wants in the patient’s preferred place of death, as best they can. SK1
I think that Little Haven is pretty much switched on to keeping people out of hospital as much as possible, you know at the final time at home. SK6
Little Haven is known locally for its responsiveness to referrals, which are attended to promptly, with no waiting list:
I think one of our most important aspects is we won’t turn anyone away; we won’t cap their numbers. SK4
Another GP was impressed by the simplicity of referral processes, which can be very challenging in other services:
I had somebody that I felt might benefit from our view by Little Haven. I called them up, and they have been very responsive, which is terrific in any service, you know a lot of the services we have … can be difficult to deal with, and I found that that it’s (Little Haven) been exactly the antithesis of that. SK6
In keeping with their stated intention, Little Haven will accept referrals early in the illness trajectory, including upon diagnosis (as described in many palliative care documents as the most desirable timing for referral).
And we won’t wait till people have a crisis of three months. So that early intervention, I think we’re well known for the fact that people can walk from the hospital where they get a diagnosis or prognosis of a life limiting event. And they’ll walk straight down to us at that moment. And that’s when they go on our books. It’s very much an open-door policy and early intervention and not turning anyone away. SK4
The benefits of early intervention are well established in the sector and published literature, and were extolled by this GP:
All the studies tell us that you know early referral into palliative care services improves your life quality, your longevity… looking after people, we need to do it early. SK5
However, when early intervention was not possible due to late referral, Little Haven are still able to respond, and in this example, it was possible due to their organisational practice of not turning anyone away:
I don’t think that there is any other service that offers that kind of support. A few years ago, I had a palliative patient who … was actually under one of the other organisations in town who were purporting to do palliative care business hours, Monday to Friday. 4 o’clock, 4.30 rolled around, they were uncontactable, and it was a woman in her fifties who was going to die. Most of this stuff happens out of hours, and her family needed support so thankfully, Little Haven took her on, because the other service just couldn’t offer it, and they eventually admitted that they couldn’t offer that. SK5
One local GP observed that Little Haven’s accessibility is a component of their model of care that makes it accountability in a regional town where the population is small and the connections are strong; indeed, rejecting immediate access can have a social cost.
Little Haven Doesn’t turn anyone away … It is a community organisation responsive to our community’s needs. It’s pretty hard to turn down someone when you know that you know the next week … like we’re buying our jams and going down to the Little Haven shop, and you know it’s very much ‘everybody knows somebody.’ You have to be accountable for your actions. SK5
It was also noted by clinical stakeholders including GPs that the Little Haven staff have advanced knowledge and skills in palliative care that are applied to practice and enable trusted interchange between Little Haven and GPs. This is especially the case where the GP might not be fully aware of the patient and their circumstances (e.g. when they are on call for their practice) and the trust in the nurses’ clinical judgement enables appropriate care to go ahead.
You might get requests from patients you won’t necessarily be looking after, as you know, my own patients, have been palliated … where the practice will be ringing up saying “This is what we recommend” and you know, they’ve got such a wealth of experience that you’re happy prescribing a script or give a phone order. I think being that segue for the family, so that that stress is taken out of it SK5
My main interaction was working in general practice with Little Haven, and particularly in the care of several patients in their palliative journey, both in terms of their initial contact service and their subsequent active palliation, where the Little Haven nursing team were the stalwarts of it, and we as the medical clinician side were guided to a large extent by what they do. SK7
The 24-hour, 7-days/week availability of Little Haven nurses is a service feature that this GP identified a range of benefits from, not the least of which is being a local service rather than a general phone number.
Being a point of contact for the family, a local point of contact, as well as opposed to some visiting service. So that sort of thing might be some of the bigger picture stuff, but also just some of the nuts and bolts of getting syringe drivers, the medications, being that link in with the primary care doctor, who the primary provider is for that patient, just in terms of getting scripts. And over the weekend as well. SK5
Further, this trust is noted by these GPs which also has them recognising that if it is a call from Little Haven, they can be confident that the request is well-considered:
You know that would be my first port of call and I think you know in the two years that I’ve been there I’ve only done one house call for a palliative care patient. I’ve been confident enough in Little Haven because their feedback is prompt when there are any issues, that was anytime about that, getting in touch and I tried to respond as quickly as I can because otherwise the interaction doesn’t work. SK6
They’re proactive with proposing ideas and suggestions of what they think is needed in the next stage, and that that is so valuable and helpful, because that is, I can’t do home visits all the time. They’re so valuable, they’re like the sort of extended eyes and ears of what I can’t see, and that they have all this experience with them, sometimes their suggestions I wouldn’t have come up with myself, so they would ring me if they have concerns. They send me a fax or an email proposing, you know they have to text in an infection, or the pain is not under control, or they wonder if something else will be valuable. SK8
Little Haven’s bereavement support service is known about in varying detail amongst the stakeholders; this GP engaged with it:
I’ve also referred patients or family of patients to them, where the patient had passed away in their care. And then the family was struggling … if Little Haven was really involved, I would often go by their advice on what to do the next step. So I feel there’s a Little Haven that is so experienced, and so on the ground with the patients, I’ve never found their advice not good or not helpful, SK8
The published literature has suggested that the highly regulated Nurse Practitioner (NP) role, described in Section 3.1.5.2 above, may assist community-based palliative care services to deliver care where a depleted workforce presents systemic challenges. This proposition treated with caution by this GP, who reported that they have, and do work with NPs in other settings; their rationale for the inclusion or exclusion of NPs from Little Haven was highly driven by their reflections on better outcomes for patient and continuity of care:
… if that resulted in better care for the patients, which is what it’s ultimately about, I think it’s good thing, but if it subsequently results in a loss of that interface between the hands-on-the-ground nurses caring for the patients and … the GP who has been looking at them … I think that could be a bit of a loss if that some of the nuts and bolts of the troubleshooting went to the NP … I guess there’s a closed circuit where the patient is … receiving active palliation in the community, and the treating team didn’t hear anything, all because the NP was able to write the appropriate script, I think that would be a bit of a loss to this service. SK6
Another GP was unequivocal in their opposition to a Nurse Practitioner, seeing instead that, between the GP and the Little Haven nurses, the care needs are addressed already:
I honestly don’t want to share my work with a Nurse Practitioner. In this circumstance, I’m not sure how a Nurse Practitioner is going to fill that role in terms of the Little Haven nurses (who) go out there. They do what they do best. They’re contactable24/7, I’m not sure what a Nurse Practitioner could actually do above what they already do. The only role I could see a nurse practitioner playing would be if that patient didn’t have a GP. There’s great value in continuity of care … there’s such value in looking after someone and their family and going out and seeing them in their home and then looking after their spouse after they’ve died. SK5
3.8.2 Staff qualities
Strong descriptions were given of the deep-seated, values-driven motivation of the staff in doing the work of Little Haven. This excerpt also expands the descriptions of the ‘boutique’ character of the organisation:
These women and men that are involved in Little Haven, they come from a place of their heart. Yes, it’s a job, but it’s, it’s a calling for them. When you get too big…I’ve seen that sort of change over the years because it’s got bigger, and then it goes, you know, interstate and it then becomes this big monolith. And it loses that genuineness about it, that innocent kind of just loving kind of organisation. And that’s how I see Little Haven. These guys are genuine and give from the heart and nothing is too hard. And that’s the beauty of them. SK1
This sense that ‘nothing is too hard’ was articulated further, leading to the next subtheme.
I have great comfort in the fact that they will cover those questions that patients and their families will have after hours, that they will take care of those questions because they’re specialist. But the nurse is awesome in those last few weeks. They go out regularly… saves me from having to go out every week. I might change it to once a fortnight or once a month, depending on what’s required. SK5
3.8.2.1 ‘Above and beyond’
Many examples were given by participants illustrating ways in which Little Haven has gone ‘above and beyond’ in their provision of care in their geographical setting. Notably, during the major flood in February 2022, where much of the town of Gympie was inundated, the efforts of this Little Haven nurse were lauded:
So, you know, even during the floods, so this happened last, during the floods, the nurse was on who was on call, her house was flooding at the at that exact time as well. And we had patients that we still had needed to care for, within this flooded region of Gympie. And I was on call and she was on call, you know, and she put the patients first, her needs she put second… SK1
It was the source of some amusement for this participant that this event had gained legendary status within the town, with embellishments made by community members in the telling and retelling of the story. However, Box 2 illustrates an unembellished story of Little Haven’s efforts towards supporting a patient and his family living on a yacht moored by one the coastal communities near Gympie and the efforts required to fulfil his wish to die ‘at home’ (that is, on his yacht).
Box 2 : Key illustration
So they had to go out every day or every two days to this yacht, to manage the syringe driver and manage a young family w h ere the father was dying on this yacht, and it was t w o teenage, young teenage kids on that boat. And they’d go out there with the coast guards. So, you know, they take them out and trying to make sure that this man was allowed to die where he wanted to die, which was on his yacht. So, there’s not many nursing services that would do that. And that’s the honest truth. Most of them would see that as an occupational health safety issue ……. That’s certainly what it is. But they didn’t even bat an eyelid . SK1
3.8.2.2 Volunteer qualities
The dedication of the Little Haven volunteers was noted, and although there are challenges facing volunteerism in Australia, this stakeholder considered older volunteers more suited to the kind of work done by Little Haven:
Volunteers are essential everywhere and they’re absolutely essential. Without them, you wouldn’t be able to provide the quality of care that we provide. The problem is there’s less young people interested in volunteering. An older set of volunteers is probably a better group to have supporting people, though, you know, particularly families when their loved ones are dying, because many of those volunteers will have had similar experiences themselves. SK1
This was subject to the caveat that although this is mostly true, there are exceptions where younger volunteers are found to be valued contributors. Notably, the youngest volunteer at Little Haven is a 16-year-old male. Nevertheless, it was observed that Little Haven’s volunteer recruitment was not slowing down:
You look at the ages of the volunteering. You know where are the young people coming through? There is less volunteering. I feel. But I think that Little Haven, when you look at the different organizations in town, you know you look around and you go, well, that’s one of the ones that is still attracting. Meals on wheels is still attracting. Little Haven is still attracting there. Some, I think that are better known than others. SK5
3.8.3 Factors impacting the Model
Four key factors were identified that represented both organisational strengths of, and risks for, Little Haven.
3.8.3.1 Governance
Two of the key stakeholders were members of the Board of Little Haven, bringing unique knowledge of the workings of the organisation beyond its provision of care and support. Little Haven was viewed as comparable to a family business model:
I work a lot with family business, here and also work with [the] Family Business Association. So, I’m very interested in in how those two sort of models align. So, the way Little Haven works, to me, it’s quite similar to a family business where we have to be in control of, you know, the things that we want to work towards, and our future. And that was always a risk to with increasing our government funding. But we’ve been able to sort of keep that family business model. And in family business, we’re always taught that governance is so important, and succession governance, understanding that we are the stewards of for future generations. So, the way those two models aligned, I quite enjoy that. SK4
Little Haven’s growth over the years ahead is set for 9-10% pa, and this ambitious target brings with it specific challenges to service delivery in community settings:
That means keeping a nursing staff and also, vehicles on the road and kilometres driven. We cover a vast area. That’s really hard. So, the travelling that nurses do … if there was some way that we could limit travelling, you know whether we have nurses that that work in certain areas and service certain areas, but that is logistically, that’s probably the hardest thing. SK4
3.8.3.2 Funding
Little Haven’s changing funding arrangements were described by each stakeholder, noting its original reliance upon community fundraising:
It’s probably what’s assisted Little Haven, especially in the early years. In the last few years, we’ve been able to get some good State and Federal funding. But in the early stages, it was very much reliant on the community, with fundraising etc. to allow Little Haven to survive and grow. SK3
However, both its current asset position and its ongoing reliance upon Government funding for its continued operation, let alone projected growth, was the subject of much discussion amongst this stakeholder cohort:
We’ve been very lucky, especially with the State funding, it has been adequate in that it has allowed us to probably pay the nurses what they should be paid, right? Whereas in the past, there was always a funding gap there. So, what we’ve got at the moment, it allows us to continue operating as it is. If you were to lose that funding … especially as Little Haven has grown strongly over the last decade, it would be very hard to continue what we’re doing without that funding. SK3
Furthermore, a direct consequence of insufficient funding was linked to operational issues such as rapid response and hospital usage:
It all comes down to funding because the complexities of the healthcare system are immense. So, when someone’s in a crisis situation, what can we do more, and maybe that’s, that’s maybe something to look out for the future? I know, there’s funding that’s for end-of-life care… But I know there’s limitations on the funding… it’s just that having that dependency on the hospital… It’s never going to happen in the timelines and maybe [when] families needed. So how can we do that better in the primary health area, rather than needing to do that through a hospital system that’s already been funded? SK2
The absence of a secure, ongoing funding stream from government and increased cost of living impacting on fundraising, represent risks to the organisation’s longer-term operations, according to this GP:
One risk would be that they can’t financially afford themselves anymore, that they run out of money… You know, with cost of living going up everywhere, you know, salaries. If people stop giving money as much. That would just dry up and I don’t know how it is with staffing, but the amount of doctors is sort of drying up. I don’t know how it is with nurses, so I guess that will be a major risk. SK8
3.8.3.3 Links with General Practitioners
The General Practitioners interviewed for this evaluation were clear in their support for the organisational components of Little Haven’s model of care, and the quality of the care provided by its clinical staff. All four GP stakeholders described Little Haven’s involvement as complementary to their long-term, primary care of pre-existing patients who had become palliative:
I’m a GP that does, you know, from birth to death and you know I do all of it, and Little Haven allows me to really comfortably do the death part, because it is quite time consuming, and there’s an after-hours component involved. Because GP is really poorly remunerated. SK5
The capacity of Little Haven to provide home visits with a frequency responding to patient need was both clinically desirable and resource efficient for the GP, who could not conduct home visits further out of town.
Generally, the patients get home visits very frequently, and they have patients with have someone in their house who can actually observe how the patient is managing and how they’re coping in their difficulties. I found that much earlier than me in in my clinic room they can detect where things are going wrong or the patient is not coping. Often the patient here in my room, they say things are going fine, and then actually that that last couple of months they just can’t really easily come to the practice anymore. SK8
However, outside of these established working relationships between these four GPs and Little Haven, there are also structural and practice constraints to working with GPs in palliative care circumstances, leading to poorer outcomes for patients and carers, observed by this key stakeholder:
GPs are becoming increasingly uninterested in prescribing… general practice is pushed, my patients are constantly complaining. And we’re constantly being asked for scripts, because GPs are just not available, they can’t get into a GP for three weeks. GPs aren’t writing scripts, because you don’t get paid for scripts… patients actually trying to access medications is hard. SK1
Another stakeholder alluded to efforts towards improved communication with GPs, particularly when hospital transfer from home is being arranged:
If there was a little bit greater collaboration from the GPs in that process as well… But whether the GPs already seen the patient when there’s already been a review, you know, if that GP could then ring our medical officers – and in the background, we’re working on improved communication between the hospital and the private health sector, you know, the GPs – I think that may help to expediate the process a little bit through the emergency department. You know, for the for the improvement in the patient. SK2
Again, it is noted that this has positive outcomes for patients.
Little Haven participates in both raising awareness amongst GPs of palliative care and supports training of new GPs through hosting students.
We’ve had medical students from James Cook University come down, and I’ve been impressed enough with Little Haven, and been keen for them (the students) to understand that in home care is but possible and available, and I think you know an option for things, so Little Haven has been kind enough to allow the students to be attached with them for a day here and there, and the feedback has been very, very positive, indeed. SK6
Opportunities with the College of Rural and Remote Medicine were also identified by a GP who is quite involved with their programs.
3.8.3.4 Community attitudes to death and awareness
The engagement of the community with Little Haven was seen to rely in some part upon the community’s familiarity with the issues of death and dying, particularly in the context of an ageing population.
I think some of this is because we’re such a death-denying society really that you know I we’re death denying so why would you need to even prick up your ears and understand why Little Haven, what is it. So, death denying society? But also I do think that you know all communities are now really struggling with what is a community and trying to engage that community spirit and foster it. There is a lot more individualism now. SK5
This lack of readiness for the death of a family member has an impact upon the subsequent grieving experienced by the bereaved.
…if there’s increased grief, because they haven’t got much exposure prior to this point of people dying and losing a loved one, then then it requires much more support to be given by the nurses and the volunteers and social workers to try and help carry that family through that event. Support family members post death as well. So that puts a huge impost on what the service can deliver when there’s more and more people to care for. SK1
Most participants linked this death denial to a lack of awareness of Little Haven, as a key player in the region in matters of dying, death and grief, where interaction with the service elicits increased acceptance of dying. Other participants in this evaluation, such as volunteers, strongly linked raising awareness of dying and palliative care to lifting the profile of Little Haven among those for whom it is not so well known.
It was interesting to note the varying levels of awareness in both Gympie and surrounding districts of Little Haven. For this GP, in a nearby town, its profile was lower than in Gympie itself.
(JR: So how well known is Little Haven [in rural location]?) I couldn’t really answer that. I don’t think I’ve had anybody come in and ask me for Little Haven and when I mentioned it I can’t really tell you where the people say, “Oh, yes, I’ve heard of it” or not. I wouldn’t say it’s all that well known. I have you know several clients on the go … and as you would know in rural places the word gets around pretty quickly, both good and bad. I only came across Little Haven by chance. It wasn’t certainly because there was handout that’s available in the practice. That might be something that’s worth a bit of a publicity program with local practices. Put handouts, you know, leaflets in waiting rooms. So that’s a sort of thing that that might be considered in the continuing support and awareness. SK6
Nevertheless, this Gympie-based GP had a different view:
I think most people are aware of it. I think that it’s an institution that the community… just for those who never needed their services aren’t aware of them. But then it’s pretty well regarded and well thought of and is protective of it. It’s a service that, I guess, has risen to the needs of the community that I think the community’s proud of. I think they’re leaders in the community. SK7
3.8.4 Future views
The stakeholders’ views of the future for Little Haven can be noted in three main themes:
3.8.4.1 Funding
All stakeholders described funding as a key issue for the future, as noted above. Not all had detailed knowledge of the funding arrangements but recognised the critical role it has to play.
I guess I just worry that they won’t get funding. I work in a … funded program that we have to reapply for funding. And I think you know this, this idea of continually having to reapply every you know, whatever… I just think it’s absurd. It’s so cost-effective to do work in your own community. Not have people travel you know, long distances. Take up hospital beds. you know all the things … It’s just in saying that you have to continually justify your existence, and why you should be paid for that. SK5
To some extent, funding models can bring about the centralisation of services currently provided by rural organisations like Little Haven and represents a risk to the communities served in the regions.
One other thing that I think, is an under-recognised risk for rural services is a desire by departments of health to centralise things. So they need to change the thinking a little bit, and be reaching out to make sure that they are providing as much local service they can, because in the long term that takes pressure off big hospitals in the middle and the centralised services, so that needs to be a piece of awareness for Queensland and help for other government agencies involved in support. SK6
3.8.4.2 Building a hospice
There are longstanding discussions in many communities about the construction of a hospice building with inpatient beds, but these are not usually in the presence of an existing home-based palliative care service. Nevertheless, this is a clear plan for the future held by Little Haven and its stakeholders. A hospice building was part of the original intention for what became Little Haven:
They started raising money at that stage for an actual hospice in Gympie. And over the years, it became apparent that a community-based care model would be easy to get up and up and running, and also turned out that that was much it, we were able to meet the needs of our community in that way. SK4
Nevertheless, there is a now a definite plan for its construction as the ‘next step’ for Little Haven:
…that’s definitely something that we’ve outlined as part of our strategy going forward. And we’ve started fundraising for it. There’s a lot of interest in in town. I think too, with raising funds in the community, of course, people like something bricks and mortar that they can, that they can actually see that that’s where their money’s gone. I think that there’s certainly an appetite for it. And there’s, obviously, we’ve seen in the last few years, that there’s now an appetite for it with Federal funding, so it’s a good time for us to be to going into that as well. SK4
3.8.4.3 Succession planning
Like many small, community-based organisations, Little Haven has a champion in its CEO, Sue Manton. She is very much the public face and voice of Little Haven and is acknowledged by many as the primary driving force behind its success and sustainability:
She’s very passionate about it. And it’s been a good voice for her. Like she’s very well respected at the highest levels of governance in the health department too and she’s good and she knows it inside out and can communicate very well. Very, very passionate. She’s not afraid to put her views. SK3
Indeed, there was a turning point in the CEO’s role that enabled Sue to move beyond managerial role and harness these strengths to the benefit of Little Haven:
When we saw a change in Little Haven being recognised for our work at that stage. We had identified that Sue’s role in Little Haven was greater in our community at about that stage too. And I think we might have gone as far as … changing her job description to include advocacy for community-based palliative care in the greater region and Australia-wide as actually part of her role in our community organisation. So, recognising that it gave her the ability to step up on those platforms without feeling like she was overstepping the mark, so I think that was also important that that, you know, we recognised yes, she was a champion for what we do. But that could also be valuable on the biggest stage. SK3
However, it is the case that Sue’s time at Little Haven will end at some point, and for the organisation, this is a risk for its continuance with the loss of corporate history, strong advocacy and an authoritative public voice. This risk is anticipated at the Board level: It’s something we definitely are aware of, and we do work on it, I’m very cognizant of that. SK3
It has been noted that during a recent unexpected and extended leave of absence, the CEO’s role was filled, and the work of Little Haven sustained, indicating existing capacity for time-limited succession.
3.8.4.4 Promoting the Model
Little Haven sees an imperative in promoting its model of care within the healthcare sector. This was most significantly achieved through a substantial written submission and subsequent address to the Productivity Commission into Reforms in Human Services in 2017:
We decided that we would … send Sue to present at the Productivity Commission. And that was really a game changer for us. We didn’t want to be seen to be blowing our own horn, but she did a wonderful job. And when that report came out, and you go through the report and see how many times Little Haven was referred to… wonderful. And that gave us a tool to then to go to the funding bodies and say, this is this is really good, what we’re doing. SK4
The stakeholders’ views about the transferability of the Little Haven model of care are considered further in the Discussion section of this evaluation report.
3.8.5 Summary
These key stakeholders brought valuable insights into the model of care at Little Haven. Clearly, it is regarded as the provider of a very high standard of clinical care and other aspects of holistic care needs. The clinical staff are seen to be pivotal in this, and again, the notion of going ‘above and beyond’ was explored. Similarly, the volunteers were regarded as essential to the work of Little Haven and at no time was there any indication of hierarchical views of staff versus volunteers.
The relationship between Little Haven and four GPs was explored in these stakeholder interviews. There are strong and trusting professional relationships where patient-centred care, support of the family and advanced clinical knowledge all contribute to better outcomes for patients and families.
Succession planning is also part of Little Haven’s view of the future. It is acknowledged that the CEO will one day no longer be in the role, and the Board is cognizant of this, particularly considering her substantial role in public promotion of the Little Haven model of care and funding opportunities.
It was acknowledged that funding remains an ongoing challenge for Little Haven’s model of care. Although the financial position of the organisation is strong, it is also highly dependent upon continued government funding and local fundraising.
3.9 Carer satisfaction surveys
3.9.1 Structure of the Carer Survey
For the purpose of this report, a contemporary 24-month sample of Carer Evaluation Survey data was drawn from the larger dataset that commenced in 2014. This comprised of survey data collected between January 2021 and December 2022.
The anonymous survey is comprised of 10 multiple choice items, three items that utilise a five-point response scale, and two open response items. Two of the multiple-choice items also provided an option to expand in the event of a ‘dissatisfaction’ response. Carers are invited to provide information regarding:
- The source of their referral to Little Haven.
- Their awareness and utilisation of key services within the Little Haven model of care.
Their reflective satisfaction regarding different aspects of Little Haven’s services and approach. A copy of the survey can be seen in Appendix 5.
3.9.2 Survey sample
Deidentified Carer Survey data were made available to the research team. For this report, a contemporary 24-month sample of Carer Evaluation Survey data was drawn from the larger dataset, that commenced in 2014. This comprised of survey data collected between January 2021 and December 2022.
Within this identified period, a total of 116 carers submitted completed carer evaluation surveys to Little Haven. The distribution of returned surveys across each quarter, along with quarterly survey response rates can be seen in Table . The highest response rate (22 persons) occurred in Quarter Four of the 2021-2022 financial year (April-June 2022).
Table 14: Responses and response rates across time
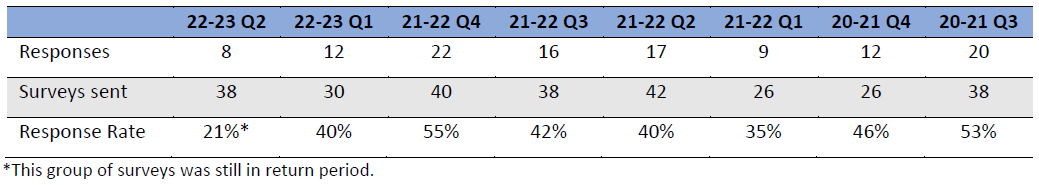
Commencing February 2021, minor modifications were made to the Carer Satisfaction Survey. A response category ‘friend’ was dropped as an identified referral source. A new category ‘respite volunteers’ was added to the care services items listed in the survey. Scale items inquiring in relation to the perceived usefulness of experienced complementary therapies, and perceived benefit of engaging with respite volunteers, were also added at this time. These differences impacted the responses of nine respondents within the dataset, and changed the available sample size from 116 to 107 for four items within the survey. These impacts are notified as they present within the data reporting below.
Responses to the multiple choice and scale items were collated and reported descriptively. Qualitative responses to the two open-ended items were collated, coded and explored for emergent themes.
3.9.3 Results
3.9.3.1 Referral Source
Forty-eight (41%) of the respondents indicated that they had been referred to Little Haven by a doctor. Twenty-nine (25%) reported referral via an hospital, and an additional 12 (10%) indicated self-referral. An additional 17 (15%) of participants attributed referral to ‘Other’. The item response structure did not provide for further detail in relation to an ‘Other’ response. Three of the nine respondents who completed the survey in January 2021 (pre-modification), indicated that they had been referred to Little Haven by friends. Seven respondents elected not to answer this item.
3.9.3.2 Service Satisfaction
Carer evaluations of service factors were uniformly highly positive (see Table 15). Between 95 and 100% of respondents indicated satisfaction with each of the measured service factors. A slightly lower 103 (92%) of respondents reported maximum satisfaction in relation to support of spiritual/emotional needs (scoring at 5 out of 5). Two of the 100 respondents (2%) reported that they did not feel supported in this regard (scoring at 1 on the 5-point scale).
Table 15: Carer evaluation of service factors
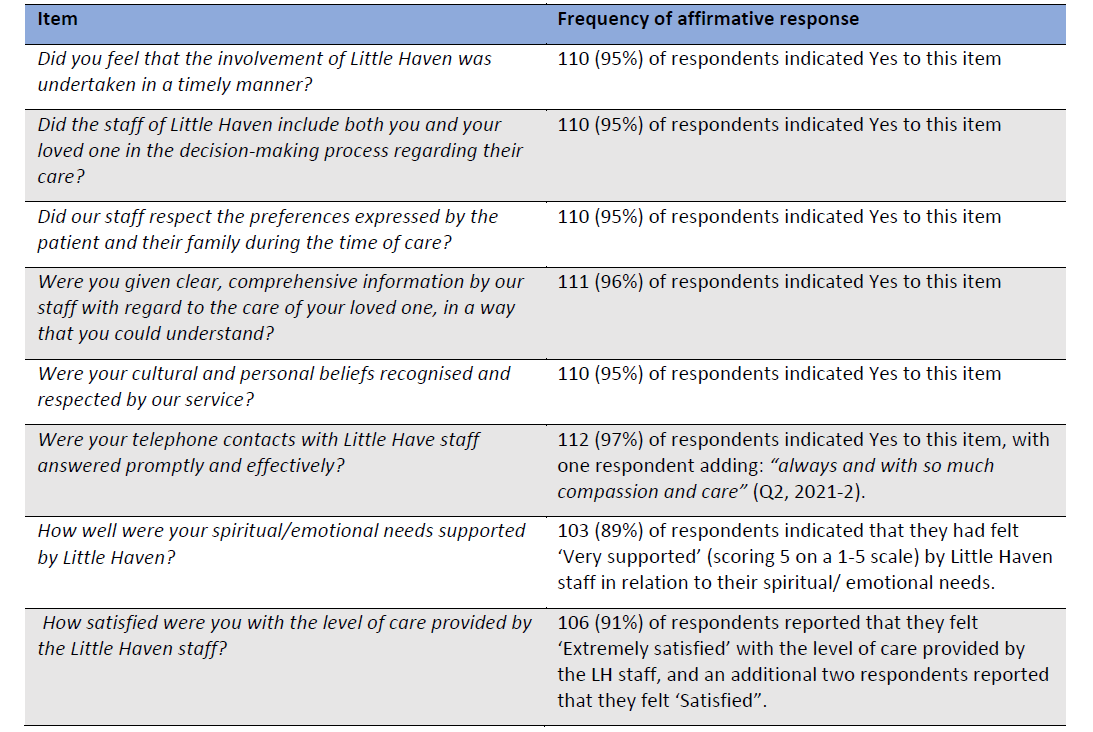
3.9.3.3 Awareness of service availability
The Carer Survey inquired regarding respondents’ awareness of five service elements:
- Nursing staff on-call 24-hours per day.
- Free loan of equipment.
- Bereavement support.
- Complementary therapies.
- Respite volunteers. *
Respondents’ awareness of the first three services was high, with 111 (96%) of respondents recognising the availability of nurse contact 24-hours per day; and 110 (95%) of respondents recognising the availability of free loan of health support equipment. A total 111 (96%) of respondents indicated that they were aware of the available bereavement support service. Awareness was slightly lower though still high in relation to the availability of complementary therapies (n=101; 87%). Awareness of the respite volunteer service was substantively lower (n=72; 66%).
*This latter item was omitted from the prior version of the survey, completed by nine participants within the present sample. Thus the sample size for frequencies related to the respite volunteers service elements has been set at n=107. The sample size for the item inquiring in relation to perceived usefulness of the complementary therapies has also been set at n=107, as this too also added to the survey after January 2021.
3.9.3.4 Respondent engagement with identified services
Responses from carers reflected a strong general uptake of three primary services: utilisation of the 24 hour on-call nursing capability 95 (82%); equipment loan 100 (86%); and bereavement support services (n=63; 54%). Uptake of available complementary therapies was lower, with 40 participants (35%) indicating that they engaged with these services, and 46 participants (40%) reporting that they had not.
Interestingly, this item was paired with a later related item querying perceived usefulness of the complementary therapies. A total 54 participants (47%) responded to this latter item. This could either suggest that uptake of these services was actually higher than indicated in the prior item, or possibly, that a small number of respondents may have thought that this item related to all of the available services as a group. Of the 54 respondents, 41 indicated that they found their engagement with complementary therapies to be very useful (scoring 5 on a 5-point utility scale), and an additional nine respondents scored the therapies as useful (4 on the 5-point utility scale). These outcomes appear to indicate that while uptake of the complementary therapies was lower, those who did engage with these services, found them to be useful.
Uptake of the respite volunteer service was comparatively very low across the provided services at 18 (n=109; 17%) of respondents. This item was also paired with a later related item querying perceived benefit of utilising the respite service. Notably, 46 respondents provided a score for this latter item, with potential explanations aligned with observations of the similar item relating to perceived utility of the complementary therapies. Forty-four of the 46 responses score a 5/5 for perceived benefit.
3.9.3.5 Aspects that need improvement
Midway through the survey, respondents were invited to identify any aspects of the service that needed improvement. There were ten responses to this item. Eight of the responses consisted of acknowledgements of the excellence of the service: ‘Absolutely marvellous’ (Q2 21-2); ‘All staff were amazing’ (Q3 21-2); ‘Beautiful treatment from all of the staff – nurses’ (Q1 22-3); and ‘None – everything was excellent’ (Q2 22-3).
One respondent suggested ‘Perhaps more advice and support on what to give {name of patient} to eat to help me with his meals’ (Q2 22-3). One respondent mentioned within the further comment item (Question 7. Aspects of our service that you feel need improving): ‘Pushing their beliefs’, then adding ‘Thank you all for your kind support’ (Q3 21-2).
3.9.3.6 Additional Comments
At the close of the survey, respondents were provided with an invitation to add further comment. There were 83 responses to this item distributed across time, shown in Table 16.
Table 16: Distribution of responses to the open comment item across time

Emergent themes: carers
The bulk of comments were focused on the expression of thanks, acknowledgement of the support received as carer, the pivotal contribution of Little Haven in enabling family members to die at home, quality of the service, and the experienced relational qualities of staff engagement with family and carers. Specific themes, frequencies of categories of comment, and representative quotes are presented below (see Table ).
Table 3: Emergent themes within Additional Comments content
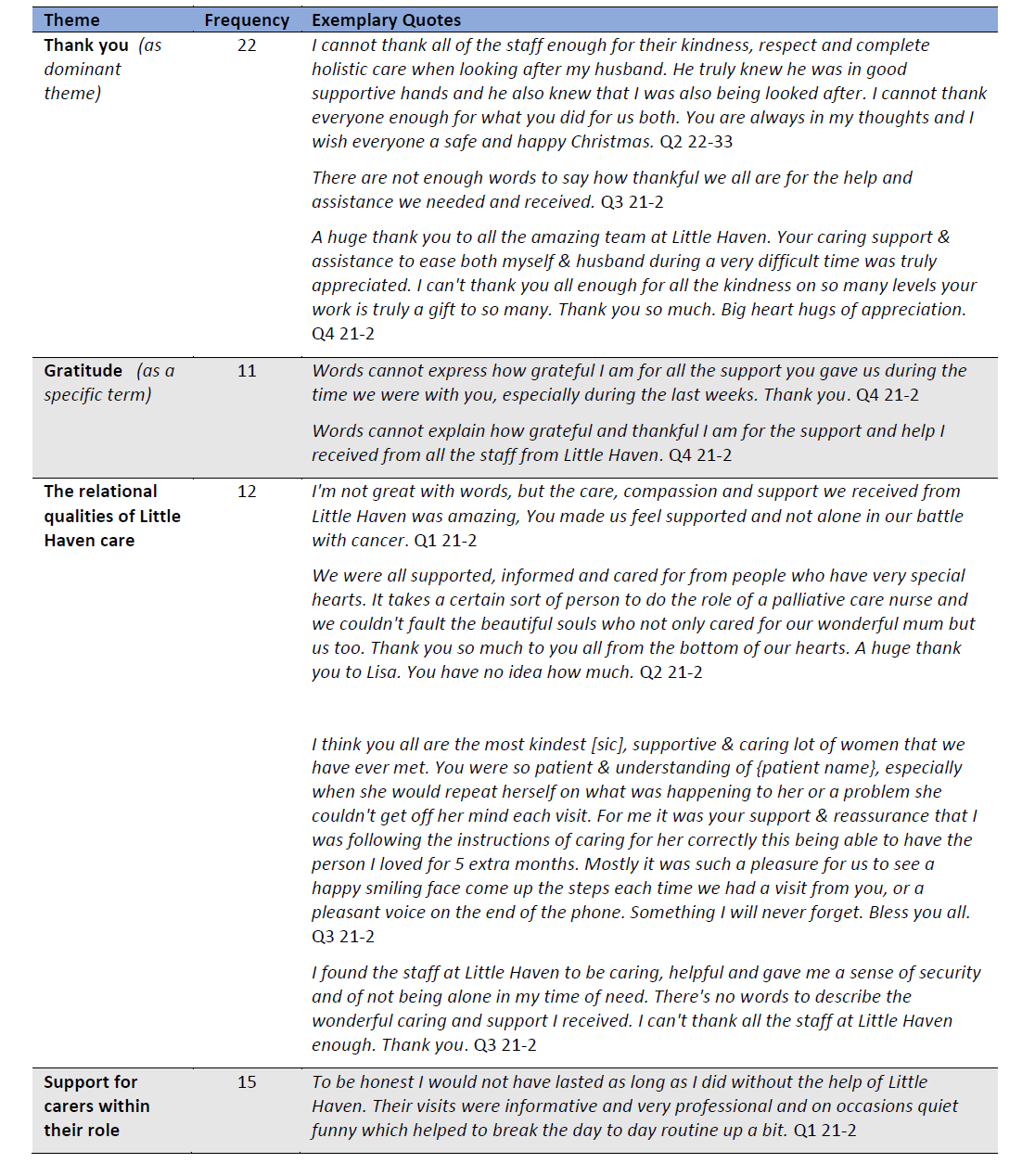


Several of the responses integrated different themes within a single statement. To provide insight in relation to the integrative nature of the responses, exemplars are included below:
Words cannot express how grateful myself, my daughter & my beautiful Dad … were for your incredible support daily. It was 7 weeks that could have been unbearable but your support, knowledge, compassion & fast responses allowed us to have quality time together before, as Dad put it, “he headed off on his next adventure” peacefully & in no pain thanks to the unbelievable support on the last day. And your bereavement counselling &follow ups has helped in more ways than you will ever know. The time with my Dad was a privilege and a blessing – in no small way because of you. Q4 21-2
We can’t express enough the gratitude we have. The whole experience of caring for both of my parents at home with the care, understanding and professional approach to them and us as a family was wonderful. I feel privileged to have been able to have them stay at home but without your wonderful organisation and just amazing staff it would not have been possible. Q2 21-2
One respondent acknowledged the practice of LH staff of reaching out and offering services, even though they had elected not to engage with them:
I’ve been offered numerous times, bereavement support, complementary support, respite volunteers but have never taken up the offer to date. Thank you for your understanding. Q4 21-2
Finally, even respondents who had only a brief involvement with Little Haven felt moved to add comment:
Being a short time between using and departing of husband I really had not much time to comprehend the situation, but was pleased. Q4 21-2
My husband came home from Eden Hospital just 3 days before he died. Each day one of your ladies spent a morning helping us wash and care for him. They were wonderful. My family and I cannot praise them highly enough. I cannot answer all the questions as they are not applicable. Without the help of the Little Haven ladies my husband would not have been so well cared for by us – his family. Q2 21-2.
Expressions of concern
Only two of the 83 comments expressed concern. The first queried the arrangement of meeting spaces that required vaccination: ‘Disappointed venue for later meeting other people had to have all vaxes.’ (Q4 21-2) The second related to a perceived delay in referral, relating more to referral source than the Little Haven service itself:
It was probably because of covid, but I think we were not referred early enough. I think we should have had a referral at least a week earlier. As it was, my mother passed away very peacefully. And I felt well supported. Thank you. Q4 21-2
3.9.4 Discussion
Evaluation data collected via the Carer Satisfaction Survey provides clear indication that carers of patients are satisfied with service provision, and that key objectives of Little Haven in relation to timeliness, collaboration, and respect are experienced as well met. The majority of carers are aware of the suite of Little Haven services and engage strongly with the 24-hour nursing service, no-cost equipment loans, and the bereavement support arms of the service in particular. Complementary health services are utilised to a lesser degree, though are rated highly by those that use them. Qualitative input from respondents describes both the tremendous significance to, and perceived benefit of, Little Haven services to carers of individuals who are dying.
Much lower rates of engagement are reported in relation to the respite volunteer service, highlighting a potential area for further investigation.
3.9.4.1 Service satisfaction
Over 90% of the respondents indicated that they were ‘Extremely Satisfied’ with Little Haven services. Ninety-five percent or more of respondents expressed their belief (in each case) that:
- involvement with Little Haven was timely.
- staff were highly inclusive of patients and carers in care decision-making.
- the preferences of patients and carers were respected.
- pertinent information was communicated clearly, comprehensively and accessibly.
- personal and cultural beliefs were appropriately recognised.
Just under 90% of respondents indicated that they had felt very supported by Little Haven staff in relation to their spiritual and/or emotional needs. Ninety-seven percent of respondents identified that telephone contact was responded to promptly and appropriately.
3.9.4.2 Service awareness
There was high level awareness among carers in relation to four of the core service arms – at over 95% for 24-hour nursing availability, no-cost equipment loans, and the bereavement support services, and at 87% for the available (no cost) complementary therapies. These outcomes suggest that current modes of communication to carers in relation to these services is effective.
As anticipated, service engagement was highest for the 24-hour nursing service and equipment loan services, at 82% and 86% respectively. Just over half of the respondents had utilised the bereavement support services, and just over a third had engaged with complementary therapies and found the engagement with these therapies to be very useful.
Awareness in relation to the respite volunteer service was substantively lower than that for the other services at 66% and may indicate a potential point of future emphasis in service promotion, with uptake within the surveyed group at 17%. Given that carer support was identified as a highly valued element of Little Haven by carers, this low uptake is of interest. While awareness of the service was lower than that for other services, engagement was much lower. Interestingly, those that did elect to utilise the service felt it to be highly beneficial. As such, it appears that the respite volunteer service is a potentially beneficial support strategy that is at present underutilised to a degree greater than explained by lack of awareness of its availability. Further discussion with Little Haven service users may provide insight in relation to potential obstacles/barriers that may be inhibiting uptake of this service element.
3.9.4.3 The Additional Comments item
Almost three-quarters of the survey respondents utilised the provided ‘Additional Comments’ invitation, to add a personal expression to their completed surveys. The provided comments were overwhelmingly positive, with respondents expressing and detailing their appreciation for the Little Haven service and team.
Emergent themes highlighted several points of specific importance to the carers. The relational qualities of staff engagement with carers and patients were emphasised, with compassion, kindness, helpfulness and support presenting as key descriptors of carer experience. The pivotal contribution of Little Haven in enabling patients to die at home was acknowledged as a forefront and deeply appreciated offering of the service. Little Haven’s attention to the needs of carers was also highlighted as a key point of appreciation, with several carers describing this support as a core sustaining resource during the later stages of care.
3.9.5 Summary
In the words of one respondent, ‘Keep doing what you have always been doing’ (Q2 22-3). Outcomes of the carer survey firmly and clearly establish that among carers, there is a shared perception that Little Haven services comprehensively meet the needs of both patients and themselves. Responses further indicate a high degree of service awareness and satisfaction, and a strong or sound uptake of most of the offered service initiatives.
At present there is room for growth in terms of uptake of the respite volunteer service. Further exploration of possible barriers to engagement may inform initiatives to promote carer and patient engagement with this respite offering.
4. Discussion
This section synthesises the multiple sources of data reported in Section 3 to address two evaluation aims:
- The extent to which Little Haven’s model of care meets their goals for service provision and community engagement and provide efficiencies in the utilisation of health care services, through the examination of organisational structures, processes and outcomes, including economic costs and benefits.
- A comparison of Little Haven’s model of care to like services to identify those structures, processes and outcomes not found elsewhere, to determine its replicability in other settings.
4.1 Models of community-based palliative care
Palliative care within the home can improve pain and symptom control, increase quality of life, improve family bereavement, reduce the need for hospital-based care and provide cost-savings for governments. Further, many palliated individuals wish to die in their own homes as it can offer a source of physical and psychological comfort, aligning with the concept of a ‘good death’ (Haydon et al., 2021, p.625).
This quote from the published literature captures the intent of community-based palliative care, and it is clear from this evaluation that Little Haven fulfils these components. Its model of care contains all the key organisational elements identified in the national and international palliative care sectors described in Section 2.2.4 (see Figure 2):
- Accessibility of service.
- Early intervention.
- Patient- and family-centred approach.
- Specialist staff.
- Holistic care.
- Community involvement.
- Free to low-cost services.
Further, the values that underpin Little Haven’s implementation of their model are clearly evident in the clinical and non-clinical practices of staff, volunteers and the Board. This is especially apparent in the organisation’s engagement with the communities in Gympie and surrounding districts, and key stakeholders in clinical practice.
Identifying how these components are configured and operationalised in the Little Haven model of care was essential to ascertain the extent to which the model meets the goals for service provision and community engagement and provides efficiencies in the utilisation of health care services.
4.2 Structures
The configuration of organisational elements* in the Little Haven model of care are clearly ordered around its stated goals to provide the delivery of the highest quality of care, support and education for those experiencing or anticipating serious illness and loss in the Gympie and surrounding region.** The literature identified that access to palliative care services is mainly through provision of home visits and after-hours care, 24-hour phone support, provision of care on demand, and operating day care centres (Kilonzo et al., 2015) and comparisons with Little Haven’s model are of interest. These structural elements of their model are explored in more detail here.
* After Donabedian (1980, 2003)
** https://littlehaven.org.au/about/
4.2.1 Built environment
The current co-location of Little Haven’s offices with Gympie Hospital is viewed as enabling close liaison between the Hospital and the Service to the benefit of both teams and patients:
I think being on site is an advantage. Because they also share the building, just by chance with the cancer care unit, [and] the renal care clinic. So, if there’s a patient that’s under Little Haven, and they’re attending the palliative care clinic and give consent, the nurses can be a part of that review. I think it’s a positive for the patient … it’s reassuring for the patient as well. And it just creates really good collaboration amongst the teams. SK2
However, the current plans to build an inpatient hospice may require new strategies to ensure these strong links remain. The establishment of an inpatient hospice was part of the original plan of Little Haven’s founder, Mrs Phyllis Little, which was altered in response to a clearer community need for home-based care (King, 2022). In any case, the establishment of an inpatient hospice will enable Little Haven to provide continuity of care for patients who elect not to die at home or do not have sufficient support to do so:
…that’s definitely something that we’ve outlined as part of our strategy going forward. And we’ve started fundraising for it. There’s a lot of interest in town. I think too, with raising funds in the community, of course, people like something bricks and mortar that they can, that they can actually see that that’s where their money’s gone. I think that there’s certainly an appetite for it. And there’s, obviously, we’ve seen in the last few years, that there’s now an appetite for it with Federal funding, so it’s a good time for us to be to going into that as well. SK4
Notably, there is recognised community interest and investment in this planned expansion of the Little Haven model of care. Indeed, the community’s appreciation that local fundraising remains in the community and is not exported to a centralised administration is in play here. Such an expansion of the service model will of course impact upon all funding requirements, the recruitment and retention of workforce and volunteers, liaison with existing hospital services and GPs, and consequently will require some operational changes.
How this will interact with the perception identified by Little Haven staff that other healthcare providers assume that Little Haven is already a hospice remains to be seen:
We’re often assumed were hospice, right? So people often ring us and go, okay, so [name] needs to come in to you now. What do you mean? And then you could have that conversation. We can look after them at home and work out their plan and everything. But there is that assumption from new practitioners coming to the area that that’s what they assumed that we are. SF9
In this evaluation, there are clearly a range of perceptions of how well-known Little Haven is, and an opportunity presents itself once the building is completed and the facility opened to undertake a refreshed awareness-raising campaign of the expanded model of care.
4.2.2 Governance
As a not-for-profit charity receiving funding from Queensland Health and financial support through fundraising from the local community, Little Haven’s governance is critical to its operation. Its nine-member Board oversees the governance of the organisation. Little Haven’s model of care was compared to a family business model:
The way Little Haven works … it’s quite similar to a family business where we have to be in control of … the things that we want to work towards, and our future. And that was always a risk to with increasing our government funding. But we’ve been able to sort of keep that family business model. And in family business, we’re always taught that governance is so important, and succession governance, understanding that we are the stewards of for future generations. So, the way those two models aligned, I quite enjoy that. SK4
This is a notable structural component of the model of care as it enables local – rather than centralised – governance of the service, which is highly regarded by multiple participants as essential to the model. Ensuring this local governance is retained whilst obtaining government funding is a feature of this structural element.
Although the Board’s work was not commonly commented on by other participants in the evaluation, the volunteers saw the Board as entrusted with responsibility for pursuit of funding to ensure the ongoing longevity of Little Haven and construction of the hospice building. Many of these volunteers considered themselves as best able to offer support the service at the community coalface through fundraising activities, whilst acknowledging that they are represented on the Board by one of their number.
4.2.3 Programs
Community-based services providing specialist palliative care are better suited than generalist services to address the needs of home-dwelling patients with life-limiting illnesses (Gomes et al., 2013b). The specialist knowledge and compassionate care offered by Little Haven services are key features of how its program of care is structured. This key stakeholder put it this way:
The standout thing is that not only do they have a good skill set, but they are very patient-focused, and they will do what it takes to try to deliver the care that the patient wants in the patient’s preferred place of death, as best they can. SK1
In community-based models, the provision of palliative care goes beyond addressing the physical health of the patient (through medical, nursing, and allied health services), to embrace spiritual and psychosocial support, bereavement counselling and other services, such as advance care planning and complementary therapies, in addition to with noted benefits to patients (Gomes et al., 2013b). This Little Haven staff member clearly articulates this view:
It is a holistic approach to terminal diagnosis that comes to a family. It is not necessarily about patients. In the essence of it, it’s about the people that support somebody with that prognosis …so I think that is where we really shine. We make it quite clear in admission that we’re here for all of you. SF10
This requires the presence of a comprehensive, coordinated and cohesive multidisciplinary team and the nature of the Little Haven team was explored in great depth in this evaluation, particular by staff and volunteers, whose perspectives reflected a model of care that is person-centred, responsive and flexible; these are commented on below in discussing process elements of the model of care.
4.2.3.1 The multidisciplinary team
As structural component of the model of care, the internal multidisciplinary team is comprised of nurses of differing levels, allied health including social work and bereavement support personnel, and volunteers including complementary therapists. As noted in the literature review in Section 3.1.5, in regional settings, resourcing can limit the range of clinical disciplines available, and external partnerships are essential to delivery of comprehensive services. Externally, strong interdisciplinary and interagency links are found with Gympie Hospital and the wider SCHHS, GPs and generalist home-based care providers.
The structures of the multidisciplinary team are explored here drawing on multiple participant perspectives – further exploration of process elements is addressed later.
Nurses
The organisational prioritising of holistic, person-centred care including care for carers are key elements of the nurses’ role in Little Haven. Specifically, early admission, rapid response, flexible delivery, the inclusion of volunteers and the Nurse Mentor Program were structural elements that were identified by nurses as key strengths of the model of care. Although organisational structures can be unyielding, it was noted that at Little Haven, they still permit the flexible focus upon individual needs:
It’s truly client centred care … it’s what each client needs. We might have a bit of a framework for our care, but we also tailor it to each client and each family based on their needs…The focus is always the client’s needs. SF3
The capacity of the Little Haven model to allow for flexibility of approach with patients and families was identified as a hallmark feature of this model:
I’ve worked for other community nursing organisations, and they’re very strict with like, how long we get with each person, whereas I love the Little Haven model, which is you’d have a visit. And if that visits 15-20 minutes, or if that visit’s two hours, it’s whatever that family needed that day at that time. And, and I love the flexibility of that and not feeling the pressure of when they got an hour here, I gotta go. If they need that time, they get that time. SF3
The 24-hour, 7-days/week availability of Little Haven nurses is a structural feature acknowledge by other external multidisciplinary team members, such as this GP:
Being a point of contact for the family, a local point of contact … as opposed to some visiting service. So that sort of thing might be some of the bigger picture stuff, but also just some of the nuts and bolts of getting syringe drivers, the medications, being that link in with the primary care doctor, who the primary provider is for that patient, just in terms of getting scripts. And over the weekend as well. SK5
Other service providers who seek Little Haven’s input into the care of their clients provide an opportunity to advocate for a preferred model of care:
…it’s good that organisations come to us and say, could you just talk our workers through what you’d expect of their care in the home, and we’re able to say we would like some consistency with the carer in going into the home, we want, don’t want a different person going in every day. I think that helps upskilling them as an organisation. So sometimes our nurses can pair with them to actually teach them, how to better give appropriate care for someone who’s going into the palliative stage where it really matters how they are handled. SF1
Once other services are involved, Little Haven nurses can provide context specific training of other agency providers supporting improved and more appropriate care on the part of the providers, and a better experience of care for patients and family members. The published literature has suggested that the highly regulated Nurse Practitioner (NP) role, described in Section 3.1.5.2 above, may assist community-based palliative care services to deliver care where a depleted workforce presents systemic challenges. This proposition treated with caution by one GP, who reported that although they have, and do still work with NPs in other settings, it is not clear that such a role would not risk the recognised qualities of the Little Haven model. Another GP was unequivocal in their opposition to a Nurse Practitioner, seeing instead that, between the GP and the Little Haven nurses, the care needs are addressed already.
Bereavement support
The Little Haven model of care provides a comprehensive and expert bereavement support service. In most palliative care services, bereavement support is either absent, or focussed primarily upon support during the caregiving period. At Little Haven, support is available and ongoing to carers beyond the death of the patient. This initiative within the Little Haven Palliative Care model is offered to each family, entailing the following elements:
The day following the death of a patient, a member of the clinical nursing team will visit the family to provide bereavement support. There is also a pack that is sent out in the mail that has a little booklet that just talks about grief. It lets them know that a social worker will be in contact in the next two weeks, and that there are some complementary therapies available to them as well as part of the bereavement support program. Within the two weeks, one of our social workers will reach out over the phone. They will talk to the person and assess where they are at, and what might be of assistance for them in terms of bereavement support…. The model tries to address that everybody grieves differently, everyone’s circumstances are different. Not everyone necessarily needs six face-to-face sessions. But, you know, just trying to identify with that person collaboratively about what is going to be useful at this time. SF2
This further demonstrates the person-centred nature of the model, avoiding a ‘one size fits all’ approach to bereavement support.
Volunteering
Little Haven is well-known for its team of community volunteers. Many volunteers were motivated to join the team by personal experiences as family members being cared for by Little Haven, sometimes from decades ago. Their dedication to Little Haven is clear, and although there are challenges facing volunteerism, it is regarded as an essential structural component of Little Haven’s model.
Volunteers can be involved in a range of support roles including the Little Haven offices, within the community in activities related to the promotion of, or fundraising for, Little Haven, and within the homes of patients, providing respite for carers. These roles are highly valued, not just by the volunteers themselves, but by other team members too; their presence, in fact, is essential to Little Haven’s model of care:
Volunteering is such a big part of our community … as well, because you know, a lot of services are moved away from volunteering, because it’s difficult, then managing volunteers is difficult, but what they bring to us is so important. One is a social support system for some of our bereaved who, come back into the into the model as volunteers. They have their own social support. Yeah, and it all keeps us true to our mission. [the volunteers] are still doing things to prop our service up bringing their hands to work. I think volunteers get a lot out of what at what they do to I believe they’ve got their own social network development. It is so important to engage [with the volunteers]. We would never afford to do what we do without them. SF1
As noted, managing volunteers can be challenging, and increasingly subject to external governance requirements. This presents a challenge for some volunteers, who find the regulation of their volunteering unwelcome:
I think volunteering also has a lot of problems with governance. There’s lots of restrictions. There’s lots of government restrictions that get in the way. Lots of them, including insurance. You know, you can’t do this, you can’t do that. VL11
Although there is a respite volunteer service, awareness of the respite service was lower (at 17%) than that for other services, engagement was much lower, highlighting a potential area for further investigation. Given that carer support is a highly valued element of Little Haven by carers, this low uptake is of interest. Little Haven encourages family involvement, utilisation of package care service and coordination of family and friend networks before offering respite volunteer support. Some carers felt that it should be made available to those whose need they assumed was greater than theirs. Notably, those that did elect to utilise the service felt it to be highly beneficial.
General Practitioners
The General Practitioners interviewed for this evaluation were clear in their support for the organisational components of Little Haven’s model of care, and the quality of the care provided by its clinical staff. All four GP stakeholders described Little Haven’s involvement as complementary to their long-term, primary care of pre-existing patients who had become palliative:
I’m a GP that does, you know, from birth to death and you know I do all of it, and Little Haven allows me to really comfortably do the death part, because it is quite time consuming, and there’s an after-hours component involved. Because GP is really poorly remunerated. SK5
This relationship between GPs and Little Haven is not simply transactional, but an established understanding of clinical expertise and appropriate communication within a structured interface:
And I think, you know, the GPs take the call from a Little Haven first, you know, whereas they don’t from other places that might call because they know Little Haven nurses are calling for no reason. They’re not going to waste their time, they’re going to know that patients, they’re going to give an accurate handover. SF2
Notably, although this perception was evident in GP interviews, it was also observed that some GPs’ participation in the provision of palliative care through Little Haven was not always as reliable, with some noted to have poor understanding of Little Haven’s service model. Limited or incorrect knowledge were reported in some cases by carers, while being very comprehensive in others. There was a potential geographical link identified within this theme, with GPs within the Gympie area appearing to be more aware of Little Haven, how the organisation works and admission procedures than GPs outside of the Gympie area. Notably, Little Haven participates in both raising awareness amongst GPs of palliative care and supporting training of new GPs through hosting students:
We’ve had medical students from James Cook University come down, and I’ve been impressed enough with Little Haven, and been keen for them (the students) to understand that in home care is but possible and available, and I think you know an option for things, so Little Haven has been kind enough to allow the students to be attached with them for a day here and there, and the feedback has been very, very positive, indeed. SK6
In a broader context where there are challenges to the sustainability of the primary care workforce in the regions, including Gympie and surrounds, Little Haven’s efforts in promoting these partnerships remain critical.
4.2.3.2 Care coordination
The program components rely upon care coordination both within Little Haven and between it and collaborating services. Although there were many aspects of healthcare to navigate, the role undertaken by Little Haven in coordination of care is strongly linked to patients remaining at home for as long as possible or desired. This collaboration with other services has long been considered essential to the program of care and relies significantly upon the establishment and sustainment of formalised partnerships:
The formalisation of partnerships across the network provides a platform to explore creative alternatives for better continuity and coordination of local palliative delivery, including initiatives such as: co-funding of service delivery; utilising common palliative care clinical indicators and assessment and management tools; standardised data collection, developing a common language; and the use of end-of-life care pathways by generalist health care providers in all care settings (Phillips et al 2006, p.377).
These services are important to patient care, and as such are important to foster. In turn, the fostering of such relationships is facilitated by the excellence of the model of care that Little Haven provides.
4.2.4 Staff support
The Monthly Meeting of staff to review the preceding deaths is a structural component of the model congruent with the values of Little Haven to support its staff’s professional development and personal resilience. It addresses case specific communications, tasks, updates and planning; importantly, it offers a forum for staff to offer their personal reflections and check in on their reactions to these experiences. For some staff members, this was an unprecedented experience:
I’ve never worked in another line of nursing where you don’t have to just suck it up. But that is not what happens. Everybody has an understanding of the needs we have that support each other. I think that’s what is so incredibly different about it. SF11
The presence of this regular meeting in the structure of the model reflects a longstanding acknowledgement of the challenging nature of palliative care provision and practice, with the subsequent need for team building and resilience.
For volunteers, being treated as equal members of the team was greatly valued. The support of the CEO was praised for being at the coalface and supportive to the volunteers’ work:
If it’s a function, she’s in there getting her hands dirty as well. She just doesn’t say “Do this. Do that.” She’s helping. VL12
There was a sense of being cared for by the organisation when volunteers were themselves sick:
… there’s been times when everybody’s probably had something medically wrong with them, but Little Haven actually will ring you and say, “How are you going? Is there anything we can do to help?” VL4
4.2.5 Financial systems
Little Haven’s goal for growth is set at 9-10% per year, and this ambitious target brings with it specific challenges to service delivery in community settings:
That means keeping a nursing staff and also, vehicles on the road and kilometres driven. We cover a vast area. So, the travelling that nurses do … if there was some way that we could limit travelling, you know whether we have nurses that that work in certain areas and service certain areas, but that is logistically, that’s probably the hardest thing. SK4
Little Haven is in a strong financial position however its reliance upon Government funding for its continued operation represents a risk for the organisation. Previous increases in government funding have addressed a wages shortfall, rather than underpinning growth:
We’ve been very lucky, especially with the State funding, it has been adequate in that it has allowed us to probably pay the nurses what they should be paid, right? Whereas in the past, there was always a funding gap there. So, what we’ve got at the moment, it allows us to continue operating as it is. Yeah, if you were to lose that funding you would be, especially as Little Haven has grown strongly. Over the last decade, it would be very hard to continue what we’re doing without that funding. SK3
Applying a conservative cost estimate based on a reduction of QH health service use (hospitalisations and emergency admissions), cost savings are estimated to range from $730,000 – $980,000 per year for the cohort of Little Haven clients (n=160) in the last year of life alone. Average costs per person per year of providing palliative care services were much lower for Little Haven clients ($6,194) compared to the national average for in-home palliative care services ($8,000) or hospital-based palliative care services ($15,373). Furthermore, contracted deliverables to the state funding body QH in terms of hours of occasions of service provided were exceeded by far (250%) with average cost of only $33/hour instead of an anticipated/funded $166/hour.
From a business perspective, Little Haven is a viable service which consistently resulted in a higher total income compared to total expenses over the observed period of service. The main driver of income is funding, in particular from QH and the main driver of expenses are staff-related costs which is expected from a service provider. The economic evaluation demonstrates that Little Haven is a highly viable community-based service and provides excellent value for money from a health service perspective.
4.3 Processes
The operationalisation of structures into processes* that aim to achieve the organisational goals of the Little Haven model of care is where it most clearly demonstrates excellence. These process elements are explored here.
* After Donabedian (1980, 2003)
4.3.1 Access and inclusiveness
Patients are accepted at referral regardless of their diagnosis, prognosis, or personal circumstances. A social health approach drives the inclusion of all those with identified need within the geographical footprint of the service:
… it’s zero discrimination. It doesn’t matter if people live alone or have carers, it doesn’t matter where people live, as long as it’s in a geographical zone, it doesn’t matter if it’s a shanty, to a mansion. And everybody’s treated exactly the same. And that’s because we don’t have any means testing for that. Our services are free to every single person, there’s no limitations to who we can care for. And everybody gets the same care and access to care. SF3
This flexible person-centred care applies equally to those who might not all be experiencing high needs, both at admission and during the period of care:
We take patients from the minute they ask for us. Nobody is turned away. Generally, a palliative diagnosis is 90 days, the three months thing, and a lot of people don’t recognise palliative care as being as extensive as we do. Our run sheets do actually have stable people on them, and we are doing a lot of holistic caring, really preparing these people spiritually and emotionally. So with these people … populating our patient lists, it does make for a more flexible patient list, because not everyone on the list is vitally scripted for a visit today. SF10.
When arranging care for an existing patient of another service provider, the constraints to access can become quite evident, and it is here that Little Haven demonstrates a unique capacity:
…and that seems to be very different to a lot of organisations we deal with. You ring them up and before you can start talking it’s like, “Oh, we don’t do this, we don’t do that.” So we try always … well, what can we do to help? We might not be the main provider for them, but at least we can triage their concerns and get them on the right track. I think that’s probably the difference. SF1
This GP reported a simple – and welcome – referral process, which had been challenging in other services:
I had somebody that I felt might benefit from our view by Little Haven. I called them up, and they have been very responsive, which is terrific in any service, you know a lot of the services we have … can be difficult to deal with, and I found that that it’s (Little Haven) been exactly the antithesis of that. SK6
4.3.2 Early provision of care
As noted in the review of literature, the provision of care early in the disease trajectory is linked to improved end of life outcomes, including alleviation of symptom burden (Baumann et al., 2015), reduced pain (Mularski et al., 2009), and improved satisfaction with care (Gade et al., 2008). Further, it may provide a reduction in the avoidable transfer of home-dwelling patients to hospital during palliative care, which in turn can result in better patient and carer experiences, and efficiencies in the cost of health care (Youens & Moorin, 2017). As this staff member noted, early provision of care enables rapport and continuity of care:
Meeting early means that you can build that rapport…you get to know them, and they trust you. And you’re able to go through the whole trajectory with them, which is really special. SF6
However, as a process element, early admission is an uncommon practice in palliative care primarily due to funding constraints, with admission limited to those with a likely prognosis of three to six months. This responsiveness of Little Haven to referrals, which were attended to promptly and early in the illness trajectory is highly regarded by patients, carers and other healthcare providers enabling ‘a flexible service which allowed carers to maintain “normal” family life activities’ (Poulos et al, 2018, p.276):
… we won’t wait till people have a crisis of three months. So that early intervention, I think we’re well known for the fact that people can walk from the hospital where they get a diagnosis or prognosis of a life limiting event. And they’ll walk straight down to us at that moment. And that’s when they go on our books. it’s very much an open-door policy and that early intervention and not turning anyone away. SK4
However, when early intervention was not possible due to late referral, Little Haven are still able to respond, and in this example, it was possible due to their organisational practice of not turning anyone away. As this GP noted, restrictive models of care do not meet all patients’ needs for support:
I don’t think that there is any other service that offers that kind of support. A few years ago, I had a palliative patient who … was actually under one of the other organisations in town who were purporting to do palliative care in business hours, Monday to Friday. 4 o’clock, 4.30 rolled around, they were uncontactable, and it was a woman in her fifties who was going to die. Most of this stuff happens out of hours, and her family needed support so thankfully, Little Haven took her on, because the other service just couldn’t offer it, and they eventually admitted that they couldn’t offer that. SK5
However, referral late in the illness trajectory does not prevent the provision of excellent care; rapport with team members is reported to develop quickly, however consequences for grieving by bereaved carers is seen to be more complex, requiring the input of the bereavement support program. Addressing this specific need is viewed as an uncommon element in palliative care.
4.3.3 Responsiveness and flexibility
The capacity of a service to respond promptly to requests from patients and carers for advice and care is more likely to enable them to continue their daily routines, avoiding the need to present to hospital emergency department (Romanò et al., 2017) and reduced length of hospital stay if they are admitted (Trtchounian et al., 2017). This addresses a systemic problem in palliative care where unnecessary or avoidable admissions to hospital carry and enormous impost on both patients and health services. Little Haven’s support in this way promotes dignity, autonomy and independence and a sense of control in an otherwise uncontrollable circumstance.
The capacity of Little Haven staff to work very flexibly with patients and carers across time in in response to always-changing needs is identified as a strength of the model. Interestingly, this flexibility in practice has also been described by some staff as one of the significant challenges of the Little Haven approach, indicating that there is a weight of service associated with this factor, that is borne with an understanding of the benefit that it provides:
It is challenging having to work in a flexible environment all the time. My diary never looks like 8-8.30 and 8.30-9. There has to be flexibility built into that to allow for unexpected drop-ins. A gentleman dropped in today unexpectedly who I have been trying to get to come in since his wife died, and I was just able to attend to him immediately. SF2
4.3.4 Person-centred care
The processes underpinning person-centred care at Little Haven demonstrated congruence between their stated goals and values, with their organisational practices. Person- (or patient-) centred care is a central tenet of palliative care and a key process element in the operationalisation of services like Little Haven. The intention of person-centred care has been well-described in this article:
…considers people’s relational, creative, spiritual, cultural and social needs, as well as their physical and psychological needs. Strategies to connect on holistic levels can ensure that clinical care aligns with what is meaningful and important to patients and their families (Stanley & Daddo, 2022, p.10).
Being able to remain within the home to obtain answers to medical concerns was identified as a key aspect in maintaining a more ‘normal life’ for palliative patients and their carers and families. Prompt answers to concerns and being able to then self-administer treatments within the home, allowed patients and carers to continue their routines without the upheaval of extensive and prolonged hospital emergency department visits as a regular occurrence. These holistic approaches enable optimal independence and planning for anticipated care needs as health declines, and before crises occur, if possible. In addition to open and early access, responsiveness and flexibility, the provision of 24-hour/7 days per week care enables the service to place the patients’ and carers’ needs first; this provides responsiveness to identified needs, of course, but also ensures that health is monitored appropriately, with timely address of any chronic or arising health needs:
So many people talk about how that’s what got them through. They knew if something happened at two o’clock they could call. SF2
Patients themselves acknowledged that Little Haven’s input went beyond the clinical care, and that their quality of life was important to Little Haven too, regardless of the aspect of their lives it sits within; for example, staying on the farm (PT2), accessing medication (PT3), staying out of hospital (PT4) were all described as important by current patients. Continuity of support for bereaved carers is also highly valued, particularly for those whose partner had died and were experiencing disconnection living alone. In rural settings, this is particularly the case, however with Little Haven providing ongoing support, it can address this: If I am really upset…I can call and talk to anybody at Little Haven. For carers, too, this personalised service embraced their experiences …they make you feel like one of the family. BC2
4.3.1.1 Expert knowledge and skills
The advanced knowledge and skills in palliative care applied to practice by Little Haven clinicians was highly valued by other service providers:
I have great comfort in the fact that they will cover those questions that patients and their families will have after hours, that they will take care of those questions because they’re specialist. But the nurse is awesome in those last few weeks. SK5
This was also evident amongst local pharmacies:
A lot of pharmacists are also very responsive to us, if we ring up and say we are from Little Haven, they will put whatever we need ahead of the other scripts that they need to fill, because we have a timely response that we need to do. And, you know, some of our pharmacists are trying to carry more of the meds that we need in an instant. SF6
This expertise further enables trusted interchange between Little Haven clinicians and GPs. This is especially the case where the GP might not be fully aware of the patient and their circumstances (e.g., when they are on call for their practice) and the trust in the nurses’ clinical judgement enables appropriate care to go ahead.
You might get requests from patients you won’t necessarily be looking after, as you know, my own patients, have been palliated … where the practice will be ringing up saying “This is what we recommend” and you know, they’ve got such a wealth of experience that you’re happy prescribing a script or give a phone order. SK5
The capacity of Little Haven to provide home visits with a frequency responding to patient need and with a holistic and expert view was both clinically desirable and resource efficient for this GP, who could not conduct home visits further out of town:
Generally, the patients get home visits very frequently, and they have patients with have someone in their house who can actually observe how the patient is managing and how they’re coping in their difficulties. I found that much earlier than me in in my clinic room they can detect where things are going wrong, or the patient is not coping. SK8
4.3.1.2 Over and above
A very strong view was reported from multiple sources in this evaluation that Little Haven’s person-centred care goes ‘over and above’ or ‘above and beyond’ or even ‘way over the top’ (Q3 21-1) in its service provision. In this evaluation, patients and carers expressed surprise at how willingly Little Haven responded to their individual views and needs:
I was surprised that they are so good at what they do, that they just respect those that, you know, they get to know those people…they are not just a set of values they stick to, they step into your values…and they work within those values. BC5
The words of this volunteer, who had been a carer for her husband years earlier, perhaps capture this notion perfectly:
The nurses go, you know, they’re 24/7. When my husband was sick and couldn’t believe that the nurses were 24/7 and [name] was one of the nurses that looked after my husband. And “anytime, just pick up the phone just ring me” 24/7 Who gives you that? Some places don’t even give you that, it’s like, “Oh, go somewhere else.” VL12
In a very specific context, the major flood in February 2022, where much of the town of Gympie was inundated, saw striking example of this:
So, you know, even during the floods, so this happened last, during the floods, the nurse was on who was on call, her house was flooding at the at that exact time as well. And we had patients that we still had needed to care for, within this flooded region of Gympie. And I was on call and she was on call, you know, and she put the patients first, her needs she put second… SK1
4.3.5 Communication
Communication is, not surprisingly, a fundamental process within the Little Haven model of care, and is present between staff, patients and carers, volunteers, and other service providers. As noted in the literature above:
To ensure the success of the interventions, the nurses need to discuss with the client the nature of the intervention and how it will impact on the client in depth prior to the intervention commencing (Aoun et al., 2016, p.17).
Honest and open communication of information by nursing staff in particular alleviates fears and uncertainty for both patients and carers around the dying process and is clearly evident in this evaluation. It is regarded as a strength of the clinicians and makes up part of the high calibre, professional care given in what are often confronting circumstances for patients, families and carers.
The expert observation by Little Haven nurses described above elicits confidence in GPs who rely upon them for their advanced knowledge and skills in palliative care:
They’re proactive with proposing ideas and suggestions of what they think is needed in the next stage, and that that is so valuable and helpful, because that is, I can’t do home visits all the time. They’re so valuable, they’re like the sort of extended eyes and ears of what I can’t see, and that they have all this experience with them, sometimes their suggestions I wouldn’t have come up with myself, so they would ring me if they have concerns. They send me a fax or an email proposing, you know they have to text in an infection, or the pain is not under control, or they wonder if something else will be valuable. SK8
Further, team members who were engaged in home visits had strong communication processes that ensures regular contact with them throughout the day while on shift:
We’ve got good systems in place to be able to connect in. We use [name of program] on the computer. So that’s a really good system that we can, you know, make sure things are uploaded and happening, we’ve got a good email system, texting system. So we’ve in communication with all of our staff … even when people are sort of out of areas, because there’s quite a few areas that don’t get service. SF4
This staff member clearly articulated the impact of this staff communication on managing the risk of isolation in the community settings serviced by Little Haven:
Not being alone is a part of our model of care. So in the same way that it’s one of the, like, spinal parts of our structures that our clients and families never feel alone in their job, I don’t think as a nurse that I feel alone in the work that I’m doing. But I can always call and even if it’s, if even if I know that a staff member is not working, that I’m really kind of stuck with something or needing to talk, I know, I can call [colleagues], and just go, Can I just talk to you about this? So I feel like what we provide for our clients and families, we also provide for each other. SF3
Telehealth is one approach to clinical care in community-based palliative care services, particularly in regional areas, linked directly to decreased hospital admissions (Spilsbury & Rosenwax, 2017). Little Haven’s model of care extensively integrates telephone contact into its patient care and carer support processes. Further, it will sometimes conduct telehealth consultations in the patients’ home with other services dialling, such as the SCHHS teams. It is noted that, like elsewhere, issues with connectivity and patient/carer capacity to manage the required technology can vary widely.
However, when viewed as an early intervention, telehealth has been observed elsewhere to provide more information to regional services when a home visit is not feasible. The introduction (or expansion) of this element relies upon its co-design with families, staff and volunteers; development and implementation can be complicated, given that it must strive to achieve ‘…a balance between clinical need, consumer benefit, and technical and financial feasibility (Tieman et al, 2014, p.6). Where this has been introduced, it is seen to complement, rather than replace, the face-to-face interaction between clinicians and patients, whilst addressing resource limitations.
4.3.6 Community participation
Little Haven’s model of care is embedded deeply within its community, and it upholds its responsibility to that community. This permeates many of its practices, including its stated responsiveness to patient or referrer inquiry as possible in light of this deep connection:
I think that our responsiveness comes from that community connection. We feel a responsibility to our community, because we’re part of the community …when I work for Little Haven, I think ‘what does the community expect of us?’ and they don’t expect us to put someone off. If somebody reaches out to us and wants our support, then we give our support. SF2
Further, it urges non-professional team members such as friends, relatives, family members, volunteer community members, and spiritual/faith leaders, to provide assistance to patients in any way they can. This mobilisation of informal social networks is central to providing holistic, person-centred care:
The responsibility for supporting those experiencing a life limiting illness, the frail, elderly and bereaved can be shared by the community rather than provided predominantly in family and professional silos … If the confidence and capacity of the community were enabled to respond earlier and to less urgent, practical, emotional and spiritual care for those around them, professional care services would have increased capacity to respond to those with more complex care needs (Stanley & Daddo, 2022, p.11).
There were mixed views about the extent of community awareness of Little Haven in Gympie and surrounds. The Marketplace shopfront was seen to be a pivotal interface between Little Haven and the community, but even there, awareness varied enormously:
A lot of people know about Little Haven, but a lot of people don’t. We run a marketplace … and a big surprise is how many people ask you what Little Haven is about and where does the money go? And a lot of people out there we deal with, a lot of people every day… but people out there don’t know what Little Haven is… You get a lot of the young ones coming through, they don’t know what Little Haven is about. VL5
This bereaved carer’s experience demonstrates this further:
I did know there were palliative care options… despite, as I said before, being involved with the end-of-life care committee, I actually found there were obvious gaps in my knowledge and understanding of how the process was going to be begun, which isn’t Little Haven’s [fault] …I don’t know who to blame. At the time I did feel, why have I not got this understanding and what must it be like for anyone out there who has not even heard of end of life, palliative care? …I thought the GP would kick start the whole thing, so I was waiting for this to come to me… BC4
However, it is clear that once Little Haven was known to community members, it was held in high esteem. They could see it as a service of ‘care and compassion … shown to the family members’ (VL9).
Community engagement is a process element that Little Haven’s model demonstrates clearly. It is actively engaged – beyond fundraising – in its annual “Little Haven Week’ and memorial service, gratitude walks, public forums and Dying2Know Day; it has an online presence on its website and Facebook page.
4.3.7 Financial operations
Little Haven’s efforts to raise funds in the community are one of the ways in which they are known. It certainly is effective when staff and volunteers are seen in shopping centres and public forums (particularly the CEO), however this evaluation identified some lack of clarity amongst participants whether government funding is actually provided in addition to local fundraising efforts. It is thought by some Little Haven service users that the service is underfunded by government and that the amount of fundraising required to offer the service free of charge is excessive. However, it can also be asserted that it is its fundraising that enables Little Haven to raise its profile and be so well-trusted within the Gympie community. To reiterate an earlier point, the locally raised funds remaining in the local community is evidence of this:
There was one other thing that stands out this Little Haven and whatever money is made, stays under the Little Haven umbrella doesn’t go here, there and everywhere and everybody gets a bite out of it. It stays in Gympie and the surrounding district, and that I think is makes it so much more … they’re very personal. VL7
The processes of ‘occasions of service’ measured the financial operations of Little Haven. It typically delivers most occasions of service for allied health and nursing care (~60%), followed by bereavement, social and emotional and care conferencing activities (~25%) and after-hours nursing care (~15%). Notably, the yearly hours of contracted occasions of service by QH were far exceeded by Little Haven by 250%.
Its income in the financial year 2021/22 comprised 61% Government funding (proportionally slightly decreasing) with donations and fundraising representing 34% (proportionally increasing). The highest contributors to overall expenditure were related to staff costs, including wages (65-68%), superannuation (6-7%), and employee benefits (5%). Fundraising expenses contribute around 4% per year, followed by IT expenses with about 3% of expenses. Overall, the economic evaluation demonstrates a net surplus between total income and expenses, with the highest surplus in financial year 2020/21, mostly due to extra COVID-related funding and government subsidies and lower wage-related expenses compared to the last financial year (2021/22).
However, Little Haven far exceeded on contracted deliverables and provided over 30,000 hours of service, resulting in a cost of only $33/hour, representing only 28% of the anticipated cost and resulting in excellent value for money from a QH perspective.
4.4 Outcomes
The products resulting from the structures and processes* of the model of care demonstrate the extent to which Little Haven meets its goals of care. A high degree of congruence exists between the tenets of compassion, care and support within the model, as offered to patients and carers, and the caring orientation of management, staff and volunteers towards each other. This is a service and a model that recognises itself to be situated deeply within its community and upholds its responsibility to that community.
Specific outcome areas are explored below.
* After Donabedian (1980, 2003)
4.4.2 Patient outcomes
As noted in the literature review, about 60-70% of people in Australia prefer to die at home regardless of age (Swerissen, 2014) and it is well-established that receiving palliative care in the home increases the likelihood of death occurring there (Shepperd et al., 2016; Ventura Mde, 2016). Further, in comparison to generalist home-based services, there is improved health-related quality of life among patients receiving specialist palliative care home-based services (Brännström & Boman, 2014; Shepperd et al., 2016).
This key outcome of providing community-based palliative care to enable individuals to stay in their preferred care location for as long as possible, and to die at home if desired, is a notable accomplishment of the Little Haven model of care. As this patient noted, it enabled them to remain at home when presentation to hospital was being contemplated:
Oh, I talked to [nurse] at 11.30pm and she was up, she was doing things, it was her shift. She said sensible stuff. I did it. And I went to sleep on that. Whereas, you know, we were hovering…do we have to go to the hospital again? How long can I avoid it? What are we gambling with? …I find that I can talk to someone I know, outside the medical [hospital] system to gauge what’s really worth doing. PT4
Fulfillment of patients’ preferred place of care and death is an important outcome measure in this context. Little Haven is a strong advocate of fulfilling clients’ needs and ~90% of their clients died according to their wishes (measured in fulfillment of Advance Care plans) which could not be calculated in terms of fiscal costs but rather is emphasised in the context of value for money:
One of the top three fears most people in the world have is fear of dying. It’s the unknown. And I think that earlier entry gives us time to actually help people process that existential angst and all of the questions and all of the fears. You can’t do that overnight. Yeah, you can do that stuff in a few weeks. It takes time for them to accept, to process, and all of those things because it’s so tiring… People say, I’m not scared of dying. I’m not scared of what happens after I die. I’m scared of what’s going to happen between now and then. Because they don’t know. So it’s just being able to talk through and demystify it. Normalise this process, remind them that we’re human beings the same as any other animal, and our systems work very similarly. And just talking them through those things. SF3
4.4.3 Carer outcomes
Community-based palliative care transfers a significant care burden that reduces the pressure on hospitals and the health system. Family carers often carry a greater care burden as a result, and the availability of community-based palliative care is reported to have carers subsequently experience greater sense of support and, ultimately, less complicated grieving (Aoun & O’Connor, 2014; Bajwah et al., 2020; Gomes et al., 2013b; Gomes et al., 2014; Ping, 2014).
The Little Haven Carer Satisfaction Survey provides clear indications that carers of past patients are satisfied with its service provision, and that key objectives of Little Haven in relation to timeliness, collaboration, and respect are fulfilled, enabling the patient die at home, providing high quality of care, and skilful staff engagement with family and carers. Maintaining as full a quality of all areas of life as possible is a central wish of patients and carers, and an outcome of the 24-hour service:
I was surprised at how much availability and how supportive and with phone calls and, you know, the 24-hour service. Like if I do have any questions…I was surprised that there was something out there like that. So instead of having to go through the hospital system to ask all those questions, to have that once you come out of that hospital system and to go into one [organisation] that doesn’t have to follow those protocols…everybody that we spoke to nurse-wise was able to answer the questions, they didn’t have to refer it up. CC1
Over 90% of the respondents indicated that they were ‘Extremely Satisfied’ with Little Haven services. Ninety-five percent or more of respondents expressed their belief (in each case) that their involvement with Little Haven was timely, staff were highly inclusive of patients and carers in care decision-making, preferences of patients and carers were respected, relevant information was communicated clearly, comprehensively and accessibly and personal and cultural beliefs were appropriately recognised. Thanks to the bereavement support service, this reassurance remains after the death of the patient:
I found the staff at Little Haven to be caring, helpful and gave me a sense of security and of not being alone in my time of need. There’s no words to describe the wonderful caring and support I received. I can’t thank all the staff at Little Haven enough. Q3 21-2
This consistently high feedback seen within the Carer Evaluation Survey outcomes are explained by a clinical team member in this way:
I think in particular, it’s not pathologizing, your grief, that, you know, it’s a bereavement support model. So it actually acknowledges that when you have somebody die, particularly if you’ve been a carer for that person, or they’re a very significant person in your life, that it is a significant challenge and struggle, and that you might need, you know, just a little bit of support to get you through that without necessarily needing to diagnose in any way… It’s that continuity of care. SF2
4.4.4 Staff outcomes
There is strong confidence and belief in the Little Haven model of palliative care. Staff members clearly enjoy what they do, believe that they do it well, and are affirmed in their practice by patients and families, management, their colleagues, and the community of Gympie. A high degree of congruence exists between the tenets of compassion, care and support within the model, as offered to patients and carers, and the caring orientation of management, staff and volunteers towards each other. For volunteers, it was seen to be valuable experience to bring to the volunteering role, although there was a strong sentiment of ‘giving back’.
Staff can identify key strengths and benefits of the model and point to organisational structures and processes that promote sustainability. Interestingly, when potential challenges experienced in relation to the model arose in data collection, the challenge was briefly acknowledged and quickly moved to identifying potential or actual solutions to it.
Staff expressed high levels of job satisfaction working in the Little Haven model of care:
I feel that it’s what I am supposed to be doing. I feel incredibly comfortable doing what I’m doing. It’s an incredible honour to do what I do. And just the knowledge that you are making that difference with these people. You walk into a house and these people are so scared, they’ve just been told they are terminal. They have been given this unrealistic prognosis of how long they are going to live and they are scared. And you walk into that house and you go, hi, I’m [name], I’m from Little Haven, and everything is going to be okay. And you talk through what is going to happen and what services we provide, and that we are 24/7…We are frequently in dishevelled in people’s houses at two in the morning. When you walk out the door, they are calm and relaxed. That sustains me that the knowledge that I am doing that. SF11
Resilience to burnout presented as perhaps the most significant outcome for staff as a result of working within the Little Haven model, leading to high staff satisfaction and low attrition:
Field nurses burn out in palliative care. Yes. Somewhere between five and seven years or something. Between five and seven years. For that long, yes. It’s too much. Yes. Now here, I am at nine years. [Colleague name] is nine years. Wow, [Colleague name] is 16 years. [Colleague name] is retired. She would still be there otherwise. She was 70. Yeah, we don’t burn out? SF10
4.4.5 Volunteer outcomes
Like their counterparts in the staff, Little Haven’s volunteers describe enormous satisfaction drawn from their contributions to the service. They see it as both valuable and valued, and understand it to be contributing both to the immediate needs of families and the betterment of the local communities it supports.
It is noted that the current recruitment and retention trends for Little Haven are sufficient for current demand, however it is also seen in Figure 3 in Section 3.2.2 that most existing volunteers are aged 60 and above. Amongst their own numbers, it is acknowledged that the nature of volunteering is changing and that, with time, fewer and fewer volunteers are likely to be available and willing to support the work of Little Haven. Some felt that the situation was manageable for now but not indefinitely:
While we’re all going It’s great. But in 5 years, there’s probably going to be half of us not volunteering. Yeah, so who’s going to replace us? VL4
Although it was suggested that finding ways to recruit younger volunteers, once participant did not view that as a realistic path:
I know that the younger people aren’t gonna volunteer. Their mindset is completely different. Some of them are there talking about being paid. Others, the whole thing is … life is completely different nowadays. People once, they got cared for. There’s less caring in society, a lot less caring. And I suppose if you’re not cared for, you’re not willing to care for others. And there seems to be a lot of that. VL11
This alludes to not only the numbers of potential volunteers to replace the attrition of the current cohort, but the nature of volunteering itself and whether Little Haven will continue to buck the trend widely observed elsewhere.
4.4.6 Community outcomes
The Little Haven model may not be able to be separated as a distinct entity from the community in which it has developed, reflecting its deeply embedded quality. Its structures and processes are both derived from community need and inform community awareness. In this sense, it is a ‘community citizen’ more so than simply a service provider, and this speaks to a critical quality of difference for the organisation. In return for the community investment – both social and financial – in it, Little Haven provides members with holistic, immersive, multidisciplined, high standard palliative care, free of financial cost to the patient and their family. Community members are offered the experience of being held deeply by their community, as they move towards the end of their life. This care is extended beyond death, in the form of bereavement support, and community remembrance.
The community’s familiarity with the issues of death and dying, particularly in the context of an ageing population, is largely viewed as relating to the engagement of the community with Little Haven. This stakeholder considered this against the context of widespread death denial and breakdown of community cohesion:
I think some of this is because we’re such a death-denying society really that … we’re death denying so why would you need to even prick up your ears and understand why Little Haven, what is it? But also I do think that you know all communities are now really struggling with ‘what is a community?’ and trying to engage that community spirit and foster it. There is a lot more individualism now. SK5
This collective lack of readiness becomes quite pointed when confronted with the impending death of a family member, which can have a flow on effect upon the grieving experienced by the bereaved:
…if there’s increased grief, because they haven’t got much exposure prior to this point of people dying and losing a loved one, then then it requires much more support to be given by the nurses and the volunteers and social workers to try and help carry that family through that event. Support family members post death as well. So that puts a huge impost on what the service can deliver when there’s more and more people to care for. SK1
It was interesting to note the varying levels of awareness in both Gympie and surrounding districts of Little Haven. Perhaps not surprisingly, end-of-life care is not something that is widely known about until it is needed, therefore, patients and carers alike, begin to learn about the service offered by Little Haven from the time of admission:
I knew they were there. But then once I realised what they were like, I didn’t realise how extensive their support is, and how ongoing and how they really do look after you. I know I could go up there tomorrow and sit down and they’d make time to have a chat. I wouldn’t feel at all awkward about doing it. BC2
As noted, keeping local fundraising gains in the local community is an important outcome for the community, reflecting the social investment noted above:
There was one other thing that stands out this Little Haven and whatever money is made, stays under the Little Haven umbrella doesn’t go here, there and everywhere and everybody gets a bite out of it. It stays in Gympie and the surrounding district, and that I think is makes it so much more … they’re very personal. VL7
This local benefit is again seen to be a component of their model of care that makes it accountable in a regional town where the population is small and the connections are strong; indeed, rejecting immediate access can have a social cost:
Little Haven Doesn’t turn anyone away … It is a community organisation responsive to our community’s needs. It’s pretty hard to turn down someone when you know that you know the next week … like we’re buying our jams and going down to the Little Haven shop, and you know it’s very much ‘everybody knows somebody.’ You have to be accountable for your actions. SK5
Further to the challenges for volunteering noted above, raising public awareness was seen as critical to facing the challenges of the future, and opportunities were seen in the Marketplace:
Well, I think down at the Marketplace. We need to put more information out, what’s Little Haven? with our signage: Little Haven Marketplace, that could be anything. Palliative care: have you heard that word there or not? “Little Haven Marketplace”, it might give people a better idea. VL5
Maintaining a high profile for Little Haven is essential and attainable, as this volunteer asserts:
… everybody in Gympie can know more about Little Haven, what they do and what they stand for, and why we do what we do in Little Haven … VL12
4.5 Little Haven’s model of care
This extensive appraisal of Little Haven’s model of care, utilising multiple sources of data and an established analytical framework for organisational evaluation, captures a clear picture of the structures, processes and outcomes that constitute the service.
I feel like we [clinical team] are the arms and legs. The business model is the brain. And the community is the heart. That’s the whole organisation. SF11
Little Haven is a well-run community service and, for as long as QH or other government funding can be secured in the future, it is in a strong financial position. Many of the financial benefits of its model of care are evident, including lower health care costs (Abian et al., 2022; Brereton et al., 2017; Smith et al., 2014), and reduced health system costs if provided early (Seow et al., 2022). Community-based palliative care services provided by Little Haven enables individuals to receive care in their preferred location (in most cases their home), whilst reducing time spent in hospital (4.5-7.5days less) and fewer emergency department presentations (2-13% less) in the last year of life (KPMG, 2020). This equates to average health savings of $4,544 (worst case) to $6,109 per person (best case) per year (KPMG, 2020). Further, Little Haven has accrued a substantial amount of cash on hand and total assets with only minor liabilities. Based on Little Haven service provision during the last financial year this would apply to 160 individuals who died during the financial year 2021/22 and were hence in the last year of their life, resulting in indirect cost savings to Queensland of $727,040 in a worst case and $977,440 best case scenario.
However, to some extent, current or future funding models can bring about the centralisation of services currently provided by local organisations like Little Haven and represents a risk to the communities served in the regions.
One other thing that I think, is an under recognised risk for rural services is a desire by departments of health to centralise things. So they need to change the thinking a little bit, and be reaching out to make sure that they are providing as much local service they can, because in the long term that takes pressure off big hospitals in the middle and the centralised services, so that needs to be a piece of awareness for Queensland and help for other government agencies involved in support. SK6
Clearly, Little Haven is regarded as the provider of a very high standard of clinical care and other aspects of holistic care needs. The multidisciplinary clinical staff are seen to be pivotal in this, and again, the notion of going ‘above and beyond’ was clear. Similarly, the volunteers are regarded as essential to the work of Little Haven and at no time was there any indication of hierarchical views of staff versus volunteers. Patients and carers prospectively and retrospectively report high satisfaction with not only the type of services received, but the way these services are delivered. Other service providers are largely supportive of Little Haven’s model of care, particularly those GPs who work most closely with them in shared care arrangements. Where there are multiple services engaged in care, Little Haven undertakes a care coordination role which is essential in the support of patients and their families and carers. Recognising the necessity for self-care in palliative care practice, Little Haven’s staff support strategies are outstanding and clearly enable the challenges of PEoLC provision to be addressed.
In this context of excellent service delivery, there are only a few issues to summarise for Little Haven’s consideration as it continues to evolve and respond to these data and other continuous improvement outcomes (as noted in Section 4.5):
- Securing ongoing funding is clearly an ongoing concern for Little Haven considering current approaches to funding of community-based palliative care. The affordability of Little Haven’s model includes, but goes beyond, an equation of costs for service delivery; it also rests on value for money achieved through its model of care and measured by the critical flow on effects to the health, social and economic outcomes.
- It is reasonable to believe that the volunteering program will be impacted upon by changing social cohesion and volunteering patterns, despite its current stability. An investigation of how other programs are optimising this transition could inform Little Haven’s medium-term planning. Approaches to citizenship based on public health palliative care are found globally that might add value to evolving understanding of community engagement with Little Haven’s work.
- Although liaison with GPs is reported positively by those participating in this evaluation, structural and practice constraints are present that may impact upon Little Haven’s operation. Whilst there are systemic workforce issues relating to General Practice in the region (and beyond) which exceed Little Haven’s remit, its continued attention to sustaining existing, and building new, relationships with GPs in the region is essential.
- It is not clear from this evaluation whether an Aboriginal Health Worker is available for indigenous clients, or if indeed, indigenous people requiring palliative care seek Little Haven’s support. This might be considered when indigenous families receive support from Little Haven in partnership with culturally appropriate services.
- Similarly, it is not clear whether people experiencing, or at risk of homelessness, receive care from Little Haven, whether singly or in collaboration with other services specialising in this area. It is noted that those living alone do successfully receive care from Little Haven. • There are observed barriers to accessibility to allied health and complementary therapies either due to location or declining health, meaning that attending Little Haven premises is not always possible. Carers raised the question whether these could be provided in-home.
- Succession planning is also part of Little Haven’s view of the future. Like many small, community-based organisations, Little Haven has a champion in its CEO, Sue Manton. She is very much the public face and voice of Little Haven and is acknowledged by many as the primary driving force behind its success and sustainability. It is acknowledged that the CEO will one day no longer be in the role, and the Board is cognizant of this, particularly in light of her substantial role in public promotion of the Little Haven model of care and funding opportunities.
4.6 Transferability of model
This evaluation the Little Haven model of care enables identification of key components of Little Haven’s model of care and informs consideration of the replicability of the model in other settings. This was most significantly achieved through a substantial written submission and subsequent address to the Productivity Commission into Reforms in Human Services in 2017:
We decided that we would … send Sue to present at the Productivity Commission. And that was really a game changer for us. We didn’t want to be seen to be blowing our own horn, but she did a wonderful job. And when that report came out, and you go through the report and see how many times Little Haven was referred to… wonderful. And that gave us a tool to then to go to the funding bodies and say, this is this is really good, what we’re doing. SK4
As noted in Section 2.2.4, Little Haven’s model of care demonstrates each of the components identified in the review of the literature and regarded as essential to all models. These components are highly contextualised, and reflect the structure-process-outcomes elements noted above, including:
- Offers a notably early point of engagement post-diagnosis with patients than is broadly practiced in the palliative care sector.
- Is highly flexible in its capacity to meet patient needs on a day to day and overarching basis, and in its support of patient preferences.
- Provides high levels of support for family and carers.
- Integrates care coordination.
- Offers new nursing staff a substantive time to orient to the Little Haven model of care with a one month mentoring process.
- Demonstrates high rates of staff retention and longevity.
It should be noted, these are closely inter-related, rather than distinct from one another; in the subsections to follow, the points above are considered in six key areas.
4.6.2 A ‘citizen organisation’
Where there are cohesive communities with a strong sense of identity and healthcare providers who not simply provide a service but are a clear ‘citizen’ of the community, a partnership between them can attend both to holistic care needs of patients and families and the broader social character of the community in addressing the issues of dying, caregiving, death and grief. It is clear in this evaluation that this characteristic permeates throughout Little Haven’s model and is a significant point of difference at the very foundations of its presence in the Gympie community.
For this reciprocal relationship between service and community to be replicated, the need for knowledgeable, skilled and engaged communities is essential:
That would have to be a part of the model, [if] you’re going to try and regenerate the model anywhere else. I think you have to start with community awareness of death and dying and the potential to have better life transitions. SF10
The community engagement strategies implemented by Little Haven bring both its expertise in, and familiarity with, the issues of dying, caregiving, death and grief and respond to identified community need. This strongly reflects the principles and practices of public health palliative care where partnerships between communities and palliative care services are central to their success.
4.6.3 Regional settings
Under-resourcing and physical distances to health and social care services can impede access to specialist palliative care and it is recognised that regional and rural communities can have PEoLC needs distinct from metropolitan communities (Spelten et al., 2019). This goes beyond the resources required in such communities to the character of the community itself, as noted in the previous subsection.
The Little Haven model of care provides an approach for use in other regional centres. Whilst elements of the model are relevant in many settings, communication processes that enable staff support and safety when visiting patients and families in locations with restricted access is essential; similarly, frequent telephone contact with patients and families to complement face to face visits is a resourceful approach to maintaining both clinical observation and interpersonal links where distance is a factor. Cooperative and trusting partnerships between palliative care services and local GPs, pharmacists and other service providers addresses many of the care needs of patients when larger healthcare centres are harder to access.
4.6.4 Accessibility and early admission
A notable characteristic of the Little Haven model of care is the absence of restrictions on admission – apart from geographical location (and even then, not without exception), any person with a life-limiting illness can seek admission to Little Haven’s service at any point in their illness, regardless of prognosis. This feature comes at a financial cost to the service as it is not supported by current Government funding models, however this evaluation demonstrates clearly the personal and social benefits of early intervention; these include patient stress and carer burden, connection with staff and volunteers at a vulnerable time of need, optimal communication with GPs and other services, and better scaffolding of the grief experienced by bereaved carers.
Replicating the Little Haven model of care in other settings could include an ongoing capture of social data and health service usage relating to these organisational elements, to substantiate economic benefits.
4.6.5 Over and above
Closely related to its place as a ‘citizen organisation’, Little Haven’s practices of going ‘over and above’ are a notable feature of their model. This are not just acts of kindness by clinicians or volunteers in unplanned response to ad hoc need; rather, it is a structural feature of the model that enables its clinicians to take the time required to provide the care needed, and a process feature that sees it responding to its accountability to the communities it serves. In other settings, incorporating this feature into a model of care would require the routine allocation of longer visit times than usual and an established reputation as a compassionate, citizen organisation.
4.6.6 Bereavement support
Like some other components of its model of care, Little Haven’s bereavement support service is not supported by current government funding models, yet in this evaluation, its individual and collective benefit was abundantly evident. Given the consequences of poorly or unattended grief to the health and social wellbeing of individuals and communities, and its impact on health service usage amongst the bereaved, this comprehensive program is a uncommon and a key element of the model.
4.6.7 Resilience to burnout
The prevalence of burnout, and subsequent attrition, of nursing staff is unusually low in Little Haven. This is attributed to its comprehensive staff support program, including close mentorship, monthly meetings and strong interpersonal bonds fostered among the team members. This showcases psychological safety and has efficiency dividends in a regional community where workforce challenges are common.
4.6.8 Final remarks
This ongoing interest in actively encouraging other communities to seed and develop their own version of Little Haven, sharing elements of their model while also being informed by the character and context of the communities in which it sits, is a feasible goal for the organisation to pursue. Critically, such replication is not proposing a ‘cut and paste’ of Little Haven, but the emergence of a community-based palliative care service that is ‘their communities answer to what they need’ (SF1):
It can be replicated in other communities, but we can’t be a service that goes [and sets ourselves up in] other communities, it should grow out of that community, because it is so important to have that basis and the respect of the community and to have the responsibility back to your community. So getting that through to Queensland Health is proving more difficult than I’d hoped. I very much have encouraged other communities to develop a model like Little Haven, yes, but they need their own Little Haven. And it needs to be their community’s answer to what they need. SF1
5. References
Abel, J., Kellehear, A., & Karapliagou, A. (2018). Palliative care-the new essentials. Annals of palliative medicine, 7 (Suppl.2), S3-S14.
Abel, J., Walter, T., Carey, L. B., Rosenberg, J., Noonan, K., Horsfall, D., … & Morris, D. (2013). Circles of care: should community development redefine the practice of palliative care? BMJ supportive & palliative care, 3(4), 383-388.
Abernethy, A. P., Currow, D. C., Shelby-James, T., Rowett, D., May, F., Samsa, G. P., … & Phillips, P. A. (2013). Delivery strategies to optimize resource utilization and performance status for patients with advanced life-limiting illness: results from the “palliative care trial”[ISRCTN 81117481]. Journal of pain and symptom management, 45(3), 488-505.
Abian, M.H., Antón Rodríguez, C. & Noguera, A. (2022). End of Life Cost Savings in the Palliative Care Unit Compared to Other Services. Journal of Pain and Symptom Management.
Aoun, S. M., Breen, L. J., & Skett, K. (2016). Supporting palliative care clients who live alone: Nurses’ perspectives on improving quality of care. Collegian, 23(1), 13-18.
Aoun, S. M. & O’Connor, M. (2014). Home palliative care services increase the chance of adults with advanced illness dying at home and reduce symptom burden without impact on caregiver grief. Evid Based Nurs, 17, 81.
Aoun, S., O’Connor, M., Skett, K., Deas, K., & Smith, J. (2012). Do models of care designed for terminally ill ‘home alone’ people improve their end-of-life experience? A patient perspective. Health & Social Care in the Community, 20(6), 599-606.
Arnold, E., Finucane, A. M. & Oxenham, D. (2015). Preferred place of death for patients referred to a specialist palliative care service. BMJ Support Palliat Care, 5, 294-6.
Australian Institute of Health and Welfare. (2022). National Palliative Care and End-of-Life Care Information Priorities.
Australian Institute of Health and Welfare (2022). The last year of life: patterns in health service use and expenditure. Retrieved from Canberra: https://www.aihw.gov.au/reports/life-expectancy-deaths/the-last-year-of-life-health-service-use-patterns
Bajwah, S., Oluyase, A. O., Yi, D., Gao, W., Evans, C. J., Grande, G., Todd, C., Costantini, M., Murtagh, F. E. & Higginson, I. J. (2020). The effectiveness and cost-effectiveness of hospital-based specialist palliative care for adults with advanced illness and their caregivers. Cochrane Database Syst Rev, 9, Cd012780.
Baumann, A. J., Wheeler, D. S., James, M., Turner, R., Siegel, A. & Navarro, V. J. (2015). Benefit of Early Palliative Care Intervention in End-Stage Liver Disease Patients Awaiting Liver Transplantation. J Pain Symptom Manage, 50, 882-6.e2.
Blackford, J., & Street, A. (2012). Is an advance care planning model feasible in community palliative care? A multi-site action research approach. Journal of advanced nursing, 68(9), 2021-2033.
Blanchard M., Clapham, S., Daveson, B. & Eagar, K. (2022). Patient Outcomes in Palliative Care – Australian National report for July – December 2021. Palliative Care Outcomes Collaboration, Australian Health Services Research Institute, University of Wollongong.
Brännström, M. & Boman, K. (2014). Effects of person-centred and integrated chronic heart failure and palliative home care. PREFER: a randomized controlled study. Eur J Heart Fail, 16, 1142-51.
Braun, V., & Clarke, V. (2006). Using thematic analysis in psychology. Qualitative research in psychology, 3(2), 77-101.
Brereton, L., Clark, J., Ingleton, C., Gardiner, C., Preston, L., Ryan, T. & Goyder, E. (2017). What do we know about different models of providing palliative care? Findings from a systematic review of reviews. Palliat Med, 31, 781-797.
Chatland, L. E., Harvey, C., Kelly, K., Paradine, S., Bhagat, M., & Hudson, B. F. (2023). Research participation in palliative medicine—benefits and barriers for patients and families: rapid review and thematic synthesis. BMJ Supportive & Palliative Care, 13(1), 35-44.
Clarke, V., & Braun, V. (2017). Thematic analysis. The Journal of Positive Psychology,12(3), 297–298.
Collier, A., Morgan, D. D., Swetenham, K., To, T. H., Currow, D. C., & Tieman, J. J. (2016). Implementation of a pilot telehealth programme in community palliative care: A qualitative study of clinicians’ perspectives. Palliative medicine, 30(4), 409-417.
Cross, J., Fischer, A., Shotton, D., Pollicino, C., May, A., Vora, R., … & Good, P. (2020). Supporting choice: an innovative model of integrated palliative care funded by a private health insurer. Internal medicine journal, 50(8), 931-937.
Daddow, A., & Stanley, M. (2021). Heidi’s legacy: community palliative care at work in regional Australia. Social Work in Health Care, 60(6-7), 529-542.
Delgado-Guay, M. O., Kim, Y. J., Shin, S. H., Chisholm, G., Williams, J., Allo, J. & Bruera, E. (2015). Avoidable and unavoidable visits to the emergency department among patients with advanced cancer receiving outpatient palliative care. J Pain Symptom Manage, 49, 497-504.
Disalvo, D., Agar, M., Caplan, G., Murtagh, F. E., Luckett, T., Heneka, N., … & Phillips, J. (2021). Virtual models of care for people with palliative care needs living in their own home: A systematic meta-review and narrative synthesis. Palliative Medicine, 35(8), 1385-1406.
Donabedian, A. (1980). The definition of quality and approaches to its assessment. Health Administration Press.
Donabedian, A. (2003). An Introduction to Quality Assurance in Health Care. Health Administration Press.
Edwards, J., Hooper, D., Rothwell, G., Kneen, K., Watson, J., & Saurman, E. (2019). A nurse practitioner-led community palliative care service in Australia. International Journal of Palliative Nursing, 25(5), 245-253.
Gade, G., Venohr, I., Conner, D., Mcgrady, K., Beane, J., Richardson, R. H., Williams, M. P., Liberson, M., Blum, M. & Della Penna, R. (2008). Impact of an inpatient palliative care team: a randomized control trial. J Palliat Med, 11, 180-90.
Gardiner, C., Ingleton, C., Ryan, T., Ward, S., & Gott, M. (2017). What cost components are relevant for economic evaluations of palliative care, and what approaches are used to measure these costs? A systematic review. Palliative medicine, 31(4), 323-337.
Gomes, B., Calanzani, N. & Higginson, I. J. (2014). Benefits and costs of home palliative care compared with usual care for patients with advanced illness and their family caregivers. Jama, 311, 1060-1.
Gomes, B., Calanzani, N., Curiale, V., McCrone, P. & Higginson, I. J. (2013a). Effectiveness and cost-effectiveness of home palliative care services for adults with advanced illness and their caregivers. Cochrane Database Syst Rev, 2013, Cd007760.
Gomes, B., Calanzani, N., Gysels, M., Hall, S. & Higginson, I. J. (2013b). Heterogeneity and changes in preferences for dying at home: a systematic review. BMC Palliative Care, 12, 7.
Handley, T., Jorm, C., Symington, C., Christie, L., Forbes, E., Munro, A., & Cheney, R. (2022). ‘It sort of has the feel of being at home’: Mixed-methods evaluation of a pilot community-based palliative end-of-life service in a regional setting. Australian Journal of Rural Health, 30(5), 582-592.
Hatton, I., Mcdonald, K., Nancarrow, L., & Fletcher, K. (2003). The Griffith area palliative care service: a pilot project. Australian Health Review, 26(2), 11-18.
Haydon, H. M., Snoswell, C. L., Thomas, E. E., Broadbent, A., Caffery, L. J., Brydon, J. A., & Smith, A. C. (2021). Enhancing a community palliative care service with telehealth leads to efficiency gains and improves job satisfaction. Journal of telemedicine and telecare, 27(10), 625-630.
Hussainy, S. Y., Box, M., & Scholes, S. (2011). Piloting the role of a pharmacist in a community palliative care multidisciplinary team: an Australian experience. BMC palliative care, 10(1), 1-12.
Independent Hospital Pricing Authority. (2021). National Hospital Cost Data Collection Report. Public Sector, Round 24 (Financial Year 2019-20). Retrieved from https://www.ihacpa.gov.au/sites/default/files/202208/NHCDC%20Round%2024%20Report_0_0.pdf
Kaufman, B. G., Granger, B. B., Sun, J. L., Sanders, G., Taylor, D. H., Jr., Mark, D. B., Warraich, H., Fiuzat, M., Steinhauser, K., Tulsky, J. A., Rogers, J. G., O’Connor, C. & Mentz, R. J. (2021). The Cost-Effectiveness of Palliative Care: Insights from the PAL-HF Trial. J Card Fail, 27, 662-669.
Kilonzo, I., Lucey, M. & Twomey, F. (2015). Implementing Outcome Measures Within an Enhanced Palliative Care Day Care Model. J Pain Symptom Manage, 50, 419-23.
King, K. (2021). Gold Standard Community Palliative Care- The Little Haven Palliative Care Model of Care. Unpublished paper.
KPMG. (2020). Investing to save: the economics of increased investment in palliative care in Australia: Palliative Care Australia.
Lam, T. C., Chan, S. K., Choi, C. W., Tsang, K. C., Yuen, K. K., Soong, I., Wong, K. H., Lui, L., Lo, S. H., Tong, M., Lo, R. S. K., Lam, P. T., Lam, W. M. & Li, B. (2021). Integrative Palliative Care Service Model Improved End-of-Life Care and Overall Survival of Advanced Cancer Patients in Hong Kong: A Review of Ten-Year Territory-Wide Cohort. J Palliat Med, 24, 1314-1320.
Luta, X., Ottino, B., Hall, P., Bowden, J., Wee, B., Droney, J., Riley, J. & Marti, J. (2021). Evidence on the economic value of end-of-life and palliative care interventions: a narrative review of reviews. BMC Palliat Care, 20, 89.
MacWilliams, J., Bramwell, M., Brown, S., & O’Connor, M. (2014). Reaching out to Ray: delivering palliative care services to a homeless person in Melbourne, Australia. International journal of palliative nursing, 20(2), 83-88.
Mitchell, G., & Price, J. (2001). Developing palliative care services in regional areas: the Ipswich Palliative Care Network model. Australian family physician, 30(1), 59-62.
Mularski, R. A., Puntillo, K., Varkey, B., Erstad, B. L., Grap, M. J., Gilbert, H. C., Li, D., Medina, J., Pasero, C. & Sessler, C. N. (2009). Pain management within the palliative and end-of-life care experience in the ICU. Chest, 135, 1360-1369.
Nagarajan, S. V., Lewis, V., Halcomb, E., Rhee, J., Morton, R. L., Mitchell, G. K., … & Clayton, J. M. (2022). Barriers and facilitators to nurse-led advance care planning and palliative care practice change in primary healthcare: a qualitative study. Australian journal of primary health, 28(2), 151-157
Namasivayam, P., Bui, D. T., Low, C., Barnett, T., Bridgman, H., Marsh, P., & Lee, S. (2022). Use of telehealth in the provision of after-hours palliative care services in rural and remote Australia: A scoping review protocol. Plos one, 17(1), e0261962.
National Health and Hospitals Reform Commission. (2009) A Healthier Future for All Australians – Final Report of the National Health and Hospitals Reform Commission. June 2009.
Nysaeter T.M., Olsson, C., Sandsdalen, T., Wilde-Larsson, B., Hov, R., & Larsson, M. (2022). Preferences for home care to enable home death among adult patients with cancer in late palliative phase -a grounded theory study. BMC Palliative Care, 21, 49.
O’Brien, A. P., Bloomer, M. J., McGrath, P., Clarke, K., Martin, T., Lock, M., … & O’Connor, M. (2013). Considering Aboriginal palliative care models: the challenges for mainstream services. Rural and Remote Health, 13(2), 1-10.
O’Connor, M., Palfreyman, S., Le, B., & Lau, R. (2016). Establishing a nurse practitioner model to enhance continuity between palliative care settings. International Journal of Palliative Nursing, 22(12), 581-585.
Palliative Care Australia. (2018). Palliative Care Service Development Guidelines.
Patel, M. & Noonan, K. (2022). Community development: compassionate communities. In Abel, J. & Kellehear, A. Oxford Textbook of Public Health Palliative Care (1st ed.). Oxford University Press.
Pellizzari, M., Hui, D., Pinato, E., Lisiero, M., Serpentini, S., Gubian, L., Figoli, F., Cancian, M., De Chirico, C., Ferroni, E., Avossa, F. & Saugo, M. (2017). Impact of intensity and timing of integrated home palliative cancer care on end-of-life hospitalization in Northern Italy. Support Care Cancer, 25, 1201-1207.
Phillips, J. L., Davidson, P. M., Jackson, D., Kristjanson, L., Bennett, M. L., & Daly, J. (2006). Enhancing palliative care delivery in a regional community in Australia. Australian Health Review, 30(3), 370-379.
Ping, L. S. (2014). Cochrane review summary for cancer nursing: effectiveness and cost-effectiveness of home palliative care services for adults with advanced illness and their caregivers. Cancer Nurs, 37, 84-5.
Poulos, R. G., Harkin, D., Poulos, C. J., Cole, A., & MacLeod, R. (2018). Can specially trained community care workers effectively support patients and their families in the home setting at the end of life?. Health & Social Care in the Community, 26(2), e270-e279.
Quinn, K. L., Stukel, T., Stall, N. M., Huang, A., Isenberg, S., Tanuseputro, P., Goldman, R., Cram, P., Kavalieratos, D., Detsky, A. S. & Bell, C. M. (2020). Association between palliative care and healthcare outcomes among adults with terminal non-cancer illness: population based matched cohort study. BMJ, 370, m2257.
Romanò, M., Bertona, R., Zorzoli, F. & Villani, R. (2017). [Palliative care in the intensive cardiac care unit: a new competence for the cardiac intensivist]. G Ital Cardiol (Rome), 18, 685-695.
Rooney, E. J., Johnson, A., Jeong, S. Y. S., & Wilson, R. L. (2022). Use of traditional therapies in palliative care for Australian First Nations peoples: An integrative review. Journal of Clinical Nursing, 31(11-12), 1465-1476.
Rosenberg, J. P. (2007). A study of the integration of health promotion principles and practice in palliative care organisations. (Doctoral thesis). Queensland University of Technology.
Rosenberg, J. P., Horsfall, D., Leonard, R., & Noonan, K. (2018). Informal care networks’ views of palliative care services: Help or hindrance? Death studies, 42(6), 362-370.
Rosenwax, L., Spilsbury, K., Arendts, G., McNamara, B., & Semmens, J. (2015). Community-based palliative care is associated with reduced emergency department use by people with dementia in their last year of life: a retrospective cohort study. Palliative medicine, 29(8), 727-736.
Sahlen, K. G., Boman, K. & Brännström, M. (2016). A cost-effectiveness study of person-centered integrated heart failure and palliative home care: Based on a randomized controlled trial. Palliat Med, 30, 296-302.
Saurman, E., Allingham, S., Draper, K., Edwards, J., Moody, J., Hooper, D., … & Eagar, K. (2022). Preferred place of death—A study of 2 specialist community palliative care services in Australia. Journal of Palliative Care, 37(1), 26-33.
Seow, H., Barbera, L. C., McGrail, K., Burge, F., Guthrie, D. M., Lawson, B., Chan, K. K. W., Peacock, S. J. & Sutradhar, R. (2022). Effect of early palliative care on end-of-life health care costs: a population-based, propensity score-matched cohort study. JCO Oncol Pract, 18, e183-e192.
Shepperd, S., Gonçalves-Bradley, D. C., Straus, S. E. & Wee, B. (2016). Hospital at home: home-based end-of-life care. Cochrane Database Syst Rev, 2, Cd009231.
Smith, S., Brick, A., O’hara, S. & Normand, C. (2014). Evidence on the cost and cost-effectiveness of palliative care: a literature review. Palliat Med, 28, 130-50.
Spelten, E., Timmis, J., Heald, S., & Duijts, S. F. (2019). Rural palliative care to support dying at home can be realised; experiences of family members and nurses with a new model of care. Australian journal of rural health, 27(4), 336-343.
Spilsbury, K. & Rosenwax, L. (2017). Community-based specialist palliative care is associated with reduced hospital costs for people with non-cancer conditions during the last year of life. BMC Palliat Care, 16, 68.
Stanley, M. A., & Daddow, A. A. (2022). Well, what do You Want to do?’ A Case Study of Community Palliative Care Programme: ‘Heidi’s Have a Go. OMEGA-Journal of Death and Dying, 00302228211052801
Swerissen, S. (2014). Dying Well. Grattan Institute.
The Agency for Clinical Innovation. (2013). Understanding program evaluation: an ACI framework. www.aci.health.nsw.gov.au
Tieman, J. J., Morgan, D. D., Swetenham, K., To, T. H. M., & Currow, D. C. (2014). Designing clinically valuable telehealth resources: processes to develop a community-based palliative care prototype. JMIR Research Protocols, 3(3), e3266.
Tieman, J. J., Swetenham, K., Morgan, D. D., To, T. H., & Currow, D. C. (2016). Using telehealth to support end of life care in the community: a feasibility study. BMC palliative care, 15(1), 1-7.
Trtchounian, A., Aberger, K. & Nelson, J. (2017). Early palliative care consultation associated with decreased length of stay. Annals of Emergency Medicine, 70, S115.
Ventura Mde, M. (2016). Effectiveness and cost-effectiveness of home palliative care services for adults with advanced illness and their caregivers. Sao Paulo Med J, 134, 93-4.
Woodman, C., Baillie, J. & Sivell, S. (2016). The preferences and perspectives of family caregivers towards place of care for their relatives at the end-of-life. A systematic review and thematic synthesis of the qualitative evidence. BMJ Support Palliat Care, 6, 418-429.
World Health Organization. (2020). Global Atlas of Palliative Care at the End of Life, 2nd Ed, WHO.
Yosick, L., Crook, R. E., Gatto, M., Maxwell, T. L., Duncan, I., Ahmed, T., & Mackenzie, A. (2019). Effects of a population health community-based palliative care program on cost and utilization. Journal of palliative medicine, 22(9), 1075-1081.
Youens, D., & Moorin, R. (2017). The impact of community-based palliative care on utilization and cost of acute care hospital services in the last year of life. Journal of palliative medicine, 20(7), 736-744.
6. Appendices
Appendix 1: Ethics approval

Appendix 2: Suite of Research Participant Information Sheets and Consent Forms






Appendix 3: Search history



Appendix 4: Guidance questions for participant groups data collection
Patient
- I want to ask you about your experience with coming into LH’s care.
- What are some of the things that led you to become involved with Little Haven?
- How were you referred? How quickly did LH respond to your referral?
- What are your expectations around what LH will provide? Are these being met?
- What has the communication with LH been like since you’ve become involved with the service?
- LH asks this question of its new patients: ‘What do I need to know about you to best look after you?’. So perhaps a question: What are some of the things that are important to you at this time? How is LH responding to this?
- What stands out to you about your experience with LH? Has anything surprised you about LH?
- Is there anything that is not currently offered by LH that you feel might be helpful?
- Have you had any concerns about your experience with LH? Have you been able to communicate these concerns? How responsive have LH been to your expressed concerns?
Carer of Patient (living) - I want to ask you about your experience of LH as a carer/family member of {name of patient}.
- What informed your decision to go to LH for support during {name of patient} illness?
- What are your expectations of LH for {name of patient}, and for you? How are these being addressed?
- Do you feel connected with the team at LH?
- Have you been able to make use of the allied therapies {list examples} available at LH for carers?
- What are some of the things that stand out for you when you think of your experiences with LH during this time? What are the particular strengths of the LH approach for your as carer?
- What is your experience of communication with LH (service/team)?
- Have you had any concerns about your experience with LH? Have you been able to communicate these concerns? How responsive have LH been to your expressed concerns?
- Reflecting on your experience, what changes to the present approach of LH to the support of carers could improve their support?
- How do you think LH is viewed in the Gympie community/region?
Bereaved Carers:
- How have you found the bereavement support provided by LH?
- What were your expectations? Were these met?
- Was the bereavement support that was offered helpful in terms of understanding your experience of grief?
- What were the elements that you found most supportive?
- Were you happy with the follow-up contact: timing and frequency?
- What stands out to you about this experience?
- Have you had any concerns about your experience with LH? Have you been able to communicate these concerns? How responsive have LH been to your expressed concerns?
- Was there anything that was not done, that could have been helpful? Was there anything that could have been done differently?
- Have you been able to make use of the allied therapies {list examples} available at LH for carers?
- Do you still feel connected with LH? Do you feel connected with your broader community in receiving support in your grieving?
Key Stakeholders
- Tell me about your connection to LH. Is it clear to you how LH and you/your organisation relate?
- What are the strengths of the relationship between LH and you/your organisation?
- What could be done differently? What would be the change if this happened?
- When you think about the approach LH takes to providing palliative care, what do you believe it’s doing well?
- What could LH do differently? What would be the change if this happened?
- How aware is the Gympie community/region of LH?
- How is LH understood in this community? Do community members know what LH does?
- What are the priorities in the community that LH could plan for in the future?
Focus Groups – Staff/Volunteers
- Briefly, what drew you to LH? what sustains you at LH?
- I’m interested in your experiences of the LH Model of Care – in other words, the approach that LH takes to providing palliative care, and its place in the community.
- What are some of the standout features of the model?
- What are the strengths of this approach? What are the benefits of the model for patients and carers?
- What challenges for you or LH more broadly lie in this approach? What could be done differently? What would be the change if this happened?
- How would you like to see the model grow?
- How could you express any concerns you might have about LH’s approach? Have you experienced this? How were your concerns received?
- What capacity to you believe you have to contribute to the ongoing development of the LH model?
- How aware is the Gympie community/region of LH?
- How is LH understood in this community? Do community members know what LH does?
- What are the priorities in the community that LH could plan for in the future?
- Acknowledgement of staff contribution
Appendix 5: Carer satisfaction survey