Community Based Palliative Care – Little Haven a working model.
I am incredibly nervous about addressing a group of health care professionals with better credentials in palliative care than I, and nervous that my emotions will overcome me. Because currently my mum’s glioblastoma multiforma, diagnosed 14 months ago, is catching up with her and my partner is looking after her at her home in Salisbury so I can be here. Truth is it’s rare for me not to get emotional when I talk about Palliative Care – but today especially this could be very tricky.
So here I am armed with the tools provided by my very nurturing staff… Emergency Essence (It’s not just Brandy you know- if you listen closely you can hear the flower vibrations) and this rock which apparently will keep me grounded. Let’s see how they go.
Because with so much of the current talk in Palliative Care being around Community connection I have a wonderful story to share about community based palliative care in rural and regional Qld and I have a pressing need to tell it.
I had great plans to give you a biopic of access to community based palliative care across rural Qld and the services providing them but when I sort out info on this from Louise Welch she shut that idea down pretty smartly.
“You can’t talk about that, you can only talk about what you know. Talk about Little Haven”.
Frank as always – she was also right.
More qualified people than me have done reports, modelling, scoping of state-wide palliative services. I am only qualified to talk about what community based palliative care can look like when a community puts value in care of the dying.

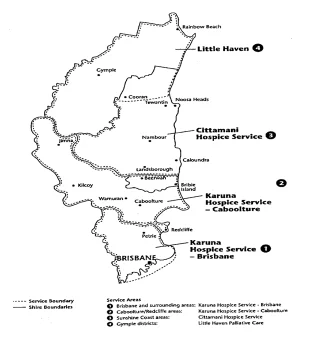
Little Haven Community Based Palliative Care
She gathered together a group of friends with the aim of building a hospice in Gympie for terminally ill patients. For years, this group, solely funded by the community, literally operated out of the boot of a car, providing cancer support, respite care and equipment loans whilst raising funds for their vision. Over the years this vision changed to echo the sentiment of the community, from building a stand-alone hospice to providing hospice in the home.
Much of the money raised by this group went towards setting up two palliative care rooms in the Gympie General Hospital. These rooms continue to provide the only 2 dedicated palliative care beds in the Gympie region.
In 1989 Little Haven Cooloola / Sunshine Coast Palliative Care became an incorporated organisation. A full decade before palliative care was on the Qld health care radar.
In 1999 when under a Federal Government initiative, Queensland Health provided project funding for palliative care services, Karuna, Cittamani and Little Haven became the first partially funded community based Palliative care services.
Funding is also provided under this initiative to 3 outstanding community based hospices in regional areas of Qld – Hopewell Hospice –on the Gold Coast, Toowoomba and Ipswich Hospices.
I was a fledgling on the Little Haven committee then, but I recall Karuna’s Director Venerable Yeshe Khadro being the driving force in seeking recognition and funding for our model of care.
Little did this group of pioneers dream what they were setting the foundation for, as these organisations would grow and flourish over the next 20 years to become respected and established services in their local communities – providing home based palliative care for thousands of Qld families.
With funding secured a permanent home for Little Haven was found in the Gympie General Hospital grounds (the old maternity ward). Many of our patients were either born themselves or bore their children in our building and there is a great comfort and synergy in this circle of life. Being onsite has allowed us seamless communication and ease of transition from hospital to home ~ and vice versa.
Happily ensconced in our new home, nurses were employed to provide care 24 hours a day, 7 days a week. A full range of palliative services was made available to patients in our region. From humble beginnings today Little Haven’s team of 10 specialist nurses headed by the beautiful Bronwyn, 2 bereavement support staff, 52 respite care volunteers and 10 complementary therapy volunteers, work with the treating doctors, to provide comprehensive support for the physical, emotional, psychological and spiritual needs of the individual.
For my part when the opportunity arose to take on the management of the organisation 13 years ago and I jumped at it. And so began my passionate involvement with community based palliative care in our region and in serving the community who were so engaged with our mission.
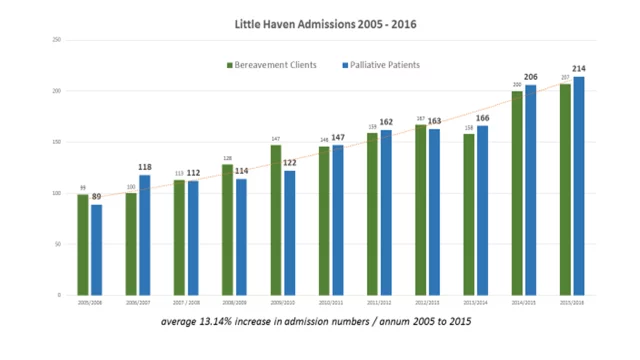
Building a community based Palliative care service that initially cared for around 40 palliative patients a year to 214 in the last financial year. We work tirelessly to ensure our wonderful nurses have the resources and support to provide whatever was needed to meet all the nationally recognised standards of palliative care for every patient who sort our service.
SLIDE (Service statistics)
I’m incredibly proud of Little Haven’s nurses (3 of whom are here today Carolyn, Kelly and Georgie) and am passionate about our community based Palliative care model. Like many of you here I’ve been a staunch advocate for community based palliative care for many years.
My Mum’s story
However it seems life when you least expect it has a way of jumping out at you and shaking you to the core. So it did 14 months ago, as I sat with mum in the Wesley Hospital anxiously awaiting her MRI results.
Hoping for a distraction from our gloom I turned on the TV and up popped Tony Jones and a Q&A episode on Palliative Care – what are the odds? Professor Deb Parker’s words filled the air
“Palliative Care shifts the focus to quality of life not quantity”…. “We call palliative care low tech, high touch”.
I turned it off as these words, which I’d often used myself sounded strangely hollow. I wanted QUANTITY, I wanted HIGH tech and I desperately wanted to hear the word Curable. No doubt this was the shared experience of the 214 families who’d walked through Little Haven’s door that year.
That night, still reeling, I opened the Little Haven website determined to change the palliative care message but was instead comforted as the first graphic loaded….. “Don’t give up – the beginning is always the hardest”, and so it is.
The site like our service emphasised HOPE and it emphasised support – practical and emotional, and it offered COMFORT through access to an extensive range of life affirming complementary therapies.
Our Community Based Palliative Care Model
This is our mission and this is our message – Compassionate Care and LIVING SUPPORT because whilst we may like to focus on “Let’s talk about dying” so many of our patients come to us with everything to live for and may only come to accept death in the hour it is inevitable.
Reflecting on some of the heart breaking patients we have cared for this year, their tenacious fight for life meant our service was there working alongside the oncology team, the radiotherapists, the specialist services and most importantly the GP as they sought every treatment available to prolong life and our job was to relieve the burden of disease and nurture the spirit – the spirit of those dying and the spirit of those being left behind.
For how does a young mother ever accept leaving her children, how does the Mayor of our town hand over his vision for the region, how does a family let go of their teenage child or a man leave the love of his life alone in this world – her carer for years as her dementia increased?
The value of our community based Palliative care service was to provide all the support and comfort they needed TO LIVE …..practical, technical, clinical support and all the nurturing they needed to find the peace to relax into dying. Our nurses provide HIGH TECH and HIGH TOUCH care.
Our model of care values
Early intervention of palliative care to support patients from their point of diagnosis
Of note the average number of patients on our books at any given time has nearly doubled in less than 5 years; from 38 in 2012 to a current average of 74 patients on our books at any given time. Families are accessing support earlier and staying with us longer– just as we’d hoped.
With a growing body of evidence demonstrating the benefits of early intervention of palliative care, like much of Little Haven’s history we’ve done instinctively what research is now confirming.
Supporting patients through active treatments
We receive regular referrals from the visiting oncologists for support during their cancer treatments. With one carer recently saying she was simply told by her oncologist,
“go and see Little Haven, patients who have their support do better than those that don’t”.
Providing support in the patients environment of choice
From the Gratten institutes report into dying well.
Dying in Australia is more institutionalised than in the rest of the world. Community and medical attitudes plus a lack of funds for formal community care mean that about half of Australians die in hospital, and about a third in residential care. Often they have impersonal, lingering and lonely deaths; many feel disempowered. Seventy per cent of people want to die at home, yet only about 14 per cent do so. People are twice as likely to die at home in countries such as New Zealand, the United States, Ireland and France.
…. And that’s a disgrace
This places a high cost burden on the health system, and potentially a poorer quality of death. Little Haven consistently averages well above these stats supporting over 60% of our patients remaining at home to die in the past reporting period and a further 24 % dying with less than 5 days in Hospital (Given the age of our population that’s exceptional) – Cittamani’s stats are similar if not better.
Educating and empowering families to care for their loved ones – backed up by our 24/7 support
Genuine after hours care not just telephone support!
Dr Heather Richardson – PCV Conference in July 2016
“[Carers] are the people doing the majority of end-of-life care and they have appallingly small amounts of training. Training them will give them the skills and confidence they need to deliver high quality care to people in the latter years of life.”
Shaping compassion by community engagement in care of the dying
The very core of our model
Equitable access for all through provision of all services on a no fee basis
Clinically our patients are very well supported with many local GP’s providing extremely good palliative support, home visits and after hours advice. This relationship – one of mutual professional respect has been fostered across the years.
Slide Dr Dodt LH
We are the GP’s foot soldiers and our patients advocates.
The commencement in 2008 of the Sunshine Coast specialist pall care service visiting Gympie was the icing on the cake. Our patients with more complex clinical needs have specialist support, access to their multidisciplinary team and excellent inpatient management at Dove House if needed.
How lucky are we to have the likes of Louise Welch and Prem Ram to guide our clinical care when management outside of the scope of the GP is needed? Our care is enhanced by the weekly clinical case conference with this service and our nurses learn so much by sitting in on the fortnightly outpatient clinics with our patients (when appropriate).
Nursing and clinical care are unceasing; they take the majority of our resources. Our nurses visiting patients across a 70 km radius from our base (60% greater than 20 kms away), 3 vehicles on the road daily they navigate all kind of terraines across our beautiful region. Rainbow Beach, Kilkivan, Mary Valley, Boreen Point
A few examples…….
The nurses will check if the patient is febrile and if so they need to attend the hospital, which is the last thing they want to do. Invariably they will ask that the nurse come out. She goes. Gives the antiemetic and then gently explains what post chemo neutropenic sepsis is and its risks. The outcome is as you would expect, the patient comes into hospital for appropriate management.
This kind of nursing presence and monitoring is key to the successful outcome of the chemo treatment they’ve chosen to embark on. In some cases the nurse has actually transferred the patient to hospital herself.
8 months later… our on-call nurse received a phone call late Saturday from his children concerned and pleading for nursing presence at their Mums house. She attended and found a very distraught woman clearly on the edge of breakdown and experiencing complex grief. With LH bereavement support (previously refused) I am pleased to report she is emerging from the fog of her loss. She continues to access complementary therapies and attends regular 1:1 sessions with our bereavement worker.
Ascites taps, wound dressings, care plan alterations, medication management, dietary advice, manual handling training, referrals for services, Advanced Care Planning, Range of movement and physio, diversional therapy, occupational therapy, Social work services, bereavement services…… all supplied at no cost to the consumer 24 hours a day, 365 days a year.
But our service is so much more …. In addition to our nursing care Little Haven Community based Palliative care provides
All Equipment Required
All the equipment needed in that care delivered to our patients home as soon as it’s needed by The St Vinnies men, loaned out without charge including:
- electronic beds
- medical supplies
- dressings
- O2 concentrators
- beds
- utensils to ease ADL’s
- continence aids
Mostly sourced from community donations like the Historical MCC, who’ve donated the funds raised from their Poker Run year in year out for as long as I can remember, with one member telling me how good he felt when he saw the recliner chair providing such comfort for his dying friend bore the plaque – Kindly donated by The Historical Motor Cycle Club of Gympie.
Our equipment is also accessed by
- Qld Health OT’s
- The Private Hospital
- Nursing Homes
to enable patients to remain ‘in place’ as their care needs increase.
Respite Care
Our volunteers provide respite care, carer support, transportation and even handyman services in some cases – As an example of what we can do, we recently taught a patient how to use e-mail and the internet, broadening his world of opportunity enormously.
Complementary Therapies
Little Haven Community based Palliative care first offered complementary therapies in 2002 when they were viewed by many as pseudo-science. That may be so for how can science explain a 54 year old aboriginal man’s elation after one of these deep relaxation therapies, saying I’m no longer afraid to die – having seen his mother beckoning him home.
Today our number of therapies on offer are extensive
All provided by professional therapists who donate their time to Little Haven’s community based Palliative care services. And the Dr’s have come around too –even referring patients specifically for access to our therapies. Sarah the Pall Care Reg wants me to tell you about Lynda who she referred to us for support
Lynda and her son came to our centre to do art therapy together and her husband benefited from the deep tissue massage he received from Peter our Masseuse and also the opportunity to talk to Peter in a safe environment about his fears for his wife. Sarah is amazed by the change in the whole family.
Bereavement Support
Bereavement support (formally introduced in 2004) is there for as long as needed for anticipatory grief or after a loss. Through one on one counselling or regular support groups, and more often than not just adhoc as our bereaved know they can call or come in to the centre whenever they feel low and someone will be there “Ah Lyn – you look like you need a hug”. Our recently started a walking group is starting to gain traction too. (Pardon the pun)
Community Education
Resource Library and Education and Increasing Awareness of Advance Health Planning. Little Haven hosts forums for health professionals and the community on issues of aging, advanced health planning, palliative care, loss and grief. Community Forums like “Living Well ~ Dying Well” attended by over 100 older local residents help our aging population prepare for a quality end of life.
The addition of a social worker to our team this year has greatly assisted patients and their families with advanced care planning and ensuring they have clearly articulated their health care choices and end of life options. (The best part is we can meet their end of life options)
A holistic non clinical approach recognising it’s more important to know the person who has the disease than it is the disease the patient has. (One of Hippocrates better quotes)
Back to mum
About this time last year, my brother, mum – now a couple of weeks post op and I, had a bedside meeting with Viv the Neuro-Oncology Nurse Practitioner at Wesley Hospital. Mum, on asking (as they do), was gently told her prognosis and really from this point she would need 24 hour supervision.
After Viv left it was mum who broke the silent gloom.
“Well what was the point of surgery if that’s all that lies ahead”?
Mum’s hope was to go home and have some normality in her life and despite the risks of this decision it was up to us to make it happen, because without hope there was no point.
Accessing outside services proved difficult, arduous, an endless round of assessments – outsourced to contractors with little knowledge of health. Remember this coincided with the new My Aged Care system and the system seemed broken – mums’ initial assessment was by a fireman from NSW who frankly should have stuck to calendars as secondary income.
And it seemed services were more focused on what they couldn’t provide than what they could. Given I was about to hand over some of the care of my mum, 79, physically vulnerable and living alone, to strangers, I thought it reasonable to enquire as to who would have access to her keys, what sort of training or security checks they had? But instead my questions were met defensively.
If the system was hard for me how must it be for others, and I was infuriated on behalf of every lay person being subjected to the stream of acronyms and random questions about packages and prognosis. It lacked the warmth I’d assumed those facing these tough decisions would be afforded.
A Clinical, Confusing and Unhelpful System
They needed re-educating and I had no problem letting them know ….
“This is a stressful time for families”, I said “how much nicer would it be if you simply told us how you could help?” and …. “No! You’re wrong, mum pursuing the best treatment options available (Surgery, Chemo and Radiotherapy) does not make her ineligible for palliative support”.
It’s NOT an either or scenario.
I (the carer) needed the cloak of palliative care right at the start, because I was terrified for mum and for all of us, I needed a place to fall apart then and at any time in the future when the going got tough. I needed to know who’d be there to prop us up as we provided the same care for my mum I had seen countless others in our community do for their loved ones.
A gentle calm amidst the clinical whirlwind of disease and treatments and specialist appointments and blood tests we’d suddenly been thrown into, and practical help to gain resources to meet mum’s needs and wishes, not 6 months, 3 months or even 3 weeks down the track. I needed it then and I as an advocate for palliative care expected it then, and I didn’t know why it wasn’t a given.
Mum had just been told she has a brain tumour for goodness sake and whilst she had a remarkable team of caring specialists (The A team in fact) who were completely focused on treating this terrible disease …. but after you step out of the edifices of Cancer Care – what then?
If mum lived in our rural community we would have known to go into Little Haven and immediately we would have had someone to help shoulder the weight, someone to help navigate the treatment options available and someone to help alleviate the impost of these treatments. Because that’s what a caring community does when one of their own needs support.
COMMUNITY
We have created an outstanding working model of community based palliative care and it is there for all in our community who need it – at no charge.
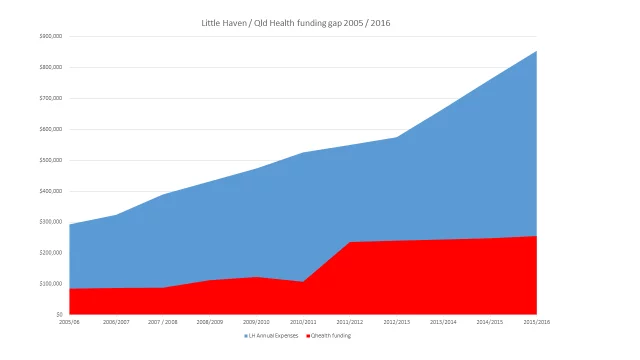
Little Haven receives under 35% of our annual budget from Government funding ($255K project funding annually) – So how do we fund our care?
(SLIDE Funding Graph)
To answer that question first you have to remember that we’ve never turned away a patient in need. We have only ever expanded our boundaries, added more nursing staff and services and just cared for people via our community based Palliative care model.
The key is community and I will show you that is in numbers.
(SLIDE LH Source Funding Graph)
Our fundraising calendar is diverse and exhausting – this month’s especially so, but it fills our cup – not just financially
For example, on Saturday and Sunday just gone the Rotary Club of Gympie held a Quilt and Craft spectacular with proceeds of the 2 days coming to Little Haven. During that 2 days 30 Little Haven volunteers ran the café making all the food ourselves we raised just on $10,000 which to give you an idea of how busy that was our most expensive meal was $10. Monday we were back in the kitchen preparing for our annual Melbourne Cup Luncheon where we make and serve a 2 course sit down lunch for 220 racegoers. This annual event on our calendar raising $12,000.
I can think of no better way to capture the magic of Little Haven’s community based palliative care and the great privilege of being the conduit for community generosity than to recount the events of Tuesdays fundraising lunch.
- Staff, Volunteers and Committee working congenially side by side. An 80+ year old volunteer wielding the electric knife in the kitchen for literally hours without complaint.
- Other community groups cheerfully lending a hand to make the day flow. Rotarians helping with set up and running the bar, prizes donated by local businesses for Diana’s multiple raffles
- The local St Pat’s year 10 students serving the food.
- The generosity of this community in opening their hearts, talents and wallets to us purchasing tickets, sweeps, sponsoring trotters the list is endless
- A glance around the crowd – long time supporters who have been at our functions from day one and most poignantly the families of people we have cared for. How lovely it is to see them 2, 5, 10 years down the track, still grateful, for the care they received for their loved one and wanting to give something back.
Little Haven has a small army of 120 registered volunteers who run a myriad of Fund raising activities including
- Pop Up shops and Shed Sales
- Dynamic list of events
- Annual monster book sales
- A constant calendar of raffle selling
But it is more than the money…
Our fundraising volunteers are out in the community raising awareness and representing Little Haven on a daily basis. They are often the first contact people will have with our service.
Many volunteers have had firsthand experience of Little Haven’s community based Palliative care, as they were a wife, husband, brother or sister of someone we have cared for. Many come through our bereavement support and become a volunteer with a desire to ‘give something back’. In return they express feeling a renewed sense of purpose “lifting the fog of grief’.
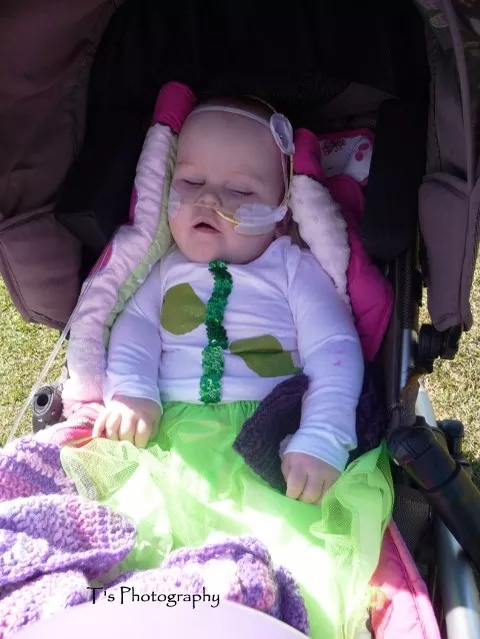
Supporting this beautiful family to pack all the love they could into Paigies short life.
Little Haven visited regularly often daily for just on 12 months, to manage her fitting and other care needs associated with her congenital encephalopathy.
Darren a qualified chef volunteered his time in the kitchen on Tuesday. During a quiet moment, I asked him if he could sum up in a few words how LH’s involvement helped their journey with Paige. He automatically said he would need at least half an hour but then offered
- You always came to our home when we needed you and you were always there. We know of others in the city who never have any specialist care provider visit at home and so we realise how fortunate we were.
- Your nurses just blended and moulded into our home life and family ways, always supported our decisions and worked to fulfil the way we wanted to do things, never questioned our ideas and always made it seem it was possible for us to have things the way we wanted them.
- Whenever I walk into your centre I always feel enveloped in care and love
All of our volunteers know that what they do, no matter how small contributes to fabric of our service.
Our volunteers give over 10,000 hrs annually to Qld Health to bridge the gap in services and funding. Little Haven’s history of volunteering, support and fundraising not only bears a responsibility to deliver exceptional care, but has helped shape compassion in our community. Gympie has engaged with our vision that it “takes a village to care for their dying” and the ripples of this vision have spread out into the community.
John Rosenberg opened the conference with this theme – the need for connection with communities. Sighting studies from England and Ireland but John need only travel a few hours out of Brisbane to see how organisations that are fed from the ground up are harnessing the energies and support of their communities to show their value for the dying. Regional Queensland is leading the way in community based palliative care.
Pardon my frustration but despite our proven track record of delivering an outstanding model of community based Palliative care with minimal draw on the state-wide Palliative Care funding we struggle to have a voice in the sector. I was recently told by Louise Welch this funding model is antiquated and is only still in place because there would be a community outcry. AND THERE WOULD BE!
Having earned the respect of the community Little Haven in return receives enormous recognition and support locally. We are often told when employers poll their staff about where they would like sponsorship dollars / donations to be directed, Little Haven is unanimously the name put forward.
NGO’s know if you want to draw from the community you need to be responsible with their money and serve that community. It should be no different for Government bodies but there seems a disconnect about where their money comes from.
So what of mum
I drew up a 7 day roster – emailed, group face booked it and asked family and friends to do what they could.
People are amazing and there’s a support network out there – they just needed to be asked and educated on what care was needed and I provide the 24/7 back up they need for reassurance.
The result is 14 months later mum’s still at home, having had a wonderful year where we could all give back to her the love she has given us across the years …. and to quote mum on her last visit to her GP
“So does this mean I’ll have to buy Christmas presents again this year”
In Conclusion
It is beholden on all of us in the palliative care sector to do all we can to treat each and every family facing death with the compassion and respect they deserve. We as a team across the sector – gp’s, hospitals, specialist services, generalist nursing services, aged care facilities and home care services because when we get it right it’s beautiful (as we all like to say – a privilege to be involved in)
Through our advocacy we need to drawer on the enormous capacity of the community to value care of the dying. They already do – they just need to be empowered to know how to do it. Whether it’s filling a family roster or dragging the bin out for a neighbour they barely know but have noticed are unwell.
In educating the care givers and increasing the capacity of community based palliative care services and we can extend our reach into EVERY community.
And we can’t afford to get it wrong. Making services difficult to access, or so clinical in nature they reel away without the warm embrace palliative care should provide.
Families only farewell their father, mother, child once and if we don’t get it right at each and every contact that hurt is hard to undo. If we don’t provide dignity to each and every dying patient we’ll risk losing our voice in the euthanasia debate. The loudest voices in this debate are the carers and families whose loved ones have not died well – or who have not had their grief needs addressed. And who can blame them.
However I could count on my hands the number of patients over the years who actively seek euthanasia at end of life. Is it because they know in our community they will be cared for well at the end of life or is it human natures indefatigable quest for life? Probably both.
Is our model sustainable?
Our history across the years of financial prudence, strong community support, countless volunteer hours given generously and with love and an unswerving commitment to our mission give us a resilience for the challenges that lie ahead. As they say …the stronger the wind, the stronger the tree.
In closing I call on the power brokers in Palliative Care – the Dr William Cairns, John Haberecht’s and Rosenberg’s, Professor Patsy Yates and the likes and our peak body, Palliative Care Qld, and Qld health, to get behind the community based Palliative care providers because frankly we’re frustrated that out of annual 81+ million dollars funding for Palliative Care in Qld, we the community based Palliative care providers get the crumbs from the table.
You don’t have to travel the world looking for the best model of community based Palliative care, it’s here on your doorstep and we need your help to roll this efficient, effective model of care out in every community – because with equitable long term investment into true community based palliative care providers we have the capacity to catch up with the rest of the world in providing dignified end of life care for all Queenslanders.
2024 Update:
In 2022-23 the University of the Sunshine Coast (Unisc) conducted a comprehensive 12 month evaluation of the Community Based Palliative Care Model that Little Haven has developed. In February 2024 that research paper was published in full and can be read and downloaded here.